To compare the intraocular pressure (IOP) measurements obtained with the rebound tonometry (RT), dynamic contour tonometry (DCT) and Goldmann applanation tonometry (GAT) in keratoconic corneas and to investigate the effects of central corneal thickness (CCT) and corneal radius of curvature (CR) on IOP measurements.
MethodsSixty-three eyes of 63 keratoconus patients were enrolled in this cross-sectional study. IOP was measured on each subject always in the same order, ICare RT-Pascal DCT-GAT, after a minimum interval of 10min between measurements. CCT and CR were measured using a rotating Scheimpflug camera before the IOP measurements in all subjects. One way repeated measures ANOVA and Pearson correlation coefficient analysis was used for the statistical assessment.
ResultsMean IOP for all enrolled eyes was 11.72±2.59mmHg for GAT, 9.34±3.29mmHg for RT, and 15.42±3.31mmHg for DCT. There were statistically significant differences among the three tonometers; GAT and RT (P<0.001), GAT and DCT (P<0.001), and RT and DCT (P<0.001). GAT and RT were significantly positively correlated with CCT (r=0.288, P=0.025 and r=0.483, P<0.001, respectively). RT was also significantly positively correlated with CR (r=0.550, P<0.001). DCT was not significantly correlated with CCT (r=0.115, P=0.377) nor CR (r=−0.179, P=0.168).
ConclusionsDCT has overestimated but RT has underestimated IOP readings according to GAT measurements in keratoconic corneas. DCT may be the most appropriate tonometer to use in keratoconus for the measurements of IOP, because DCT do not appear to be dependent upon CCT and CR.
Comparar las mediciones de la presión intraocular (PIO) obtenidas con el tonómetro de rebote (RT), el tonómetro de contorno dinámico (DCT) y el tonómetro de aplanamiento de Goldmann (GAT) en córneas con queratocono, e investigar los efectos del espesor central de la córnea (CCT) y los radios de curvatura de la córnea (CR) en las mediciones de la PIO.
MétodosEste estudio transversal se realizó sobre sesenta y tres ojos de un número igual de pacientes con queratocono. Se midió la PIO de cada sujeto siempre en el mismo orden, ICare RT-Pascal DCT-GAT, tras un intervalo mínimo de diez minutos entre mediciones. Las mediciones de CCT y CR se realizaron utilizando una cámara Scheimpflug rotatoria, antes de medir la PIO en todos los sujetos. Se utilizaron los análisis de coeficiente de correlación de Pearson y la ANOVA de una vía de medidas repetidas para realizar la valoración estadística.
ResultadosLa PIO media para todos los ojos estudiados fue de 11,72±2,59mmHg para GAT, 9,34±3,29mmHg para RT, y 15,42±3,31mmHg para DCT. Se produjeron diferencias estadísticamente significativas entre los tres tonómetros; GAT y RT (P<0,001), GAT y DCT (P<0,001), RT y DCT (P<0,001). GAT y RT reflejaron una relación significativamente positiva con CCT (r=0,288, P=0,025 y r=0,483, P<0,001, respectivamente). RT reflejó también una correlación significativamente positiva con CR (r=0,550, P<0,001). DCT no reflejó una correlación significativa con CCT (r=0,115, P=0,377) ni con CR (r=0,179, P=0,168).
ConclusionesEl tonómetro DCT sobreestimó las mediciones de la PIO, y el RT subestimó las mismas, con arreglo a las mediciones de GAT en las córneas con queratocono. DCT ha demostrado ser el tonómetro más adecuado para utilizar en las mediciones de la PIO en los casos de queratocono, ya que no parece depender de CCT y CR.
Proper measurement of intraocular pressure (IOP) is fundamental in the diagnosis and follow-up of glaucoma because elevated IOP is the basic treatable risk factor in the management of glaucoma. The Goldmann applanation tonometer (GAT) is currently the most widely used device in clinical practice, and is accepted as the gold standard method for IOP measurement. However, it is known to be affected by changes in corneal thickness, structure, and curvature.1
Keratoconus is a bilateral, progressive, non-inflammatory corneal ectasia that results in irregular astigmatism and reduced vision quality because of corneal thinning and protrusion.2 Hence, the corneal changes associated with keratoconus may potentially lead to difficulties in accurate determination of IOP in these patients. Previous studies have shown that currently widely used tonometers such as the GAT, tend to underestimate IOP in keratoconic eyes mainly because of the characteristic reduced corneal thickness.3 Because of the many difficulties in IOP estimation in the keratoconic eyes, clinicians are interested in new tonometers that attempt to measure IOP independently of corneal thickness and curvature.
The ICare rebound tonometer (RT) is a portable handheld tonometer, which does not require any topical anesthetic. It records IOP by detecting the deceleration of a rod probe as it is bounced off the cornea. As the IOP increases, the rod probe bounced off the cornea faster. This movement is detected by a solenoid inside the instrument. RT also minimizes corneal injury and avoids the risk of cross infection through the use of disposable probes.4 RT has been shown to correlate well with GAT and is generally accepted to be dependent on corneal parameters. RT readings are, however, on average, higher than GAT readings in previous studies.5–7
The Pascal dynamic contour tonometer (DCT) claims to be relatively unaffected by corneal biomechanical properties. It is a slit-lamp mounted, nonapplanation, contour-matching contact tonometry. The tip of the tonometry has a concave surface and measures IOP when the cornea of patient matches the tip of the tonometry. It produces minimal distortion of the cornea and the IOP is the result of a direct measurement by a sensor integrated into the center of the tip. The IOP and quality of the data (Q1-5) are reported on a digital display.8 DCT also evaluate ocular pulse amplitude (OPA) which is the difference between the average systolic and diastolic IOPs. DCT would be theoretically unaffected by neither central corneal thickness (CCT) nor corneal radius of curvature (CR).8–10
The purpose of this study was to compare IOP measurements obtained by GAT, RT, and DCT and to assess relationship between IOP measurements and CCT, CR in keratoconic corneas.
Subjects and methodsThis cross-sectional study was conducted at the Department of Ophthalmology of the Eskişehir Osmangazi University School of Medicine. The study was performed in accordance with the Declaration of Helsinki principles and the local Medical Ethics Committee approved the study. Informed consent was obtained from all participants before the study.
Sixty-three eyes of 63 keratoconus patients were enrolled in this study. All study participants underwent a detailed ophthalmologic examination including best-corrected visual acuity, slit-lamp biomicroscopy, and fundoscopy. The diagnosis of keratoconus was made by an experienced corneal specialist (N.Y.) on the basis of the following diagnostic criteria (1 sign or a combination of signs): external signs such as Munson's sign (V-shaped conformation of the lower lid on down gaze), biomicroscopic signs such as stromal thinning, conical protrusion, Fleischer ring, Vogt striae, and enlarged corneal nerves; and an abnormal retinoscopy reflex. The diagnosis was confirmed topographically with the Oculus Pentacam system (TKC “Topographical Keratoconus Classification”). The contact lens wearers stopped using their contact lenses for 1 week before all measurements. Patients who had corneas with apical scarring or any kind of surgical treatment for keratoconus were excluded.
All IOP measurements were taken between the 9AM and 11AM to minimize the potential effect of diurnal variation in IOP. IOP was measured on each subject in a sitting position and always in the same order, RT-DCT-GAT, after a minimum interval of 10min between measurements.11 IOP measurements were taken by three masked experienced examiners.
ICare RT (TA01i, Tiolat Oy, Helsinki, Finland) is conducted by positioning the tip of the probe in front of the central cornea at a distance of 4–8mm before the measurement. The RT software is preprogrammed for six measurements. After the sixth measurement, the letter P appears in the display, followed by the IOP reading. The software discards the highest and lowest IOP readings automatically and calculates the average IOP value from the rest.
Pascal DCT (SMT Swiss Microtechnology AG, Port, Switzerland) is a self-calibrating device mounted on the slit-lamp. It consists of a sensor tip with a 10.5mm radius of curvature, a concave surface, and a miniaturized pressure sensor integrated into the center of the contact surface. The device displays the IOP value accompanied by a quality control (Q1-5). Measurement was performed under topical anesthesia with one drop of 0.5% topical proparacaine solution (Alcaine, Alcon Laboratories Inc., Fort Worth, TX, USA). Mean of three qualified IOP values (Q result is 1 or 2) were considered for statistical analysis in this study.
GAT (AT900, Haag-Streit, Koeniz, Switzerland) measurement was performed using a slit-lamp with same topical anesthetic and fluorescein under cobalt blue filtered light. Three consecutive readings were obtained moving the probeaway from the cornea after each measurement and a mean IOP value was calculated.
In all subjects, CCT and CR were measured using a rotating Scheimpflug camera (Oculus Pentacam, Wetzlar, Germany) before the IOP measurements. All measurements were taken by one experienced examiner.
The normality of the continuous variables was evaluated with the Shapiro–Wilk test. The differences between IOP readings were compared with the one way repeated measures ANOVA. The relationship between CCT, CR, and IOP readings were evaluated by Pearson correlation coefficient. P values lower than 0.05 were considered as statistically significant. We use only one eye data per person to avoid problems arising from using dependent measurements (measurements of both eyes of the same person). We choose the eye with the higher mean keratometry reading when the second eye of the same patient has keratoconus. All analyses were performed wih the softwares IBM SPSS Statistics version 21 and MedCalc version 12.7.5.0.
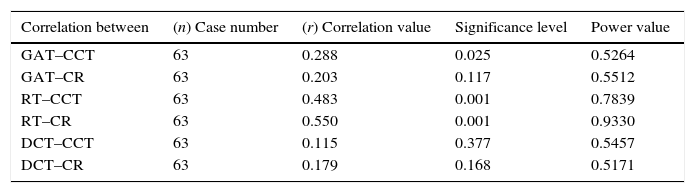
The statistical power analysis of our findings was made by using R for Windows x64 (v.3.2.2), a free and powerful statistical analysis software and programming language (R Foundation for Statistical Computing, Vienna/Austria, 2016, https://www.R-project.org). As we have had one study group and our findings were mainly based on correlation relationship, we have preferred to use power correlation calculation. The results are presented in the following table:
As it can bee understood from the table, calculated power levels of the given correlations are greater than 0.50 threshold cut-off level and this is sufficient for the given number of patients.ResultsA total of 63 eyes of 63 patients (27 females and 36 males) with a mean±SD age of 33.57±9.41 years (range, 19–61 years) were enrolled in the study.
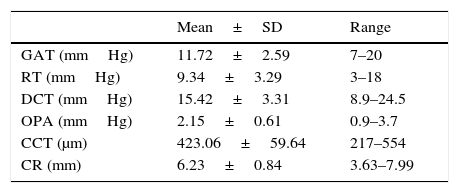
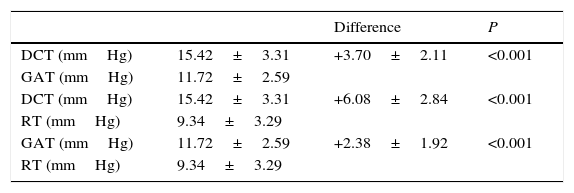
Mean IOP measurements obtained by each tonometer, mean CCT, and mean CR values are shown in Table 1. Comparison of the GAT, RT, and DCT derived IOP measurements are shown in Table 2. DCT measurements were significantly higher than GAT measurements (P<0.001) and RT measurements (P<0.001). Also GAT measurements were significantly higher than RT measurements (P<0.001).
Mean±SD IOP readings obtained by each tonometer, CCT, and CR values.
| Mean±SD | Range | |
|---|---|---|
| GAT (mmHg) | 11.72±2.59 | 7–20 |
| RT (mmHg) | 9.34±3.29 | 3–18 |
| DCT (mmHg) | 15.42±3.31 | 8.9–24.5 |
| OPA (mmHg) | 2.15±0.61 | 0.9–3.7 |
| CCT (μm) | 423.06±59.64 | 217–554 |
| CR (mm) | 6.23±0.84 | 3.63–7.99 |
GAT, Goldmann applanation tonometer; RT, rebound tonometer; DCT, dynamic contour tonometer; OPA, ocular pulse amplitude; IOP, intraocular pressure; CCT, central corneal thickness; CR, corneal radius of curvature; SD, standard deviation.
Comparison of the GAT, RT, and DCT derived IOP readings.
| Difference | P | ||
|---|---|---|---|
| DCT (mmHg) | 15.42±3.31 | +3.70±2.11 | <0.001 |
| GAT (mmHg) | 11.72±2.59 | ||
| DCT (mmHg) | 15.42±3.31 | +6.08±2.84 | <0.001 |
| RT (mmHg) | 9.34±3.29 | ||
| GAT (mmHg) | 11.72±2.59 | +2.38±1.92 | <0.001 |
| RT (mmHg) | 9.34±3.29 |
GAT, Goldmann applanation tonometer; RT, rebound tonometer; DCT, dynamic contour tonometer; IOP, intraocular pressure.
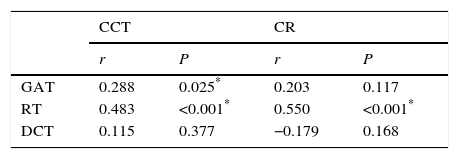
Table 3 shows correlation analyses between CCT, CR and IOP measurements. We found significantly positive correlation between GAT measurements and CCT (r=0.288, P=0.025). RT measurements were significantly positively correlated both CCT (r=0.483, P<0.001) and CR (r=0.550, P<0.001). However, DCT did not correlate with CCT (r=0.115, P=0.377) and CR (r=−0.179, P=0.168). RT is the most affected and DCT is the least affected tonometer from CCT and CR.
Correlation analyses between CCT, CR and IOP measurements.
| CCT | CR | |||
|---|---|---|---|---|
| r | P | r | P | |
| GAT | 0.288 | 0.025* | 0.203 | 0.117 |
| RT | 0.483 | <0.001* | 0.550 | <0.001* |
| DCT | 0.115 | 0.377 | −0.179 | 0.168 |
GAT, Goldmann applanation tonometer; RT, rebound tonometer; DCT, dynamic contour tonometer; IOP, intraocular pressure; CCT, central corneal thickness; CR, corneal radius of curvature.
The GAT is the most widely used method of measuring the IOP, but corneal parameters, especially corneal thickness, affect the accuracy of this tonometer. GAT underestimates IOP in thin corneas and overestimates IOP in thick corneas.12 So, newer devices such as RT and DCT are the new alternative techniques for IOP measurements. The initial reports on these new tonometers are promising and the reproducibility or reliability of data is being evaluated. In our study, DCT measurements were significantly higher than GAT measurements, but RT measurements were significantly lower than GAT measurements in keratoconic corneas.
RT has recently appeared in clinical practice after being used for some time in animal research. Its relatively low cost, portability, lack of need for topical anesthesia, being independent of a slit lamp and ease of use make it ideal for routine clinical practice.13 Previous comparative studies of IOP measurements recorded with RT and GAT have shown clinical agreement between the two devices, with a slight overestimation of readings with RT when compared with GAT.5–7 To the best of our knowledge, there is no study investigating RT measurements in keratoconic corneas. Rosentreter et al. compared RT, GAT and DCT for measuring IOP in 171 eyes with corneal abnormalities. They reported that RT significantly underestimated IOP according to GAT (12.7mmHg vs 15.5mmHg) measurements. However, only 21 eyes of 171 eyes had keratoconus in this study, being post-keratoplasty eyes (95 of 171) the most relevant of the corneal abnormalities included in this study.14 Arribas-Pardo et al. compared IOP measurements in 60 ectatic corneas having intrastromal corneal ring segment implantation using the RT and GAT. They found that Icare significantly underestimated IOP compared with GAT, whereas Icare Pro showed no statistical differences compared with GAT.15 We found that RT measurements were on average 2.38mmHg lower than GAT measurements. RT and GAT also correlated significantly with CCT. RT more affect than GAT from CCT in this study (see Table 3), therefore individuals had thin corneas such as keratoconus IOP tended to be underestimate with RT.
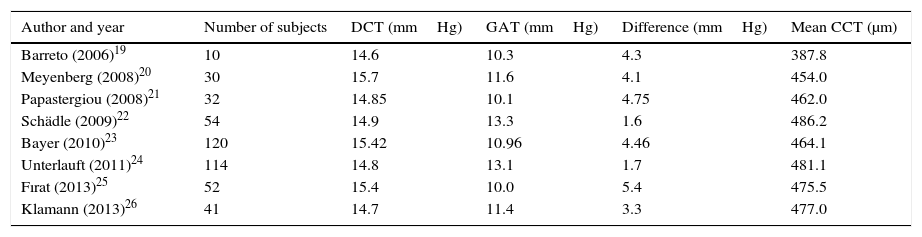
DCT is a method to measure IOP by using a pressure-sensitive tip that is closely shaped following the corneal curvature to minimize the corneal deformation. The forces of both sides of the cornea are meant to be nearly equal during the measurement.16 According to studies using human cadaver eyes, IOP values measured by DCT were significantly closer to the manometric reference pressure than the GAT measurements.17 Previous studies have demonstrated an excellent agreement between GAT and DCT, although DCT readings tended to be generally higher in healthy eyes and glaucomatous eyes.4,9,10,18 Conversely to RT, there are many studies investigating DCT measurements in keratoconic corneas. These studies are summarized in Table 4.19–26 DCT measurements about 4 mm Hg high than GAT measurements in keratoconic corneas shown in Table 4. Overestimation of DCT measurements can be explained the absence of correlation of IOP measurements with CCT, especially in eyes with thinner corneal thickness just as keratoconic corneas. Also GAT measurements have been found to be higher than DCT measurements in eyes with thicker corneas.27 In agreement with previous studies, we found that found that DCT measurements were 3.70mmHg higher than GAT measurements in our study.Today, many studies have shown that CCT is variable and is a major source of error in GAT, so the common practice of relying on unadjusted GAT results in misdiagnosis and mismanagement.1,12 We considered two corneal parameters (CCT and CR) to evalute their effect on IOP measurements in this study. We found significantly positive correlation between CCT and IOP measurements in GAT and RT but not in DCT. RT is the most affected tonometer and DCT is the least affected tonometer from CCT. Similarly, our previous study has reported that the IOP measured by RT increased 8mmHg for every 100-micron increase in CCT.28 On the other hand, there is no consensus in the literature about the relation between the CCT and IOP measurements by RT; some of the studies state that CCT affect the IOP measurements by RT5,6,28 but the others did not report this relationship.7,29 DCT did not significantly correlate with CCT in our study. DCT has been proposed to measure IOP irrespective of the corneal thickness because DCT does not flatten the cornea, which allows the cornea to maintain its shape provoking minimal distortion during the measurement.4,8–10,16–18
Studies investigating DCT measurements in keratoconic eyes.
| Author and year | Number of subjects | DCT (mmHg) | GAT (mmHg) | Difference (mmHg) | Mean CCT (μm) |
|---|---|---|---|---|---|
| Barreto (2006)19 | 10 | 14.6 | 10.3 | 4.3 | 387.8 |
| Meyenberg (2008)20 | 30 | 15.7 | 11.6 | 4.1 | 454.0 |
| Papastergiou (2008)21 | 32 | 14.85 | 10.1 | 4.75 | 462.0 |
| Schädle (2009)22 | 54 | 14.9 | 13.3 | 1.6 | 486.2 |
| Bayer (2010)23 | 120 | 15.42 | 10.96 | 4.46 | 464.1 |
| Unterlauft (2011)24 | 114 | 14.8 | 13.1 | 1.7 | 481.1 |
| Fırat (2013)25 | 52 | 15.4 | 10.0 | 5.4 | 475.5 |
| Klamann (2013)26 | 41 | 14.7 | 11.4 | 3.3 | 477.0 |
DCT, dynamic contour tonometer; GAT, Goldmann applanation tonometer; CCT, central corneal thickness.
Many published studies have suggested correction factors based on CCT and GAT, but the effects of CR on IOP measurements by GAT remain uncertain. Mark suggested that a flatter cornea might lead to lower GAT measurements in 1973.30 Orssengo and Pye discussed the deformation of a central cornea flattened by the pressure of the prism and bulging outward from the middle to the peripheries due to the inner pressure of the eye.31 However, other studies could not find any significant correlation between CR and IOP.32,33 Gunvant et al. reported that an increase of 1mm of mean CR was accompanied by a rise in IOP of 1.14mmHg measured by GAT, but this effect was weak and not statistically significant.34 Our previous study show that CR had no significant effect on measured IOP with RT in 165 healthy schoolchildren.35 Francis et al. reported that CR affected IOP measurements with DCT but not with GAT, with mean DCT IOP increased with increasing CR.36 We found a positive significant correlation between CR and IOP measurements in RT but not in GAT and DCT in this study.
Several corneal biomechanical properties affect IOP measurement except CCT or CR. The ocular response analyzer was the first device introduced to measure biomechanical features of the cornea. The ocular response analyzer reports two indices: corneal hysteresis and corneal resistance factor. Corneal hysteresis is considered to be a measure of corneal viscoelasticity. Corneal resistance factor has been formulated to delineate the effect of CCT on corneal hysteresis. Both corneal hysteresis and corneal resistance factor decrease in keratoconic corneas compared with normal patients, which indicates mechanical weakening of the stroma.23,37,38 We could not evaluate corneal biomechanics in this study, and it may be pointed as the limitation of our study. Sahebjada et al.39 reported that corneal thickness at the center and at the apex is different in different levels of keratoconus severity. These changes result in significant alterations in these parameters as severity of the disease increases. In addition to this, corneal pachymetric readings correlate well with corneal curvature but CCT and the CR may not match with the thinnest point of the cornea or the radius of curvature in the area of the conus.
In conclusion, DCT has overestimated but RT has underestimated IOP readings according to GAT measurements in keratoconic corneas. We also found significantly positive correlation between CCT and IOP measurements in GAT and RT but not in DCT. RT is the most affected and DCT is the least affected tonometer from CCT. RT measurements were also significantly positively correlated with CR.
FundingNone.
Author's contributionFÖ performed study concept and design, literature search, patient's randomization and data collection, writing and reviewing of the study. NY performed study concept and design, literature search, writing and reviewing of the study. ET performed patient's randomization and data collection of the study. AŞ performed statistical analysis of the study. All authors read and approved the final manuscript.
Conflicts of interestThe authors have no conflicts of interest to declare.