To evaluate the temperature rise of human cornea during trans-epithelial photorefractive keratectomy (trans-PRK) with a 750Hz excimer laser employing Intelligent Thermal Effect Control (ITEC) software.
MethodsIn this observational case series, trans-PRK ablation was performed on 5 eyes of 3 patients using an aspheric profile of a 750Hz excimer laser system. A high-resolution infrared camera with a frame-rate of 350 images per second was used to determine the corneal surface temperature. Images were taken sequentially, starting a few seconds prior to and ending a few seconds after the ablation. The maximum temperature of any pixel of a given image were recorded and graphed against time.
ResultsThe baseline ocular surface temperature, immediately prior to the beginning of excimer laser, ranged from 32 to 34.9°C. The maximum ocular surface temperature until the epithelium was ablated ranged from 35.2 to 39.7°C. The maximum ocular surface temperature during stromal ablation with high and low fluence laser ranged from 32.9 to 36.5 and from 34.4 to 37.7°C respectively.
ConclusionThe ITEC software is effective in controlling the maximum temperature rise during laser ablation in the extremely challenging situation of trans-PRK involving high ablation volumes of almost 6000nl, potentially improving the outcomes. The ITEC system limited the maximum temperature to 39.7°C in the epithelium, and 37.7°C in the stroma. The epithelial temperature was always higher than stromal temperature (regardless of high or low fluence irradiation). Safety limit of 40°C found in the literature was never reached.
Evaluar el aumento de temperatura de la córnea humana durante la queratectomía transepitelial fotorrefractiva (trans-PRK) con láser excimer de 750Hz, utilizando software para el control inteligente del efecto térmico (ITEC).
MétodosEn esta serie de casos observacional, se practicó ablación Trans-PRK en 5 ojos de 3 pacientes, utilizando un perfil asférico de un sistema láser excimer de 750Hz. Se utilizó una cámara de infrarrojos de alta resolución con 350 fotogramas por segundo para determinar la temperatura de la superficie corneal. Las imágenes se tomaron de forma secuencial, iniciándose unos pocos segundos antes de la ablación y finalizando unos pocos segundos tras la misma. Se registró la temperatura máxima de cada pixel de una imagen dada, realizándose un gráfico con respecto al tiempo.
ResultadosLa temperatura basal de la superficie ocular, inmediatamente antes del comienzo de la aplicación del láser excimer, osciló entre 32°C y 34,9°C. La temperatura máxima de la superficie ocular, hasta la ablación del epitelio, osciló entre 35,2°C y 39,7°C. La temperatura máxima de la superficie ocular durante la ablación del estroma con láser de alta y baja fluencia osciló entre 32,9°C y 36,5°C y entre 34,4°C y 37,7°C, respectivamente.
ConclusiónEl software ITEC es efectivo para controlar el aumento de la temperatura máxima durante la ablación por láser en la compleja situación que acontece durante el procedimiento de trans-PRK, implicando volúmenes de alta ablación de cerca de 6000 nl, y mejorando potencialmente los resultados. El sistema ITEC limitó la temperatura máxima a 39,7°C en el epitelio, y a 37,7°C en el estroma. La temperatura epitelial fue siempre superior a la temperatura estromal (independientemente de la irradiación de alta o baja fluencia). No se alcanzó nunca el límite de de seguridad de 40°C descrito en la literatura.
Temperature of the cornea is a function of the equilibrium of heat transfer between cornea and the surrounding tissues or atmosphere and therefore, any change that affects heat loss or gain may affect its temperature.1–3 The normal corneal surface temperature has been reported to range from 32.9 to 36°C.4 During excimer laser ablation, every single pulse adds heat to the cornea and contributes to the marginal increase in the local corneal temperature.5 Since the laser refractive surgery is based on the sequential delivery of multiple laser pulses, each one ablating a small amount of corneal tissue and causing a marginal increase in the local corneal temperature around the laser spot, excimer laser treatments, on the whole, may cause a significant increase in corneal temperature especially as the heat generation exceeds the heat dissipation during the laser treatment.5
The overall temperature rise on the cornea during laser ablation has been associated with the total number of excimer laser spots applied, radiant energy used and repetition rate of the laser system.6 Since the number of laser spots increase with higher refractive corrections or use of aspheric or wavefront guided ablation profiles,7 the overall temperature rise may increase, especially when such treatments are performed with smaller spot sizes and using high frequency laser systems.6 Although heat shock proteins may limit thermal damage after excimer laser ablation,8,9 it is essential to maintain corneal temperature within safe limits through the duration of excimer laser ablation as an increase in corneal temperature higher than 40°C may denaturize collagen proteins causing reduced refractive outcomes, tissue damage and complications.7,10
Measures to enhance heat dissipation have been traditionally used to keep the corneal temperatures within safe limits. Maintaining LASIK procedure room temperatures within the recommended limit (typically between 18 and 24°C) facilitates the transfer of heat from cornea to the cooler surrounding air.11 Cooled/chilled balanced salt solution (BSS) has also been used to cool the cornea prior,12–14 during13,15 and immediately after12–15 the excimer laser ablation. However, these traditional measures of enhancing heat dissipation are not adequate for the high repetition rate excimer lasers, which significantly decrease the time interval between laser pulses on the same area of the cornea, potentially increasing thermal load on the cornea.16
Early in the development of the scanning spot excimer laser systems, manufacturers (e.g., Autonomous Technologies Corporation (ATC) LADARVision (Orlando, FL) chose to use random spot sequence to decrease the overall thermal load on the cornea and obtained good visual outcomes.17 Optimal spatial and temporal separation of laser pulses has been hypothesized to provide enough time for each area on the cornea to cool between laser pulses thereby minimizing the effective thermal load on the cornea.6,18 Therefore, optimized algorithms that minimize temporal or spatial overlapping of laser pulses to avoid unnecessary local thermal load during high-repetition-rate corneal laser surgery were developed.5,7 “Intelligent Thermal Effect Control (ITEC)” software (SCHWIND eye-tech-solutions, Kleinostheim, Germany) employs a locally blocking algorithm which limits the local frequency to 39Hz while still achieving an overall high repetition rate of 500, 750 or 1050Hz depending on the system repetition rate.
The purpose of the current paper is to evaluate the efficacy of ITEC algorithm to limit the temperature rise of human cornea within safe threshold during excimer laser refractive surgery using 750Hz Amaris excimer laser system. To the best of our knowledge, this is the first paper to clinically document ocular surface temperature changes at high repetition rate of 750Hz (Previous clinical studies have documented temperature changes up to 500Hz).7,10 In addition, this is the first study to use a high resolution infrared thermal camera with a high frame-rate of 350 images per second allowing capture of thermal images after almost every other laser spot (previous studies have used much lower frame rates of up to 50 frames per second).6,7,18,19
MethodsIn this prospective, observational case series, a high-resolution infrared camera was used to monitor the corneal surface temperature changes in 5 eyes of 3 patients (2 females and 1 male) which underwent trans-PRK ablation using an aspheric profile of a 750Hz excimer laser system (Amaris 750S, SCHWIND eye-tech-solutions, GmbH, Kleinostheim, Germany). Informed consent was obtained from the subjects after explanation of the nature and possible consequences of the study.
The Amaris excimer laser system used in this study works at an overall repetition rate (total amount of pulses delivered per second) of 750Hz and produces a spot size of 0.54-mm full width at half maximum with a super-Gaussian ablation spot profile. The eye tracker works at 1050Hz frame rate and compensates for lateral movements as well as for pupil, iris, and limbus tracking with a latency time of typically 3ms. Amaris employs “Intelligent Thermal Effect Control (ITEC)” software to automatically control the local frequency during delivery of the pulse sequence so as to limit the temperature load in a local area. The local frequency as defined in previous publications is the maximum rate at which a particular corneal location may be hit twice20; i.e., a maximum local frequency of 40Hz would mean a minimum local time of 25ms. The ITEC is based on prevention of laser pulses being too often consecutively shot at the same area on the cornea. Positions that have recently received a shot as well as their surrounding area are blocked. Then the algorithm arbitrarily searches for positions on the cornea that are not blocked. Hence there is enough time for each area on the cornea to cool down between laser pulses.5 As heat dissipates to the surrounding corneal tissue and adjacent atmosphere, blocked zone becomes smaller and following laser pulses are able to move closer more quickly to the position of the last laser pulses. In this manner, the local spot frequency is dynamically limited without significantly affecting the overall laser pulse frequency.
A pre-calibrated high-resolution infrared camera (VarioCAM®hr; InfraTec GmbH, Dresden, Germany), with calibration and emissivity analogous to previous publications,5,7,18,20–22 was used to determine the corneal surface temperature. It employed a microbolometer-FPA detector to measure temperature within the spectral range of 2.0–5.5μm thermal resolution of ±0.02K and measurement accuracy of ±1%. The camera provided thermal images of 640×512 infrared pixels at a repetition rate of 350 images per second for the entire cornea. This camera was cryobolometric so that it enabled full frame (corresponding to 15×15mm field of view) even at high acquisition rates. Within each laser spot, there were more than 500 pixels providing more than 500 discrete temperature readings. The images, thus obtained, were analyzed with the help of an analysis software, Irbis 3.0 professional (InfraTec GmbH, Dresden, Germany).
The environmental conditions of the operating room were controlled to the standard temperature of 23±1°C and humidity of 28±1% (measured with a standard hygro-thermometer). Since the dimensions of the excimer laser device did not allow a perpendicular positioning, the infrared camera was placed on the surgeon's left side at a 45° angle, 66cm away from the ocular surface to allow the surgeon with reasonable space to perform surgical maneuvers. Images were taken sequentially, starting a few seconds prior to the first laser pulse and ending a few seconds after the ablation. For every image, obtained using the above described setup, the maximum and mean temperatures of a given image were calculated and recorded. The temperature measurement immediately prior to the beginning of ablation was determined to be the baseline temperature. Maximum ocular surface temperature of any pixel of an image were plotted against time (corresponding to that image) to provide a graphical representation of the progression in corneal surface temperature, as it changes through the duration of the ablation. Surface temperature readings during epithelial and stromal ablation (high and low fluence) were reported separately, for which treatment logs provided by the AMARIS were analyzed a posteriori to determine precise timings of epithelial/stromal (high and low fluence) ablation.
Refractive errors included a mix of myopia and hyperopia, with and without astigmatism, so that the area of highest number of pulses varied – centrally as well as peripherally; however, since all the ablations were trans-PRK, majority of the pulses were used to ablate epithelium.
ResultsThe mean age of 3 subjects was 43.3±7.3 years (range 33–49 years). The baseline mean ocular surface temperature immediately prior to the beginning of excimer laser ranged from 32.1 to 34.9°C (Table 1). For an ablation volume ranging from 3628 to 5949 nano-liter (nl), the maximum ocular surface temperature during epithelial ablation ranged from 35.2 to 39.7°C (Table 1). The maximum ocular surface temperature during stromal ablation with high and low fluence excimer laser ranged from 32.9 to 36.5 and from 34.4 to 37.7°C respectively (Table 1). Optical zone was 7.25mm in 2 eyes and to 7.5mm in 3 eyes; total ablation zone ranged from 7.86 to 8.96mm diameter. Maximum Ablation time was 41s and maximum ablation depth was 128μm. All treatments were uneventful and no interruption of the pulse sequence occurred.
Ablation parameters and temperature changes for five eyes of three patients that underwent trans-PRK.
| Eye | Refraction | Ablation parameters | Corneal temperature (°C) | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Patient no./eye laterality | Manifest refraction | MRSEa | Optical zone (mm) | Total ablation zone (mm) | Depth of ablation (μm) | Ablation time (s) | Ablative volume (nl) | Baseline (mean) | Maximum temp. epithelium | Maximum temp. stroma HFb | Maximum temp. stroma LFc |
| 1/OD | −0.75/−0.75×5° | −1.125 | 7.25 | 7.86 | 87 | 26 | 3628 | 34.9 | 38.9 | 36.5 | 37.7 |
| 1/OS | +0.75/−3.00×165° | −0.75 | 7.25 | 8.53 | 128 | 39 | 5406 | 32.1 | 39.7 | 36.2 | 36.0 |
| 2/OD | +1.25 | 1.25 | 7.5 | 8.16 | 92 | 25 | 4159 | 32.5 | 35.8 | 32.9 | 34.4 |
| 2/OS | +1.5 | 1.5 | 7.5 | 8.30 | 98 | 27 | 4509 | 33.1 | 35.2 | 34.8 | 35.9 |
| 3/OD | −1.00/−1.5×14° | −1.75 | 7.5 | 8.96 | 115 | 41 | 5949 | 32.7 | 38.0 | 35.4 | 36.1 |
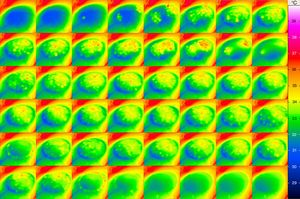
Fig. 1 demonstrates a series of infrared thermographic images of the left eye of patient 1 showing the temperature distribution on the ocular surface. The first two images in the upper left corner of the first row show the distribution of ocular surface temperature immediately prior to ablation, with temperature of most of the cornea to be around 31–32°C. The next image demonstrates the image of the ocular surface immediately after the first pulse. With the high resolution of the infrared camera, consecutive laser spots can be viewed easily. The subsequent images demonstrate the temperature distribution on the corneal surface as ablation progresses. The area of ablation and corresponding area of warming can be seen. The temperature scale, common for all images, is depicted on the right. Highest thermal points showed bright red spots corresponding to approximately 37°C.
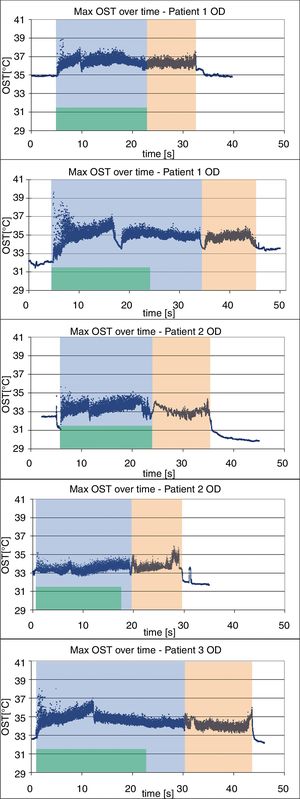
Fig. 2 demonstrates the change in maximum corneal surface temperature over time for all 5 eyes individually. Maximum surface temperature during the epithelial ablation was 39.7°C (Fig. 2 Patient 1 OS) and in stroma was 37.7°C (Fig. 2 Patient 1 OD). After a quick increase, maximum temperature rise plateaued within the first few seconds of epithelial ablation, with the majority of the values remaining within 2 and 4°C of the baseline through the duration of the ablation. After the ablation ended, ocular surface cooled down with maximum corneal temperature decreasing quickly.
Maximum ocular surface temperature (OST) versus ablation time for all the 5 eyes (Green area demonstrates epithelial ablation; blue area demonstrates ablation under high fluence and pink area demonstrates ablation under low fluence). In Patient 1 OS, the treatment was interrupted two times due to re-centration of eye and surgical maneuvers, which corresponds to the drop in temperature at two places in the graph.
Excimer laser has conventionally been considered a ‘cold’ laser5,7,20; however, development of high frequency excimer laser systems necessitated a re-examination of the basics of this concept. In essence, each pulse of excimer laser adds heat to the cornea and contributes to the marginal increase in the local corneal temperature; however, since thermal relaxation time of the molecules is usually shorter than the thermal denaturation time, heat dissipates quickly.10,23 As the frequency of excimer laser system increases, consequent pulses add more heat before thermal load from the preceding ones dissipates.6 Therefore, there is a need to develop appropriate methods to limit the corneal temperature rise during ablation with high frequency laser systems.
While chilled BSS is known to increase heat dissipation,8,13,15 increasing repetition rate of the newer excimer laser systems necessitate that innovative methods be developed to control the heat produced. To evaluate the effect of temporal and spatial positioning of laser pulses (1050Hz) on the temperature rise, Mrochen et al. studied 4 spot sequences – line, circumferential, random, and optimized – and found significant variation in maximum temperature rise during ablation with different algorithms.6 They found that scan sequences that allow higher degree of temporal and spatial overlapping led to higher temperatures than spot sequences that avoided or minimized such overlapping. Compared to the circumferential scan that resulted in a maximum temperature rise of more than 23°C for −9D ablation, spot sequence optimization decreased the maximum temperature rise to 15.36°C; yet it was not sufficient to perform high frequency excimer laser procedures safely. Therefore, there is a need to device ways to further limit the maximum increase in temperature rise with high frequency excimer lasers.
ITEC is a unique thermal control system that considers all aspects of the dynamics of the heat propagation in the cornea while using a high laser pulse frequency and two energy levels. ITEC minimizes the thermal load on the cornea by blocking small areas around the laser spots for longer intervals and wider areas for shorter intervals.5,7,21,24 Therefore, instead of ablating the corneal tissue in layers, the pulse positions are chosen arbitrarily based on whether a position is blocked or not. This ensures a thermally optimized, dynamically adapted distribution of laser pulses during treatment, meaning that there is always enough time for each area on the cornea to cool between laser pulses.
Current study was designed to measure the thermodynamic changes of cornea and therefore, evaluate the effectiveness of ITEC system in a high frequency excimer laser system of 750Hz (Amaris 750S) in the most challenging ablation needs, i.e., during trans-PRK.21 Ablation volume differs with respect to refractive error, optical zone and type of ablation (Table 2). While ablation volume for refractive correction of −10D, 6mm optical zone PRK is far less at 2512nl, the corresponding figure for trans-PRK is 5733nl. Even when trans-PRK is performed only for epithelial ablation, that is 0 D correction, the ablation volume for a 7.5mm optical zone may be as high as 2780nl. In LASIK or PRK, after flap creation or mechanical/alcohol-assisted epithelial debridement, the total ablation volume corresponds to the stromal ablation required to correct the refractive error; however, in trans-PRK, total ablation volume corresponds to the stromal ablation required to correct the refractive error as well as epithelial ablation. Since the epithelium is more sensitive than stroma (i.e., a laser pulse with same energy yields deeper ablation in epithelium than in stroma) and the parameters used in the ablation algorithm are dedicated for stromal ablation,22 a higher temperature rise of about 1–2°C is expected during epithelial ablation. Therefore, for a given refractive error and optical zone, due to much higher ablation volume of trans-PRK than LASIK or PRK and due to inherent properties of epithelium, there is a possibility of more temperature rise during the epithelial ablation in trans-PRK. While it would have been ideal to perform such a study in comparison to a control group, i.e., trans-PRK performed with a laser platform without ITEC; however, ethically such a study cannot be performed clinically due to the very well expected thermal damage to the human cornea in the control group.10,25,26
Estimated ablation depth and ablative volume for a given refraction during PRK and trans-PRK.
| Refraction (D) | Optical zone (mm) | PRK | TransPRK | ||
|---|---|---|---|---|---|
| Central ablation depth (μm) | Ablative volume (nl) | Central ablation depth (μm) | Ablative volume (nl) | ||
| −10 | 6 | 132 | 2512 | 187 | 5733 |
| −5 | 6 | 66 | 1088 | 121 | 3487 |
| −1 | 6 | 14 | 200 | 69 | 1978 |
| 0 | 6 | –a | – | 55 | 1753 |
| 0 | 6.5 | – | – | 55 | 2065 |
| 0 | 7 | – | – | 55 | 2411 |
| 0 | 7.5 | – | – | 55 | 2780 |
The maximum temperature rise during trans-PRK ablation, as found in our study, is lower than that demonstrated in previous studies. As such, the data of current study (with temperature measurement in human eyes) may not be directly comparable with the previous studies that have used bovine and ovine corneas; yet we have presented such comparisons in order to provide an overall indication of the safety and effectiveness of the ITEC algorithm in a much more challenging situation of trans-PRK than reported in previous studies. Maldonado-Codina et al. evaluated the temperature changes in ovine corneas during PRK ablation using a scanning and rotating slit micro-beam with repetition rate of 30Hz and found that the mean temperature rise was 7.35±1.13°C with a maximum temperature rise of 8.97°C for a refractive correction of −8D and an ablation depth of 113.6μm.27 Mrochen et al. investigated the influence of temporal and spatial spot sequences using a high-repetition rate excimer laser with 1050Hz in bovine corneas. Using the most optimized scan algorithm, they observed a maximum temperature rise of 15.36±0.14°C for −9.00D and 12.24±0.14°C for −3.00D myopia treatment.6
In contrast to Mrochen et al. and Maldonado-Codina et al., de Ortueta et al. demonstrated significantly less temperature rise of 3.73°C in human corneas,7 which was attributed to the use of Intelligent Thermal Effect Control (ITEC) software. Corresponding to a maximum temperature rise of 3.73°C, found by de Ortueta et al. with a 500Hz excimer laser for an estimated ablation volume of ∼2500nl, current study found a maximum temperature change of 4.1°C (from 32.1 to 36.2°C) during high fluence stromal ablation of an eye with ablation volume of 5406nl using higher frequency excimer laser equipment of 750Hz, but same local frequency as used by de Ortueta et al. Further, in the current study, we explored the temperature rise in significantly more challenging situations, that is, eyes with ablation volumes ranging from more than 3500nl to nearly 6000nl which, as described above, is possible with trans-PRK; still the maximum temperature rise was limited to 7.6°C in the epithelium (from 32.1 to 39.7°C) and 4.1°C (from 32.1 to 36.2°C) in the stroma (both maximum changes occurred for the same procedure). It is important to note that no pre/intra/post-operative cooling of the cornea was utilized in the current study. The rise in maximum temperature found in the current study in human cornea is much lower than that the maximum temperature rise of 15.36°C reported by Mrochen et al. in enucleated bovine corneas using the most optimized scan of a 1050Hz excimer laser system.6
We observed that ITEC limited the rise of the maximum ocular surface temperature, with the use of high frequency 750Hz excimer laser. The change in maximum ocular temperature was limited to 4.1°C (from 32.1 to 36.2°C) in the stroma. Although trans-PRK was performed in all 5 eyes in the current study, majority of the refractive surgeons as well as patients globally may prefer either LASIK or PRK instead of trans-PRK. Standard stromal ablation procedures like PRK and LASIK, even when performed for very high myopia are likely to have an ablation volume of less than 3000nl and therefore, maximum temperature rise in the stroma may be limited to ∼4°C when ablated using ITEC software, as demonstrated by de Ortueta et al.7 and also apparent from the current study.
It may be logical to assume that the thermal load of a treatment will depend on the actual repetition rate of the system; however, with local frequency controls in place, as in an ITEC system, the thermal load of a treatment is expected to be independent of the overall repetition rate of the system as long as same local frequency controls are maintained.22 Together with the results of the de Ortueta et al.’s study7 with 500Hz excimer laser and the current study results with 750Hz excimer laser, however with same local frequency, we find that the thermal impact of the ablation remained similar, i.e., ∼4°C. Therefore, it can be hypothesized that as long as the local frequency of the laser system is maintained below 40Hz, further increase in the overall repetition rates (e.g., 1050Hz), may not affect the temperature rise as thermal load may remain similar to excimer lasers with overall frequency of 500 or 750Hz. However, future studies may provide appropriate data to validate this hypothesis.
It is important to observe that, in the current study, the ocular surface temperature was measured using a high speed infra-red camera with a frame-rate of 350 images per second and a 750Hz excimer laser, i.e., the camera was capable of capturing almost every second pulse. This is important as the highest frame rate of the camera reportedly used in similar experiments till date was 50 frames per second.6,7,18,19 Despite the high speed, high resolution and high accuracy of the infrared camera, errors in the measurements and inferences may appear from the errors in the estimation of the emissivity factor of human cornea (∼0.9), estimation of the change of the emissivity factor of human corneas with the corneal curvature, viewing angle of the camera, precise position of the eye as the eye moves during measurement, etc. These aspects of such an experimental setup have been studied elsewhere under well controlled conditions of porcine corneas.18 Another factor which might have affected the readings of the camera are the rotationally non-symmetric ablation profiles, which were also used for astigmatic corrections in this study. However, the camera position was “far enough” as to provide full frame view of the cornea (of course at different angles due to the dome shape of the cornea) and close to 45 degrees angle. A corneal toricity of 2–3D related to a normal cornea of 40-45D mean curvature just represents ∼6%. So, the added effect for toricity shall be minor compared to the dome effect of the mean curvature. The study was designed to capture and analyze the maximum temperature per image. While a previous porcine eye study has analyzed mean temperature rise±SD of all pixels pertaining to cornea,18 it was not possible to study it clinically in a moving eye due to the technical limitation of absence of a tracking software in the infrared camera.
The current study found that using ITEC software, the maximum temperature rise during high frequency laser ablation in the extremely challenging situations of trans-PRK was still on the safe side of the thermal load. Despite the extremely challenging situation of trans-PRK with high ablation volumes ranging from 3500 to 6000nl, the ITEC system limited the rise in maximum ocular surface temperature rise to 7.6°C in the epithelium and 4.1°C in the stroma. Maximum temperature during epithelial ablation was always below 40°C and during stromal ablation was always lower than epithelium and never exceeded 37.7°C. Standard stromal ablation procedures like PRK and LASIK, even when performed for very high myopia are likely to have an ablation volume of less than 3000nl and therefore, maximum temperature rise may be limited to ∼4°C when ablated using ITEC software.
FundingThis work was supported by SCHWIND eye-tech-solutions.
Conflicts of interestDe Ortueta has no proprietary interest in the materials presented herein. Magnago and Arba-Mosquera are employees of SCHWIND eye-tech-solutions.
Raman Bedi, MD, critically reviewed the manuscript. IrisARC – Analytics, Research & Consulting (Chandigarh, India) provided literature research, writing and editing assistance.