The aim was to review the published literature on corneal collagen cross-linking. The emphasis was on the seminal publications, systemic reviews, meta-analyses and randomized controlled trials. Where such an evidence did not exist, selective large series cohort studies, case controlled studies and case series with follow-up preferably greater than 12 months were included. Riboflavin/Ultraviolet A (UVA) corneal collagen cross-linking appears to be the first treatment modality to halt the progression of keratoconus and other corneal ectatic disorders with improvement in visual, keratometric and topographic parameters documented by most investigators. Its precise mechanism of action at a molecular level is as yet not fully determined. Follow-up is limited to 4–6 years at present but suggests continued stability and improvement in corneal shape with time. Most published data are with epithelium-off techniques. Epithelium-on studies suggest some efficacy but less than with the epithelium-off procedures and long-term data are not currently available. The use of Riboflavin/UVA CXL for the management of infectious and non-infectious keratitis appears very promising. Its use in the management of bullous keratopathy is equivocal. Investigation of other methodologies for CXL are under investigation.
El objetivo fue revisar la literatura publicada sobre el tratamiento de entrecruzamiento del colágeno corneal (CXL), principalmente las publicaciones fundamentales, revisiones sistémicas, meta-análisis y ensayos controlados aleatorios. Cuando tales evidencias no existieron, se incluyeron estudios selectivos de grandes series de poblaciones, estudios controlados de casos y series de casos, con un seguimiento preferiblemente superior a doce meses. El entrecruzamiento del colágeno corneal con Riboflavina/Ultravioleta A (UVA) parece constituir la primera modalidad de tratamiento que detiene la progresión del queratocono y otros trastornos ectáticos corneales, con mejora de los parámetros visuales, queratométricos y topográficos, según lo documentado por muchos investigadores. El mecanismo específico de acción a nivel molecular no ha sido totalmente determinado aún. El seguimiento se limita a 4–6 años actualmente, aunque sugiere la estabilidad y mejora continuas de la forma corneal con el tiempo. Muchos datos publicados se refieren a las técnicas sin desbridamiento epitelial. Los estudios sin desbridamiento epitelial sugieren cierta eficacia, aunque menor a la de las intervenciones con desbridamiento epitelial, no disponiéndose actualmente de información a largo plazo. El uso del CXL con Riboflavina/UVA para el tratamiento de la queratitis infecciosa y no infecciosa parece muy prometedor. Su uso en el tratamiento de la queratopatía bullosa es equívoco. Se está llevando a cabo una investigación de otras metodologías de CXL.
Keratoconus is a degenerative disorder distinguished by para-central corneal thinning and secondary ectasia, resulting in irregular astigmatism with impaired vision, ghosting and polyopia.1–3 It is typically bilateral but often asymmetrical. Onset typically is at puberty with progression of disease for 10–20 years when it tends to stabilize. It is the commonest corneal dystrophy, affecting about 1 in 1750 individuals. It occurs in all racial groups and equally affects males and females.1–3 Studies of quality of life analysis report that that its magnitude of public health impact is disproportionate to its prevalence.4 Scores of life impairment are equivalent to grade 3–4 age related macular degeneration.4
Its aetiology is not understood and includes genetic, biochemical, and physical factors, with no sole proposed theory elucidating its range of clinical presentations and it is probable that keratoconus is the eventual manifestation for several different conditions. It usually appears as an isolated condition, but has been associated with a number of ocular and systemic disorders, including, vernal disease, retinitis pigmentosa, blue sclera, atopy, magnesium deficiency, Down's syndrome, Turner syndrome and connective tissue disorders such as Marfans syndrome, Ehlers–Danlos syndrome, osteogenesis imperfect and pseuodoxanthoma elasticum.1,2 It has been related to repeated surface ocular trauma associated with hard contact lens wear, allergic eye disease and eye rubbing.1,2 Genetic factors are important up to 10% having a family history of the condition.5 An increased activity of proteinase enzymes and reduced activity of proteinase inhibitors have been identified in keratoconic corneas,6 with the increased stromal protein digestion resulting in reduced biomechanical stability and corneal thinning.7 There appears to be an inverse relationship between severity of the condition and diabetes.8
Pellucid marginal corneal degeneration (PMD) is less common than keratoconus. It usually affects the inferior peripheral, rather than para-central, cornea in about 85% of cases and the superior peripheral cornea in 15%. It occurs in a crescentic fashion typically between the 5 and 7 o’clock positions.9,10 It is more common in males, with a male to female ratio of approximately 3:1.10 Its age of onset is usually later than keratoconus, presenting between the 2nd and 5th decades. It is typically bilateral and affects all ethnicities.9,10 The incidence and aetiology of PMD remain unknown. It often presents with progressive with severe against the rule astigmatism typically with good spectacle corrected acuity until the advanced stages of the disease. Hydrops and even spontaneous perforation can occur.9,10 Topography typically shows a “lobster-claw pattern” but this is not pathognomonic and may also occur in keratoconus and there is overlap between the two conditions, as well as with keratoglobus.10,11
Kerectasia after refractive surgery is a rare but often visually devastating complication. It was first described after Laser in situ keratomileusis (LASIK) by Seiler in 1998.12 It reported incidence ranges from 0.04 to 0.6% of post-LASIK cases,13,14 with one survey reporting that over 50% of responding refractive surgeons had documented at least one of their patients with such problems.15 Its onset is variable, ranging from 1 to 45 months after surgery with 50% of cases occurring within 12 months.13 It is often visually devastating with one study in the early 2000s reporting that 35% of cases eventually required corneal transplantation.16 As well as following LASIK it has also been reported after photorefractive keratectomy (PRK)13,17,19 and other forms of keratorefractive surgery such as radial keratotomy.18 Careful pre-operative screening is essential to reduce occurrence and identified risk factors include pre-existing keratoconus and PMD, including forme fruste cases, thin corneas, high myopic corrections, residual stromal bed less than 250μm and young age,13,16,17,19 although ectasia can occasionally occur in patients without currently identifiable risk factors.16,19
Management of keratoconus, PMD and post-surgery ectasia depends on their severity and the extent of irregular astigmatism. Mild cases are correctable with spectacles and soft toric contact lenses. However, with progressive disease, the cornea becomes more irregular and rigid gas permeable lenses are required.20 In 15–20% of keratoconic patients, surgery, typically keratoplasty, becomes necessary, as a result of contact lens intolerance, corneal scarring and thinning.21 None of these interventions, while often successful in terms of visual rehabilitation, treat the underlying causes of kerectasia and its progression. It is only with the advent of corneal collagen cross-linking (CXL) that we can hope to slow, stop or even to a limited extent reverse keratoconus.22–24
BackgroundCXL processes occur physiologically with age via natural enzymatic pathways such as transglutaminase and lysyl oxidase. Photochemical CXL with Riboflavin (vitamin B2)/Ultraviolet A (UVA) (370nm) was developed at the University of Dresden by Spoerl and Seiler.22–25 They postulated that the procedure induces physical cross-linking of collagen by Riboflavin absorbing UVA to act as a photo sensitizer to produce free radicals (oxygen singlets) that activate the natural lysyl oxidase pathway.25 By absorbing UVA, the Riboflavin also prevents damage to deeper ocular structures, including as the endothelium, lens and retina.25 A more recent paper has corroborated the importance of singlet oxygen production, created by the interaction of UVA and Riboflavin, in the CXL process.26 The singlets are, however, thought not to instigate cross-linking by lysyl oxidase but possibly by three other mechanisms: imidazolone production, which can attach to molecules, such as histidine, to form new covalent bonds; the triggering of endogenous populations of carbonyl groups in the ECM (allysine, hydroxyallysine) to form cross-links there, and/or the degradation of the Riboflavin molecule itself, releasing 2,3-butanedione, which can react with the endogenous carbonyl groups of the stromal proteins.26 The precise location of the cross-links at a molecular level is as yet undetermined. Certainly, cross-links cannot form between the collagen fibrils as the distance is too far for the formation of intra-molecular bonds. Hayes et al. in a series of ex vivo ungulate and rabbit eyes investigated corneal stromal ultrastructure using X-ray scattering, hydrodynamic behaviour and enzyme digestion and determined that it was likely that the cross links formed during Riboflavin/UVA therapy were occurring predominantly at the collagen fibril surface, rather than within the fibrils themselves, and in the protein network surrounding the collagen.27
Laboratory studies: biomechanical and biochemical considerationsThere is no definite evidence for CXL producing corneal collagen and protoeglycan cross-links, as these molecular bonds cannot be seen microscopically. Ex vivo, laboratory studies, however, have reported changes in physico-chemical properties of the stroma following CXL. Stress-strain measurements of corneal stromal tissue are significantly increased,24,28 both immediately as well as several months following the procedure.29 These changes have been shown to principally occur in the anterior 200μm of the stroma where the most of the UVA absorption takes place.30 A higher shrinkage temperature has been demonstrated in corneal tissue following CXL, with a greater effect being reported in the anterior stroma.31 Increased resistance of stromal tissue to enzymatic digestion has been confirmed after CXL, with a dose response in relation to the UVA intensity.32 In addition, an increased resistance to matrix metalloprotienase (MMP), in particular sub-types MMP-1, 2, 9, and 13, degradation of collagen and small leucine-rich proteoglycans following Riboflavin/UVA CXL has been found.33 The protective effect of CXL on collagen and proteoglycans from MMP cleavage is likely to be important in the mechanism of preventing the progression of keratoconus and other corneal ectatic disorders, where an increased activity in collagenases has been established.19 Other biophysical and biomechanical alterations include, an increase in collagen fibre diameter in Rabbit corneas,34 and a significant reduction in the hydration behaviour of the stroma, both of which are greater in the anterior compared to the posterior stroma.35 Recently, however, other investigators have suggested that such changes are probably short-term alterations, due to a consequence of the effects of the osmolarity of the Riboflavin solutions used rather than actual effects of cross-linking and not likely to be long-term changes.27,36 In addition to the above, there are alterations in the electrophoretic pattern of corneal collagen type I after CXL, with the occurrence of an extra intense polymer band, with a molecular size of approximately 1000kDa, resistant to mercaptoethanol, heat, and pepsin.37
Laboratory studies: safetyUVA is cytotoxic. It can cause keratocyte apoptosis and most significantly endothelial cell damage and death and permanent lens and retinal injury.38–41 Studies with cell cultures have found an increased cytotoxic irradiance level with UVA irradiation combined with photosensitizing Riboflavin for keratocytes, which in the clinical setting would occur in human corneas to a depth of 300μm.38 With regard to endothelial damage, cell culture studies have demonstrated a cytotoxic threshold level above 0.35mW/cm2 UVA exposure for 30min.39 This should not be reached in the clinical setting with corneal thickness greater than 400μm.39 In vivo studies have confirmed these results and have demonstrated that with UVA exposure of 3mW/cm2 for 30min, that over 85–90% of UVA radiation is absorbed by the Riboflavin in the anterior 400μm of the stroma, so that the irradiance at the level of the endothelium is less than 0.18mW/cm2, i.e. 50% less than the cytotoxic level.40,41 This is situation is the same for other internal structures, such as the lens and retina, where the level of UVA radiation reaching these structures is less than 3% of the cytotoxic threshold.41
Clinical studiesThe first reported clinical application of CXL was not for keratoconus, but to treat corneal ulceration. It was shown to effectively halt corneal melting in 3 out of 4 treated eyes.42 The first published study of its use in keratoconus was done in 2003.25 Wollensak, Spoerl and Seiler reported a series of 23 keratoconic eyes, in which there was stabilization of ectasia following CXL, with up to five years follow-up in a few eyes. In 70% of cases an improvement in ectasia was seen, with a decrease of maximal keratometry by 2 diopters (D) and the refractive error by 1D. There was no long-term loss of transparency of the cornea or lens in any eye and endothelial counts were unaltered post-operatively.25 Multiple subsequent prospective, non-randomized studies with up to 24 months follow-up from other research groups throughout the world,43–54 including case series of paediatric patients55,56 and advanced keratoconus,57 have confirmed these encouraging initial results. Typically they report keratoconic stabilization in the vast majority of treated eyes with few complications (see complications section below) and significant post-operative improvements in visual performance, reductions in keratometry/corneal power and reductions in higher order aberrations.43–57 Similar promising reports of case series of CXL in post-laser refractive surgery ectasia have been published with stability and improved vision being attained with over 2 years follow-up,58–60 with successful outcomes also reported in individual case reports of CXL for PMD.61,62
While the outcomes of these prospective studies have been very encouraging, there is a scarcity of randomized, prospective clinical studies within the literature. The few published studies, however, do support the efficacy of the technique. Wittig-Silva published interim results of a randomized, bilateral study in 33 eyes at 6 months, which showed an average reduction in corneal power of 0.9 diopters (D) in treated eyes and an increase of 0.6D in untreated eyes.63 To date the completed study remains unpublished. O’Brart et al. in a completed, randomized, prospective, bilateral study in 22 patients with documented keratoconic progression, reported stabilization in all treated eyes with statistically significant improvements in BSCVA, corneal power measurements and higher order aberrations and progression in 14% of untreated eyes over the 18 month follow-up period.64 Further randomized prospective studies, including that conducted by the Food and Drug Administration should hopefully be published in the near future.
CXL in combination with other treatment modalitiesAs an isolated treatment, CXL has been used in combination with other treatment modalities to optimize visual outcomes in keratoconic and post-laser ectasia. Combined CXL and limited topography-guided PRK in selected eyes with moderate ectasia and adequate corneal thicknesses has been shown to be effective with marked improvements in visual, refractive and topographic parameters and stabilization of the ectatic process in the vast majority eyes.65–69 Such treatments have been shown to be associated with significant improvements in quality of life scores.70 Follow-up in these studies, however, is limited to only 1–3 years so that long-term biomechanical stability has not been fully elucidated. In addition significant corneal haze/scarring has been reported.71 CXL has also been used after intra-corneal ring segment (ICRS) insertion and even in a three step procedure with both PRK and ICRS insertion.72 Some studies have suggested that CXL may have an additive effect,73,74 although this has not been demonstrated in all studies.75 CXL has also been used in conjunction with keratorefractive procedures such as PRK and LASIK in an attempt to improve long-term stability and reduce the possible occurrence of post-surgery ectasia.76,77 As yet, such studies are very limited in terms of numbers treated, efficacy and long-term follow-up, although a single contralateral eye study in of CXL after hyperopic LASIK demonstrated less regression of correction over the limited follow-up period.78
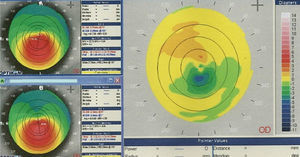
Long-term follow-upWhile clinical studies certainly support the mid-term efficacy of CXL, there is a paucity of long-term data. Keratoconus typically progresses at a variable rate, for up to two decades following presentation and then tends to stabilize, presumably as a result of physiological age-related cross-linking.1–3 The turnover rate of corneal collagen and the extracellular matrix (ECM) is unknown. Taking these factors into consideration, the length of efficacy of CXL and the need to repeat the procedure is uncertain. Table 1 documents the outcomes of those prospective case series in the published literature with follow-up of 24 months or more. Only a few groups have actually presented data with over 3–4 year follow-up. Raiskup-Wolf et al. reported 33 eyes with over 3 year follow-up and found stabilization of keratoconus with reduction of keratometry and improvements in vision with time.79 Caporossi et al. detected keratoconus stability in 44 eyes after 48 months, with a reduction in keratometry and coma and improvements in vision.80 O’Brart et al. in a series of 29 eyes of 29 patients with 4–6 years follow-up found ectatic stabilization in all eyes, with significant improvements in refraction, visual acuity, keratometry and corneal wave-front measurements.81 In addition and similar to the findings of Raiskup-Wolf et al.,79 they documented continued improvements in keratometry and higher order aberrations with follow-up from 1 to 4–6 years and similar to Caporossi et al.,80 25% of their initially untreated fellow eyes demonstrated evidence of progression.81Fig. 1 shows the difference map of a typical patient in their series, 4 years after CXL with flattening of the apex of the cone resulting in an improvement in corneal shape, reduction in higher order aberrations and enhancement in visual performance. Similarly, Hashemi et al. demonstrated stabilization in 40 eyes of 32 patients with progressive keratoconus with continued improvement in elevation measurements over 5 years of follow-up82 and Richoz et al. reported stabilization of ectasia after LASIK and PRK with a follow-up of over 5 years in some eyes in their case series.83 Such findings further support the efficacy of CXL up to 4–6 years, with documented progression in fellow untreated eyes indicating that improvements in measured parameters in treated eyes with time are not due to physiological age-related cross-linking changes. Further follow-up will determine long-term efficacy and the need if any to repeat the procedure and will elucidate how long and to what degree eyes might continue with improvement in visual and topographic parameters. The recurrence of keratoconus following keratoplasty, which typically, albeit rarely, occurs 10–20 following surgery,84 suggests that turnover of corneal collagen and ECM may be measured in decades and that CXL might be effective for at least this length of time if not longer given physiological cross-linking changes with age.
Visual, refractive and keratometric changes after epithelium off Riboflavin UVA CXL in prospective case series in which all eyes have a reported follow-up of 24 months or more.
| Lead author | Year | Number (eyes) | Follow-up (months) | UDVA change (LogMar) | CDVA change (LogMar) | MSE change (D) | K Max change (D) | Pachymetry change (μm) | Failure (%) |
| Raiskup | 2008 | 33 | >36 | −0.15 | −2.57 | 6 | |||
| Caporossi A | 2010 | 44 | 48 | −0.37 | −0.14 | +2.15 | −2.26 | +0.6 | 0 |
| Kampik D | 2011 | 46 | 24 | −0.05 | −1.23 | −21.6 | |||
| Vinciguerra A | 2012 | 40 | 24 | −0.21 | −0.19 | +1.57 | −1.27 | +14.0 | |
| Goldich Y | 2012 | 14 | 24 | −0.08 | −2.40 | 0 | |||
| O’Brart D | 2013 | 30 | >48 | −0.01 | −0.1 | +0.8 | −1.06 | +2.0 | 0 |
Difference topographic map of an eye with keratoconus 4 years after epithelium off CXL showing the typical picture of flattening of the apex of the cone (green colour) with some slight steepening of the adjacent superior hemi-meridian (orange colour). Such changes are associated in an improvement in corneal higher order aberrations, especially vertical coma, and accompanying enhancements in visual performance.
Prior to CXL, it is necessary to obtain documented evidence of progression of the condition. To reduce the risk of endothelial damage it must be ensured pre-operatively that central corneal thickness is greater than 400μm.25–27 Following fully informed consent, CXL is typically performed under topical anaesthesia. In the standard epithelium-off technique the central 8–9mm of the corneal epithelium is de-brided to enable adequate stromal Riboflavin absorption.25,43–64 Following epithelial de-bridement, Riboflavin 0.1%, suspended in a dextran T500 20% solution, is applied every 3–5min for at least 20min to allow sufficient stromal uptake prior to UVA exposure.25 Intra-operative pachymetry is advocated by many surgeons to monitor corneal thickness prior to UVA exposure and administer hypotonic Riboflavin drops if it thins excessively during Riboflavin administration. The central 8–9mm of the cornea is then irradiated with UVA, at 3mW/cm2 for 30min. During this time, Riboflavin drops are reapplied to the stromal surface every 3–5min during the 30-min irradiation period. Following treatment, topical antibiotics and corticosteroids are prescribed until corneal re-epithelialisation. Systemic analgesic and bandage soft contact lenses can be used for pain management. Topical anaesthetics in limited dosage, no more than 2h and only for 48h may also be of benefit.85 Significant ocular pain is typically experienced for the first 24–48h following surgery and vision is blurred for 1–2 weeks. Rigid contact lens wear can be resumed once the epithelium has fully healed, typically at about 2–3 weeks. Confocal microscopy has identified oedema, superficial nerve loss, rarefaction of keratocytes in the anterior and mid-stroma and isolated endothelial damage in the immediate post-operative period.86–88 There is keratocyte re-population during the first three months, which is usually completed in six months. An increased density of the extracellular matrix occurs to a depth of 300–350μm. This forms the “demarcation line” which can be seen on slit lamp examination.89 Regeneration of nerve fibres, with restoration of the sub-epithelial plexus occurs within 12 months with return of full corneal sensitivity. These confocal studies have confirmed the lack of endothelial damage, with no alterations of cell density changes or hexagonality.86–88 In vivo confocal microscopic changes after CXL have been confirmed by histological examination of corneal buttons after keratoplasty.90–92 Such studies corroborate keratocyte loss and damage, which can be prolonged,90 with an increase in collagen fibril diameter.90–92
Epithelium on versus epithelium off techniquesRiboflavin is a hydrophilic molecule which cannot easily pass the tight junctions of the intact epithelial barrier. Spoerl confirmed the need for complete central epithelial debridement to allow sufficient stromal uptake of Riboflavin and reported no changes in the biomechanical properties of corneal tissue where the CXL was performed with the epithelium intact.23 On the basis of his study, the epithelium was removed prior to Riboflavin administration in the first clinical studies.25,43–64,79–83 In spite of these findings, some clinicians have elected to perform CXL with the epithelium intact74 or partially disrupted93 or with the use of femtosecond-created intra-stromal pockets,94 in an attempt to reduce post-operative discomfort and aid visual recovery. The use of repeated applications of tetracaine 1% to try to loosen epithelial tight junctions has been advocated.74 Others investigators have utilized limited full-thickness epithelial debridement in a grid pattern, with remaining islands of intact epithelium to aid post-operative epithelial healing.93 Laboratory studies, employing spectrophotometry to indirectly measure stromal Riboflavin absorption have shown the need with standard Riboflavin solutions to completely remove the central epithelium.95,96 Superficial epithelial trauma, pre-operative, multiple administration of topical tetracaine 1%, application of 20% Alcohol solution, grid pattern epithelial removal were all found to be insufficient to attain adequate homogeneous Riboflavin stromal absorption.95,96 In recent years, novel formulations of Riboflavin have been developed to facilitate trans-epithelial absorption. Laboratory studies with Riboflavin preparations in which trometamol (Tris–(hydroxymethyl)aminometane) and Sodium Ethylenediaminetetraacetic acid (EDTA) have been added (Ricrolin TE®, Sooft Italia S.p.A.) have been shown to facilitate stromal absorption especially with superficial/grid pattern epithelial trauma.97 Similarly, preparations without dextran but with sodium chloride 0.44% and benzalkonium chloride 0.02% and 0.04% have been shown to facilitate trans-epithelial Riboflavin stromal absorption.98,99 Clinical studies with such novel formulations have shown encouraging results, although they have been somewhat equivocal with some studies suggesting similar efficacy to standard epithelium-off techniques,100,101 and others with less pronounced effects.102–104 At present all long-term data over 3 years and most published clinical studies have been performed with “epithelium-off” procedures and further clinical studies with longer follow-up and especially randomized, controlled trials are required to ascertain the efficacy of “epithelium-on” CXL compared to the current gold standard of “epithelium-off” CXL.
In addition to the novel formulations discussed above, in vitro studies have demonstrated enhanced trans-epithelial Riboflavin absorption using iontophoretic delivery (Vinciguerra P. et al. 2012: ARVO E-Abstract 1518), (Ziebarth M.N. et al. 2012: ARVO E-Abstract 2544). Riboflavin is an effective molecule for iontophoretic transfer as it is small, negatively charged at physiological pH and is easily soluble in water. Clinical studies are being undertaken with a recently published study of 22 eyes with mild progressive keratoconus which underwent trans-epithelial CXL with iontophoresis for 10min demonstrating a significant reduction in keratometry and corneal astigmatism post-operatively with an improvement in uncorrected acuity.107 As well as iontophoresis, other methodologies currently under pre-clinical investigation to facilitate trans-epithelial Riboflavin stromal absorption include the use of ultrasound,108 nano-emulsion systems109 and other epithelial permeation enhancers such as d-alpha-tocopheryl poly(ethylene glycol) 1000 succinate (Vitamin E-TPGS).110
Rapid (accelerated) CXL techniquesCurrent treatment protocols utilize UVA energies of 3mW/cm2 and require 30min of UVA exposure to achieve the desired clinical effect.25,43–64 It has been theorized that by increasing the UVA fluence while simultaneously reducing the exposure time (the Bunsen–Roscoe law of reciprocity), the same sub-threshold cytotoxic corneal endothelial UVA dosage can be administered, thereby maintaining efficacy and safety, but with a reduced treatment time. This can allow improved patient comfort and convenience as well as shortened keratocyte exposure time. The latter may perhaps result in less keratocyte damage and apoptosis.
Preclinical ex vivo studies have been encouraging, with similar biomechanical changes as measured by scanning acoustic microscopy and extensiometry, seen between the standard UVA exposure of 3mW/cm2 for 30min compared with higher fluencies with shorter exposure times,111,112 albeit with a sudden decrease in efficacy with very high intensity UV light greater than 45mW/cm2.113 This decrease in efficacy with higher fluencies is not understood but might be related to oxygen consumption and availability, which has been shown to limit the photochemical cross-linking process.26
Published clinical studies at present are few. Cinar et al. in a study of 23 eyes showed that accelerated CXL produced a significant reduction in topographic keratometry values and an improvement in corrected distance acuity with a limited follow-up of 6 months.114 Similarly, Kanellopoulos in a randomized, prospective study using a UVA power of 7mW/cm2 for 15min compared to 3mW/cm2 for 30min has demonstrated similar clinical results as the standard technique in terms of ectasia stabilization without any adverse effects associated with the higher fluence, shorter duration treatments.115 Further studies using higher fluencies and shorter exposure times are either underway or being planned and hopefully future CXL treatment times should be considerably shortened.
Treatment of thin corneasDue to the potential of endothelial toxicity and cell death, CXL using the standard protocol is contraindicated for individuals with corneas thinner than 400μm. In a number of studies, hypo-osmolar Riboflavin solutions have been used to swell the cornea intra-operatively to over 400μm and enable CXL to be undertaken. Raiskup et al. in a series of 32 eyes with corneas thinner than 400μm showed stability of vision and keratometry with no adverse events at 12 months,116 while Nassaralla et al. in 18 eyes demonstrated swelling of the cornea with the intra-operative administration of hypo-osmolar 0.1% Riboflavin with no intraoperative, early postoperative, or late postoperative complications.117 However, in one study of CXL in thin corneas endothelial counts were shown to be slightly reduced, although vision and keratometry were improved118 and in one case report, progression continued after CXL in an eye with a central thickness of less than 330μm.119 In addition to the use of hypo-osmolar Riboflavin, Spadea and Mencucci demonstrated efficacy with no endothelial damage with trans-epithelial CXL in corneas at thin as 331–389μm.120 More clinical series and follow-up are required to establish if these procedures in thin corneas are as effective and safe as standard CXL in corneas with thicknesses greater than 400μm.
New methodologiesWhile Riboflavin/UVA CXL has been shown to be effective, other methodologies which are potentially more rapid and less invasive, are currently under investigation. Rocha et al. reported a flash-linking process with UVA and polyvinyl pyrrolidone with may have the potential to photo-chemically cross-link the cornea in only 30s.121 Paik et al. have investigated the topical application of short-chain aliphatic beta-nitro alcohols122 and Cherfan et al. demonstrated an almost fourfold increase in corneal stiffness with no reduction in keratocyte viability with rose bengal 0.1% administration and green light application and a less than 5min total treatment time.123 Undoubtedly other methodologies and applications will become available over the several next years due to the vast interest in this area of research.
Adverse effects of CXLClinical studies indicate that CXL is a safe procedure with few sight-threatening complications. Adverse events, however, can occur and have been reported. Reported complications include corneal haze and scarring, reduced uncorrected and BSCVA, infectious and non-infectious stromal melting and treatment failure with progression of ectasia.
HazeMid-stromal haze occurs in the majority of eyes, typically appearing at 2–6 weeks and clearing by 9–12 months. It is the result of an increased density of extracellular matrix and arises at a depth of 300–350μm. It forms the demarcation line which can be easily seen on slit lamp examination.89 As this change is self-limiting, topical cortical steroids are not indicated. Persistent haze/scarring, however, can occasionally occur. Raiskup reported persistent stromal haze at 12 months in 8.6% of cases in a series of 163 eyes.124 Compared to eyes without haze in this series, affected eyes had a higher apex power (average 72D), higher 3.00mm keratometry (average 54.75D) and thinner central pachymetry (average 420μm). On the basis of these findings, caution and careful patient counselling before CXL is advised in patients with advanced keratoconus.125
Sterile infiltratesSterile infiltrates may occur in the early post-operative period and usually resolve with a few weeks with topical corticosteroid medication. Koller reported sterile infiltrates in 8 eyes (7.6%) in a series of 117 cases. These infiltrates resolved within 4 weeks with topical dexamethasone 0.1% treatment.125 More rarely, serious cases of non-infectious keratitis, occurring 1–4 days following CXL, with loss of BSCVA have been reported. These cases have been typically associated with a possible with atopic eye disease.126 A single case of corneal melting associated with activation of herpes simplex keratitis has also been reported.127 It is prudent therefore to fully control atopic eye disease prior to cross-linking and to give prophylactic systemic Acyclovir in patients with previous Herpetic Eye disease.
Infectious keratitisInfectious keratitis post CXL has been reported. This is to be expected as de-briding the corneal epithelium can expose the corneal stroma to microbial infection. Cases of bacterial infection with Staphylococcal epidermidis, Escherichia coli, Pseudomonas aerunginosa and Coagulase negative Staphylococcus as well as Acanthamoeba have all been reported.128–130 A number of these cases have been associated with post-operative bandage contact lens misuse. It is important to inform patients not to replace, remove or try to clean these lenses themselves.
Endothelial failureEndothelial failure has been reported very occasionally after CXL resulting in corneal oedema post-operatively. Sharma et al. in a retrospective series of 350 patients treated with a standard “epithelium-off” protocol in eyes with corneal thicknesses greater than 400μm after epithelial removal, reported persistent problems in 5 patients (1.4%), 2 of whom (0.6%) required penetrating keratoplasty.131 Bagga et al. reported a single case with keratouveitis and endothelial failure that required keratoplasty.132 While such complications are rare, they high-light the need to warn patients pre-operatively of severe sight-threatening complications and the very occasional need for keratoplasty after CXL. The aetiology of such problems has not been fully elucidated but endothelial damage after CXL may occur even in corneas with adequate thickness perhaps due to severe stromal thinning intra-operatively due to the use of hyper- and iso-osmolar Riboflavin solutions and/or lack of homogenicity with hot spots in the UV beams associated with the use of diodes and limited focusing/alignment systems.
Progression of ectasiaAlthough the great majority of eyes are stabilized after CXL, failure of treatment with progression of keratoectasia can occur. Raskup in a series of 241 eyes, with over 6 month follow-up, reported stabilization in 98% of cases with progression identified in only 2 eyes.79 Koller in 177 eyes described progression in 8 eyes (7.6%). They identified eyes with advanced keratoconus with maximum keratometry values greater than 58D of being at greatest danger of progression.125
Other clinical indications for CXLBullous keratopathyAs some initial ex vivo laboratory studies reported a reduction in the hydration behaviour of the corneal stroma after CXL,35 although this has been refuted by other investigators,27,36 it has been postulated that CXL may be efficacious in the management of bullous keratopathy, either to delay and/or prevent the need for keratoplasty. In two studies consisting of only four eyes, corneal pachymetry was found to be reduced at 6–8 months.133,134 A more recent study reported CXL in 14 eyes with pain secondary to pseudophakic bullous keratopathy.135 Treatment improved corneal transparency and reduced corneal thickness and pain at 1 month but the beneficial effects reduced with time and were unchanged from pre-operative levels at 6 month.135 Although somewhat equivocal, further longer term studies in larger patient series are necessary to determine the efficacy of CXL for this indication.
Microbial keratitis/corneal ulcerationThe first published clinical application of CXL was actually to treat corneal ulceration and melting and demonstrated cessation of the melting process in 3 out of 4 eyes.42 The ability of CXL to increase the resistance of corneal tissue to enzymatic digestion, as well as for UVA to kill microbes offers great promise for a possible role in the treatment of microbial keratitis. Within the literature there now several case series of CXL in eyes with microbial keratitis, including cases of Acanthamoeba and fungal infection, unresponsive to anti-microbial therapy. In the majority of cases progression of the melting process was halted within a few days of treatment and emergency keratoplasty avoided.136–138 This potential application of CXL is extremely exciting with a recent systemic-review and meta-analysis by Alio et al. identifying 12 published articles within which treatment of 104 eyes had been reported and from which pooled analysis suggested that CXL had a favourable effect on blocking corneal melting in 85% of cases.139 CXL may offer great potential in the treatment of microbial keratitis as a primary as well as secondary therapy, especially given the increasing reports of anti-microbial resistance to antibiotics and reports of its usage in veterinary practice are also beginning to emerge.140,141
SummaryClinical studies of CXL have shown great promise in stabilizing keratoconus and post-refractive surgery ectasia. While further randomized, prospective and long-term follow up studies are necessary, it is very likely that in the future corneal ectasia can be halted at an early stage and the need for rigid contact lenses and keratoplasty avoided. Future refinement in techniques will allow for safer and more rapid procedure with less patient discomfort. Indications for cross-linking both in Ophthalmology and other branches of medicine will undoubtedly expand, with the potential use of CXL for microbial infections begin particularly exciting.
Conflict of interestThe authors have no conflicts of interest to declare.