To evaluate the association between clinical parameters and the diagnosis of progression using VFI (Visual Field Index) and AGIS (Advanced Glaucoma Intervention Study) score in primary open angle glaucoma.
MethodsRetrospective study of 517 visual fields of 78 eyes with primary open angle glaucoma analyzed with VFI and AGIS score. Clinical data registered included: age, sphere, pachimetry, basal intraocular pressure (IOP), and IOP during the follow up.
ResultsOnly the AGIS score diagnosis of progression was associated with the clinical parameters registered. Among the analyzed data, the mean IOP during follow up (p=0.0005) and IOP at the third month of follow up (p=0.004) were statistically associated with progression using the AGIS criteria.
ConclusionThe diagnosis of perimetric progression using the AGIS score in the current study was closer to the real functional progression than the diagnosis using the VFI, as the former was associated with known risk factors for progression in glaucoma.
Evaluar la asociación entre los parámetros clínicos y el diagnóstico de progresión utilizando el Índice del Campo Visual (VFI) y la Puntuación del Estudio de Intervención del Glaucoma en el glaucoma primario de ángulo abierto.
MétodosEstudio retrospectivo de 517 campos visuales de 78 ojos con glaucoma primario de ángulo abierto analizados con VFI y la puntuación AGIS. Los datos clínicos registrados incluyeron: edad, esfera, paquimetría, presión intraocular (PIO) basal y PIO durante el seguimiento.
ResultadosÚnicamente el diagnóstico de la progresión de la puntuación AGIS se asoció a los parámetros clínicos evaluados. Entre los datos analizados, la PIO media durante el seguimiento (p=0,0005) y la PIO al tercer mes de seguimiento (p=0,004) se asociaron estadísticamente a la progresión, utilizando los criterios AGIS.
ConclusiónEl diagnóstico de la progresión perimétrica utilizando la puntuación AGIS en el estudio actual se acercó más a la progresión funcional real que el diagnóstico utilizando el VFI, ya que la primera se asoció a los factores de riesgo conocidos para la progresión del glaucoma.
Glaucoma is a progressive disease in which optic nerve damage may increase in certain patients despite adequate treatment.1 Several strategies are used to detect visual field (VF) damage progression: clinical judgment, event analysis, trend analysis, and defect classification systems.
Brusini and Johnson2 established the features of the ideal system for VF progression detection, i.e., it should be standardized, objective, reproducible, user friendly, supported by scientific and clinical evidence, able to analyze data obtained from different models of perimeters, provide useful information on the characteristics of the VF defects, provide a classification consistent with structural damage data, widely used and accepted, able to monitor even relatively small changes in functional loss over time, and available on computer software for easy day-to-day clinical use. No currently available systems fulfill all these criteria.
There is no gold standard for glaucomatous functional worsening detection that can be used to test the different methods currently available to detect glaucomatous progression.3,4 Thus, if we diagnose perimetric progression in an eye using certain method, absence of progression may be evident in the same eye using another method, and we simply cannot state which of both methods is correct.5 As in any other field, the lack of an accurate method to detect VF progression has led to the development of several methods.5,6 Unfortunately, we do not have adequate knowledge of the ability of each of them to provide useful clinical information.4
Most published studies that have analyzed the ability to detect VF progression arbitrarily chose one of the available methods to detect VF progression against which the new methods were compared.3
Ernest et al.4 proposed a new approach to identify true perimetric progression in the absence of a gold standard. They stated that the detection method that diagnoses progression in eyes with more, well-known glaucoma progression risk factors is the one nearer to the gold standard in perimetric progression detection.
The Advanced Glaucoma Intervention Study (AGIS) score is one of the most specific perimetric progression diagnostic methods that has been reported.7,8 The Visual Field Index (VFI) is an automated method for detecting perimetric progression designed for the Humphrey visual field (Humphrey Visual Fields, Carl Zeiss Inc., Dublin, CA, USA), which has been described elsewhere.9 The VFI calculates the rate of perimetric progression, which is a useful parameter for glaucoma management, according to the more recent recommendations for glaucoma follow-up.1,6 To the best of our knowledge, no studies have compared the perimetric behavior of both systems and their correlation with clinical parameters, including those considered to be risk factors for glaucoma progression.
Materials and methodsPatients with open-angle glaucoma under treatment attending the Glaucoma and Neuro-Ophthalmology Unit of the Hospital Universitario Príncipe de Asturias (Alcalá de Henares, Madrid, Spain) between January and May 2012 were studied retrospectively. All patients had a diagnosis of glaucoma based on the appearance of the optic disc and reproducible perimetric defects characteristic of glaucoma, at least four years of follow-up and five VFs obtained with a Humphrey Visual Field Analyzer II 745 (Carl Zeiss Inc., Dublin, CA, USA).
Patients were excluded if they had a visual acuity (VA) below 20/40, any concomitant pathology that could alter VF measurements, refractive errors over 5.0 diopters or 3.0 diopters of astigmatism and false positives, false negatives, and fixation errors over 25% in their visual fields.
The study was performed in accordance with the 1964 Declaration of Helsinki, and the institutional review board approved the study.
The VFs obtained were Swedish Interactive Threshold Algorithm standard 24-2 VFs with size III stimulus in the Humphrey Visual Field Analyzer Model 745.
From each VF, we obtained the date, results of glaucoma hemifield testing, VFI, mean defect (MD) and its P value, pattern standard deviation (PSD), fixation losses, false negatives, false positives, and glaucoma progression analysis (GPA) alert. All VFs collected were analyzed using the VFI and the AGIS score.
Visual Field IndexBengtsson and Heijl9 described the VFI, which is calculated automatically from the pattern deviation map values, is calculated in such a way that the central points of the VF have more impact on this global index than the peripheral points.
The VFI was calculated for each VF and had a value that ranged from 100% for a normal VF to 0% for a completely abolished VF. In addition, the GPAII analysis software calculates the linear regression of all VFI values from the same eye and provides the estimated change in the VFI expected for the next three to five years. The results are shown on a VFI diagram and a VFI bar graph. We considered that eyes had perimetric progression when the VFI progression rate was statistically significant.
The VFI-related information collected in the current study was the annual percentage decrease in VFI, its standard deviation, and its P value.
AGIS scoreThe AGIS score,10 developed to detect perimetric progression during the Advanced Glaucoma Intervention Study (AGIS), is based on the analysis of the 24-2 area of the VF subdivided into three areas: nasal, superior, and inferior. The scores for each of these areas are calculated from the total deviation map values and, depending on the location, the decibel loss that is considered abnormal ranges from 5 to 9. The score for each VF ranges from 0 (no VF damage) to 20 (terminal glaucoma). Perimetric progression is diagnosed when an increase in the AGIS score of four or more points is detected in three successive VF measurements.
Clinical dataWe collected the following data from the medical records: the more damaged eye, age, gender, date when the VF examination was performed, date of the visit to the office, family history of glaucoma, refraction, pachymetry, number of treatments, visual acuity (VA), and intraocular pressure (IOP). From this raw data, we calculated the average IOP, percent IOP decrease every 12 months, percent IOP decrease between the first and the last IOP measurements, and the average percent IOP decrease.
Statistical analysisStatistical analysis was performed using Statview SE+Graphics (Abacus Concepts Inc., Berkeley, CA) using a Macintosh PowerBook 1400cs/117 (Apple Computer Inc., Cupertino, CA).
We used the Kolmogorov–Smirnov test to evaluate the normality of our data. The continuous variables adjusted to normality were expressed as the mean and the standard deviation. An unpaired t-test adjusted by the Bonferroni correction for multiple comparisons was used to compare the perimetric and clinical data of eyes with and without perimetric progression. The level of significance was established at P<0.05.
ResultsWe obtained 517 VFs from 78 eyes (42 left eyes, 36 right eyes) of 46 patients (27 males, 58.7% of our sample). The same investigator (JGO) analyzed each VF using the AGIS score. The mean follow-up time was 7.63±2.07 years (range, 4.33–14.67 years).
More basal clinical and perimetric data are shown in Tables 1 and 2, respectively.
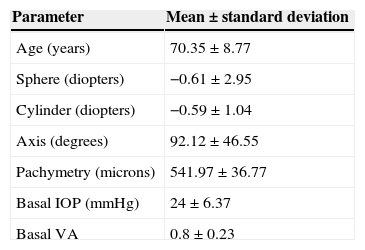
Basal clinical data of our population.
| Parameter | Mean±standard deviation |
|---|---|
| Age (years) | 70.35±8.77 |
| Sphere (diopters) | −0.61±2.95 |
| Cylinder (diopters) | −0.59±1.04 |
| Axis (degrees) | 92.12±46.55 |
| Pachymetry (microns) | 541.97±36.77 |
| Basal IOP (mmHg) | 24±6.37 |
| Basal VA | 0.8±0.23 |
IOP: intraocular pressure; VA: visual acuity; dB: decibels; mmHg: millimeter of mercury.
Basal perimetric data of the study population.
| Parameter | Mean±standard deviation | Range |
|---|---|---|
| Basal VFI (%) | 73.79±23.74 | 14–98 |
| Basal MD (dB) | −9.98±7.41 | −27.88 to 0.09 |
| Basal PSD (dB) | 7.27±4.18 | 1.83–16.88 |
| Basal AGIS | 7.29±5.82 | 0–19 |
| No. of VFs | 6.63±1.49 | 5–16 |
VFI: Visual Field Index; MD: mean deviation; PSD: pattern standard deviation; AGIS: Advanced Glaucoma Intervention Study; VFs: visual fields.
Twenty-nine eyes were diagnosed with perimetric progression using the VFI. The perimetric characteristics of those eyes diagnosed by VFI with perimetric progression compared with those without progression are summarized in Table 3.
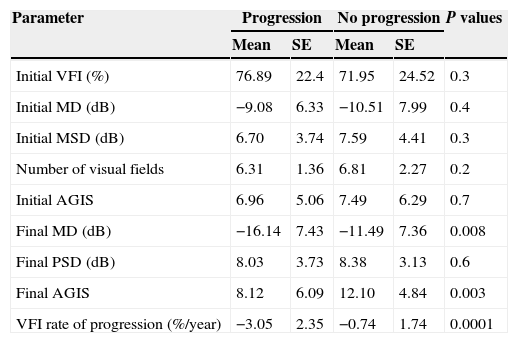
Perimetric characteristics of eyes diagnosed with VFI perimetric progression compared with stable eyes.
| Parameter | Progression | No progression | P values | ||
|---|---|---|---|---|---|
| Mean | SE | Mean | SE | ||
| Initial VFI (%) | 76.89 | 22.4 | 71.95 | 24.52 | 0.3 |
| Initial MD (dB) | −9.08 | 6.33 | −10.51 | 7.99 | 0.4 |
| Initial MSD (dB) | 6.70 | 3.74 | 7.59 | 4.41 | 0.3 |
| Number of visual fields | 6.31 | 1.36 | 6.81 | 2.27 | 0.2 |
| Initial AGIS | 6.96 | 5.06 | 7.49 | 6.29 | 0.7 |
| Final MD (dB) | −16.14 | 7.43 | −11.49 | 7.36 | 0.008 |
| Final PSD (dB) | 8.03 | 3.73 | 8.38 | 3.13 | 0.6 |
| Final AGIS | 8.12 | 6.09 | 12.10 | 4.84 | 0.003 |
| VFI rate of progression (%/year) | −3.05 | 2.35 | −0.74 | 1.74 | 0.0001 |
SE: standard deviation; VFI: Visual Field Index; MD: mean deviation; dB: decibels; PSD: pattern standard deviation; AGIS: Advanced Glaucoma Intervention Study; VFs: visual fields.
The behavior of the clinical data studied during the follow-up period and correlated with the VFI diagnosis of perimetric progression is summarized in Table 4.
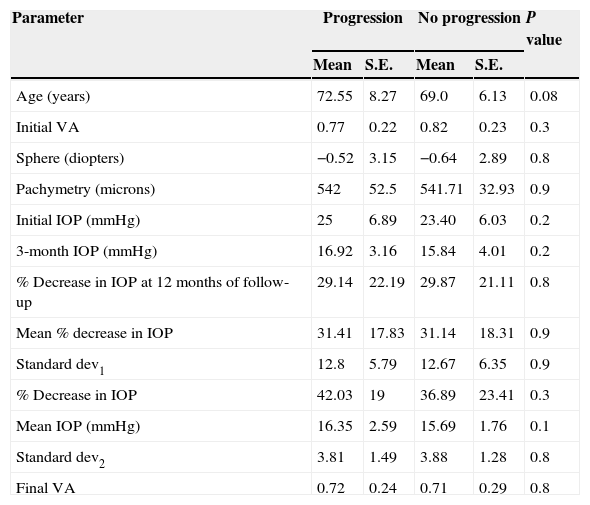
Clinical data from eyes diagnosed with VFI perimetric progression compared with stable eyes.
| Parameter | Progression | No progression | P value | ||
|---|---|---|---|---|---|
| Mean | S.E. | Mean | S.E. | ||
| Age (years) | 72.55 | 8.27 | 69.0 | 6.13 | 0.08 |
| Initial VA | 0.77 | 0.22 | 0.82 | 0.23 | 0.3 |
| Sphere (diopters) | −0.52 | 3.15 | −0.64 | 2.89 | 0.8 |
| Pachymetry (microns) | 542 | 52.5 | 541.71 | 32.93 | 0.9 |
| Initial IOP (mmHg) | 25 | 6.89 | 23.40 | 6.03 | 0.2 |
| 3-month IOP (mmHg) | 16.92 | 3.16 | 15.84 | 4.01 | 0.2 |
| % Decrease in IOP at 12 months of follow-up | 29.14 | 22.19 | 29.87 | 21.11 | 0.8 |
| Mean % decrease in IOP | 31.41 | 17.83 | 31.14 | 18.31 | 0.9 |
| Standard dev1 | 12.8 | 5.79 | 12.67 | 6.35 | 0.9 |
| % Decrease in IOP | 42.03 | 19 | 36.89 | 23.41 | 0.3 |
| Mean IOP (mmHg) | 16.35 | 2.59 | 15.69 | 1.76 | 0.1 |
| Standard dev2 | 3.81 | 1.49 | 3.88 | 1.28 | 0.8 |
| Final VA | 0.72 | 0.24 | 0.71 | 0.29 | 0.8 |
IOP: intraocular pressure; VA: visual acuity; SE: standard deviation; 3-month IOP: IOP at third month of follow-up; mean % decrease in IOP: mean % IOP decrease during follow-up; standard dev1: standard deviation of the mean % IOP decrease during follow-up; % decrease in IOP: % IOP decrease from initial to final examinations; standard dev2: standard deviation of the mean IOP values during follow-up.
Seventeen eyes were diagnosed with perimetric progression using the AGIS score. The perimetric characteristics of eyes with perimetric progression compared with those without progression are summarized in Table 5.
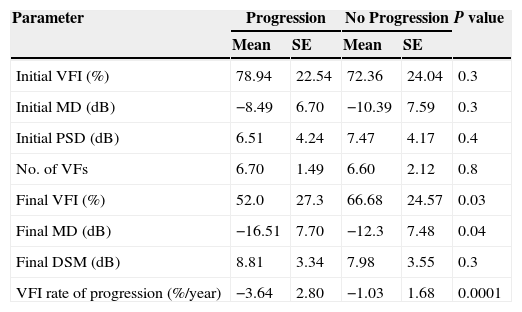
Perimetric characteristics of eyes diagnosed with AGIS score perimetric progression compared with stable eyes.
| Parameter | Progression | No Progression | P value | ||
|---|---|---|---|---|---|
| Mean | SE | Mean | SE | ||
| Initial VFI (%) | 78.94 | 22.54 | 72.36 | 24.04 | 0.3 |
| Initial MD (dB) | −8.49 | 6.70 | −10.39 | 7.59 | 0.3 |
| Initial PSD (dB) | 6.51 | 4.24 | 7.47 | 4.17 | 0.4 |
| No. of VFs | 6.70 | 1.49 | 6.60 | 2.12 | 0.8 |
| Final VFI (%) | 52.0 | 27.3 | 66.68 | 24.57 | 0.03 |
| Final MD (dB) | −16.51 | 7.70 | −12.3 | 7.48 | 0.04 |
| Final DSM (dB) | 8.81 | 3.34 | 7.98 | 3.55 | 0.3 |
| VFI rate of progression (%/year) | −3.64 | 2.80 | −1.03 | 1.68 | 0.0001 |
SE: standard deviation; VFI: Visual Field Index; MD: mean deviation; PSD: pattern standard deviation; dB: decibels; VFs: visual fields.
The behavior of the clinical data studied during the follow-up period and correlated with the AGIS score diagnosis of perimetric progression is summarized in Table 6.
Clinical data from eyes diagnosed with AGIS score perimetric progression compared with stable eyes.
| Parameter | Progression | No progression | P value | ||
|---|---|---|---|---|---|
| Mean | SE | Mean | SE | ||
| Age (years) | 71.88 | 9.22 | 69.91 | 8.67 | 0.4 |
| Initial VA | 0.81 | 0.18 | 0.80 | 0.24 | 0.8 |
| Sphere | 0.12 | 3.27 | −0.84 | 2.84 | 0.3 |
| Pachymetry (microns) | 544.57 | 26.26 | 541.25 | 39.35 | 0.7 |
| Initial IOP (mmHg) | 26.11 | 6.03 | 23.01 | 6.38 | 0.1 |
| 3-month IOP (mmHg) | 18.71 | 3.51 | 15.57 | 3.48 | 0.004 |
| % Decrease in IOP at 12 months | 31.81 | 20.55 | 29.01 | 21.71 | 0.6 |
| Mean % decrease in IOP | 32.58 | 13.26 | 30.86 | 18.45 | 0.7 |
| Standard dev1 | 13.05 | 5.23 | 12.52 | 6.15 | 0.7 |
| % Decrease in IOP | 46.05 | 20.47 | 36.78 | 22.39 | 0.1 |
| Mean IOP (mmHg) | 17.47 | 2.58 | 15.51 | 1.76 | 0.0005 |
| Standard dev2 | 3.90 | 1.42 | 3.84 | 1.34 | 0.9 |
| Final VA | 0.70 | 0.29 | 0.73 | 0.25 | 0.7 |
IOP: intraocular pressure; VA: visual acuity; SE: standard deviation; 3-month IOP: IOP at third month of follow-up; mean % decrease in IOP: mean % IOP decrease during follow-up; standard dev1: standard deviation of the mean % IOP decrease during follow-up; % decrease in IOP: % IOP decrease from initial to final examinations; standard dev2: standard deviation of the mean IOP values during follow-up.
The diagnosis of perimetric progression using the AGIS score in the current study was closer to the actual functional progression than the diagnosis of perimetric progression using the VFI, as the former was correlated with worst IOP levels during the follow-up period.
We have evaluated the validity of two different procedures for the diagnosis of perimetric progression studying simultaneously how clinical data behave during a certain period of time.
The validity of a measurement system is defined as the ability to measure the desired parameter.11 The most common validity studies are statistical studies, with results obtained from the sensitivity, specificity, odds ratios, and positive and negative predictive values. The prerequisite for those parameters calculation is the presence of a gold standard.11 Nevertheless, there is no gold standard among the available procedures to evaluate perimetric progression.4
From the clinimetric point of view, the validity can be evaluated by comparison with the clinical data, what is termed “construct validity.”4,11 Some authors4 believe that this kind of study should be conducted instead of studies that compare different systems of perimetric progression, where one system is selected as the reference system against which the other detection methods are compared.
The glaucoma risk factors used to evaluate the validity of the VFI and the AGIS score were selected based on the literature search. Regarding the IOP, the following parameters have been defined as risk factors for glaucoma perimetric progression: mean IOP,12,13 IOP fluctuations14 (standard deviation of the mean IOP in the current study), and initial IOP.15 In addition, age,13,14 central corneal thickness,12 and myopia16 are possible risk factors for glaucoma progression.
The AGIS score is probably one of the most specific systems used to diagnose perimetric progression. In addition to the fact that it was the system used by the AGIS investigators7 to diagnose progression, this method has been compared to other tools used to evaluate perimetric progression.12 Based on the current results, the estimation of the functional loss using the AGIS score was closer to the actual perimetric progression than the estimation provided by the VFI software.
When the effect of the initial perimetric features on perimetric progression was studied, none of the studied parameters were associated with progression with either the VFI or AGIS score.
Although our sample differed from those studied in large glaucoma trials,14,17 the current results agree with the Collaborative Normal Tension Glaucoma Study17 and differ from the results obtained in the Early Manifest Glaucoma Trial,18 the Collaborative Initial Glaucoma Treatment Study,19 and AGIS.14 The last 14 is the only glaucoma trial that reported that a better VF at the beginning of the follow-up period was a risk factor for progression. The same authors that described this association have not been able to explain it, however, this association disappears when other software for perimetric progression is used. The authors proposed that this fact was an intrinsic consequence of the AGIS score algorithm.
Compared with other cohorts studied with the VFI, Rao et al.20 found an association between the initial perimetric damage measured by the MD and Pattern Standard Deviation (PSD) and the rate of progression in the groups with initial and advanced glaucoma but not in the group with moderate glaucoma, in a group with similar perimetric damage than our sample. Bengtsson et al. also reported that there was no correlation between the initial VFI and the rate of progression,21 although they also found a high correlation between the estimated and the actual progression rates.
The absence of substantial differences in the number of VFs between patients with progressing glaucoma and those who are stable eliminates a possible confounding factor as Nouri-Mahdavi et al. reported that a higher number of VF examinations leads to a higher rate of diagnosis of perimetric progression mainly in trend-based systems.22
The diagnosis of perimetric progression using the VFI is associated with perimetric damage at the end of the follow-up period, quantified by the MD and the AGIS score. However, because the MD and the diagnosis of perimetric progression evolved in the same direction (i.e., the mean MD is worst at the end of the follow-up period), the AGIS score runs in the opposite direction, with those diagnosed with VFI perimetric progression having a better final AGIS score.
Kimura et al.23 studied the relationship between the VFI and MD and found a significant correlation between both parameters. Moreover, Cho et al.24 reported that this correlation did not depend on the level of perimetric damage.
The diagnosis of progression using the AGIS score was significantly associated in the current study with the perimetric parameters at the end of the follow-up period (final VFI, final MD, and percent decrease in VFI/year), excluding the PSD.
We did not found any study that evaluated the correlation between the diagnosis of perimetric progression using both the AGIS score and VFI in the same group of patients.
Regarding the results of the current study, with the VFI diagnosis of progression running in the opposite direction of the final AGIS score and the AGIS Score diagnosis of perimetric progression associated with most of the final perimetric parameters (including the VFI rate), it is plausible that both systems measure slightly different things. Another hypothesis for the origin of this divergence might be caused by an inadequate design of the algorithm for the statistical significance of the VFI trend. The VFI rate statistical significance is estimated in a mathematical way, in other words, using a 95% confidence interval (CI) of the linear regression of the available VFs.9 Some authors5 proposed the addition of the CI when obtaining rates of progression of perimetric damage, a recommendation that has been followed by the designers of the VFI. We believe as others do25 that this might be inadequate, and that the VFI software lacks a database of normal VFI loss per year against which the rates of progression obtained should be compared to flag them as pathological.
Our results are limited mainly by two reasons: the low number of patients enrolled and also by the difficulties in using the AGIS Score in a clinical environment as its calculation is certainly time consuming and may be useful only for research purposes.
In conclusion, in the current study, the diagnosis of perimetric progression using the AGIS score is nearer to the actual functional progression than the diagnosis of perimetric progression using the VFI. Nevertheless, more studies are needed to increase the level of certainty when diagnosing glaucomatous progression.
FundingThis research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Conflicts of interestThe authors cited above have no significant competing financial, professional or personal interests that might have influenced the performance or presentation of the work described in this manuscript.