The natural history of idiopathic abducens nerve paresis and the role of conservative management such as vision training during the recovery process is not well documented in the literature to the best of our knowledge. This case report presents the natural recovery process of idiopathic abducens nerve paresis in a young adult and the role of vision therapy in the recovery process.
Hasta la fecha, la historia natural de la paresia idopática del nervio abducens y la función de un tratamiento conservador como la terapia visual durante el proceso de recuperación no se hallan bien documentadas en la literatura. Este informe de un caso presenta el proceso de recuperación natural de la paresia idiopática del nervio abducens en un adulto joven, así como la función de la terapia visual en el proceso de recuperación.
Abducens nerve palsy is the most common of the ocular paresis in adults,1,2 with sudden onset of binocular horizontal diplopia as the bothersome symptom. Sixth cranial nerve palsies can be secondary to etiologies such as vascular, viral illness, inflammation, trauma, and undetermined in few cases. In younger patients it is important to rule out malignant causes such as life threatening neoplasms. The incidence of idiopathic sixth nerve palsies varies between 9.3 and 13.2/100,000 in the Caucasian population, with idiopathic reasons contributing to 26% of the total incidence.3 This case report deals with an acute onset esotropia due to abducens nerve paresis in a 25 year young adult presumably due to an idiopathic etiology or a viral illness. The natural history of the clinical presentation, findings, and role of vision therapy is emphasized through this case report.
Case historyA 25-year-old male presented with chief complaint of sudden onset, binocular horizontal, uncrossed diplopia during the past 1 week associated with eye pain in right eye. He also complained of vomiting and a radiating headache precipitated by stress, computer work and other near work. There was no history of significant systemic illness or any ocular or head injury, and he denied any recent viral illness. The local ophthalmologist had administered a 10-day course of Intravenous methyl prednisolone injection along with Tablet Prednisolone 5mg (10 tab/day) for three days. Brain imaging (MRI scan) had been done and was within normal limits.
Clinical findingsUncorrected visual acuity was 20/20, N6 @ 30cm in both eyes. Subjective and objective refraction revealed emmetropia. The Worth four dot test showed uncrossed diplopia for both distance and near. Cover test revealed a 35 prism diopter right esotropia at distance and a 25 prism diopters right esotropia at 40cm. Ocular motility showed mild restriction of abduction (−1) in the right eye and rest of the movements were full. There was no significant head posture. Rest of the ocular findings were within normal limits. MRI brain results (Plain and contrast) were within normal limits and no lesions/demyelination were identified. Diplopia charting identified the paretic muscle to be right lateral rectus. Binocular vision assessment revealed poor stereopsis, normal monocular accommodation, unmeasurable fusional vergence due to constant diplopia and reduced monocular accommodative facility and gradient AC/A ratio of 4:1. The diagnostic data is provided in Table 1. Due to constant diplopia and poor fusional ranges, a trial of prisms was recommended. The patient could fuse with 40 base-out Fresnel prisms in front of the right eye. As the patient was a frequent traveler he preferred using frosted glasses instead of Fresnel prisms.
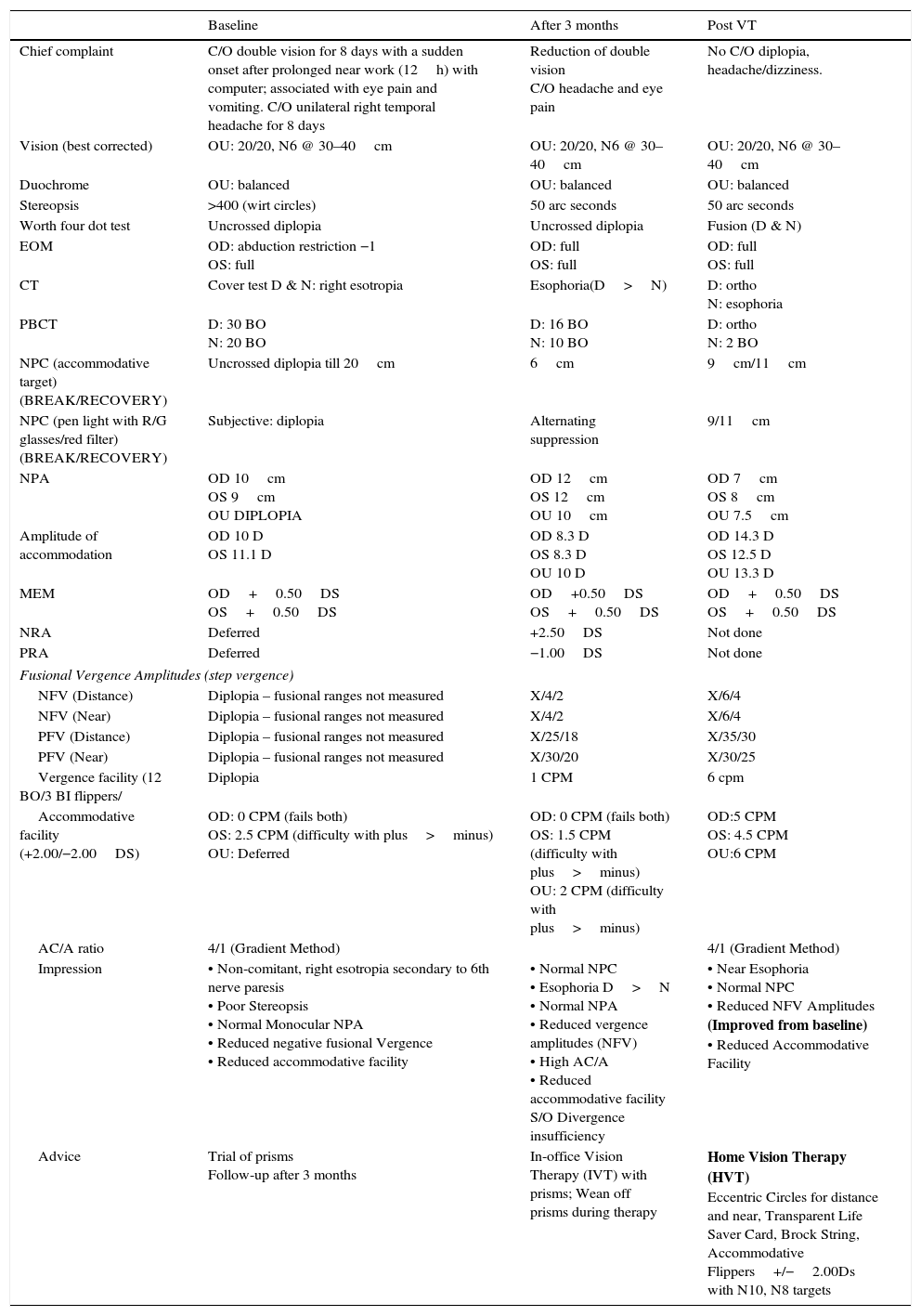
Clinical assessment details.
| Baseline | After 3 months | Post VT | |
|---|---|---|---|
| Chief complaint | C/O double vision for 8 days with a sudden onset after prolonged near work (12h) with computer; associated with eye pain and vomiting. C/O unilateral right temporal headache for 8 days | Reduction of double vision C/O headache and eye pain | No C/O diplopia, headache/dizziness. |
| Vision (best corrected) | OU: 20/20, N6 @ 30–40cm | OU: 20/20, N6 @ 30–40cm | OU: 20/20, N6 @ 30–40cm |
| Duochrome | OU: balanced | OU: balanced | OU: balanced |
| Stereopsis | >400 (wirt circles) | 50 arc seconds | 50 arc seconds |
| Worth four dot test | Uncrossed diplopia | Uncrossed diplopia | Fusion (D & N) |
| EOM | OD: abduction restriction −1 OS: full | OD: full OS: full | OD: full OS: full |
| CT | Cover test D & N: right esotropia | Esophoria(D>N) | D: ortho N: esophoria |
| PBCT | D: 30 BO N: 20 BO | D: 16 BO N: 10 BO | D: ortho N: 2 BO |
| NPC (accommodative target) (BREAK/RECOVERY) | Uncrossed diplopia till 20cm | 6cm | 9cm/11cm |
| NPC (pen light with R/G glasses/red filter) (BREAK/RECOVERY) | Subjective: diplopia | Alternating suppression | 9/11cm |
| NPA | OD 10cm OS 9cm OU DIPLOPIA | OD 12cm OS 12cm OU 10cm | OD 7cm OS 8cm OU 7.5cm |
| Amplitude of accommodation | OD 10 D OS 11.1 D | OD 8.3 D OS 8.3 D OU 10 D | OD 14.3 D OS 12.5 D OU 13.3 D |
| MEM | OD+0.50DS OS+0.50DS | OD+0.50DS OS+0.50DS | OD+0.50DS OS+0.50DS |
| NRA | Deferred | +2.50DS | Not done |
| PRA | Deferred | −1.00DS | Not done |
| Fusional Vergence Amplitudes (step vergence) | |||
| NFV (Distance) | Diplopia – fusional ranges not measured | X/4/2 | X/6/4 |
| NFV (Near) | Diplopia – fusional ranges not measured | X/4/2 | X/6/4 |
| PFV (Distance) | Diplopia – fusional ranges not measured | X/25/18 | X/35/30 |
| PFV (Near) | Diplopia – fusional ranges not measured | X/30/20 | X/30/25 |
| Vergence facility (12 BO/3 BI flippers/ | Diplopia | 1 CPM | 6 cpm |
| Accommodative facility (+2.00/−2.00DS) | OD: 0 CPM (fails both) OS: 2.5 CPM (difficulty with plus>minus) OU: Deferred | OD: 0 CPM (fails both) OS: 1.5 CPM (difficulty with plus>minus) OU: 2 CPM (difficulty with plus>minus) | OD:5 CPM OS: 4.5 CPM OU:6 CPM |
| AC/A ratio | 4/1 (Gradient Method) | 4/1 (Gradient Method) | |
| Impression | • Non-comitant, right esotropia secondary to 6th nerve paresis • Poor Stereopsis • Normal Monocular NPA • Reduced negative fusional Vergence • Reduced accommodative facility | • Normal NPC • Esophoria D>N • Normal NPA • Reduced vergence amplitudes (NFV) • High AC/A • Reduced accommodative facility S/O Divergence insufficiency | • Near Esophoria • Normal NPC • Reduced NFV Amplitudes (Improved from baseline) • Reduced Accommodative Facility |
| Advice | Trial of prisms Follow-up after 3 months | In-office Vision Therapy (IVT) with prisms; Wean off prisms during therapy | Home Vision Therapy (HVT) Eccentric Circles for distance and near, Transparent Life Saver Card, Brock String, Accommodative Flippers+/−2.00Ds with N10, N8 targets |
At the 3 month follow-up, diplopia had reduced considerably except in extreme right gaze. The frequency of the diplopia decreased, although diplopia persisted in right gaze, and this was stable for the past one month with no improvement noticed by the patient. Eyestrain and frontal headache were present with near work. On re-assessment, visual acuity was 20/20, N6 in both the eyes and worth four dot test showed fusion for distance and near. Stereopsis was 50 arc seconds with Randot stereo test. The cover test revealed a 16 PD esophoria at distance and 10 PD esophoria at near. Ocular motility was full, free and painless. Binocular vision assessment revealed improved vergence amplitudes compared to baseline. However, there were still significant reduced negative fusional vergence, and accommodative facility (Table 1). Although there has been considerable improvement probably due to spontaneous recovery, the NFV amplitudes and accommodative facility were still reduced and the patient was symptomatic. Considering no significant improvement over the past month, vision therapy was recommended to improve divergence amplitudes and to improve accommodative facility. Base out prisms were considered to facilitate training due to the large eso component. Three broad goals were established for vision therapy,4 developing divergence amplitudes for distance and near, improving accommodative facility (monocularly and binocularly), and improving saccadic/pursuit eye movements (due to diplopia in lateral gaze). On re-assessment at the end of 10 sessions, asthenopic symptoms were reduced, and no diplopia was noticed for distance and near. The patient demonstrated fusion for distance and near with the Worth four dot. The distance and near angles reduced significantly from 16 PD esophoria to orthophoria for distance and 2 PD esophoria at near. The diagnostic data at follow-up is provided in Table 1. The goals of vision therapy and details of vision therapy is sequenced in Tables 2 and 3 respectively. After 10 sessions of in-office vision therapy, he was advised to continue home-based therapy using the transparent Eccentric Circles, Life Saver Card, Brock string and accommodative flippers. A six month follow-up revealed stable alignment, and no symptoms with good compliance to home vision therapy.
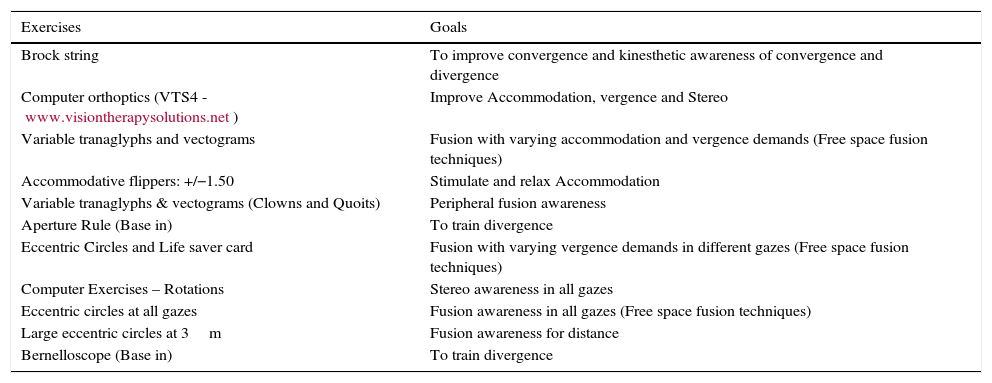
Goals of vision therapy.
| Exercises | Goals |
|---|---|
| Brock string | To improve convergence and kinesthetic awareness of convergence and divergence |
| Computer orthoptics (VTS4 - www.visiontherapysolutions.net) | Improve Accommodation, vergence and Stereo |
| Variable tranaglyphs and vectograms | Fusion with varying accommodation and vergence demands (Free space fusion techniques) |
| Accommodative flippers: +/−1.50 | Stimulate and relax Accommodation |
| Variable tranaglyphs & vectograms (Clowns and Quoits) | Peripheral fusion awareness |
| Aperture Rule (Base in) | To train divergence |
| Eccentric Circles and Life saver card | Fusion with varying vergence demands in different gazes (Free space fusion techniques) |
| Computer Exercises – Rotations | Stereo awareness in all gazes |
| Eccentric circles at all gazes | Fusion awareness in all gazes (Free space fusion techniques) |
| Large eccentric circles at 3m | Fusion awareness for distance |
| Bernelloscope (Base in) | To train divergence |
Details of vision therapy given at Each Session.
| Day1: Brock string, Computer orthoptics |
| Day2: Variable Tranaglyphs and Vectograms, Computer Orthoptics, Accommodative flippers: +/−1.50 |
| Day 3: Computer orthoptics, Variable Vectograms (Quoits), Accommodative flipper: +/−1.50 and rock |
| Day 4: Computer orthoptics, Variable Tranaglyphs & Vectograms (Quoits), Accommodative flipper: +/−1.50 and rock |
| Day 5: Variable Tranaglyphs (Quoits & Clowns), Computer orthoptics, Aperture Rule (Base in) |
| Day 6: Variable Tranaglyphs, Computer orthoptics-Stereo, Accommodative Flippers (+/−1.50D) |
| Day 7: Variable Vectograms (Clown), Computer exercise (Stereo), Brock string (in dextroversion and with rotation) |
| Day 8: Computer Orthoptics – Rotations, Transparent Eccentric Circles and Life saver card, Accommodative rock (VTS4) |
| Day 9: Brock String, Computer Exercises – Rotations, Eccentric circles at all gazes, Large transparent eccentric circles at 3m, Bernelloscope (Base in) |
| Day 10: Brock String rotation, Computer Exercises – Rotations, Eccentric circles at all gazes, Large eccentric circles at 3m, Aperture Rule (Base in) |
Acquired sixth nerve paresis is rare in young adults. The most common causes for non-traumatic sixth nerve paresis in children and adults include central nervous system mass lesions, demyelination and inflammation, vasculopathy, and multiple sclerosis.5,6 Idiopathic presentations in adults can account for up to 22% of cases.6 Spontaneous recovery of 6th nerve paresis is common (in almost 71% of affected individuals) in traumatic sixth nerve palsy at 6 months after onset,7–9 and the angle of deviation is the most important determining the prognosis.10 In our case, idiopathic or presumably a viral etiology was the most likely etiology. We utilized the sequential management approach suggested by Caloroso and Rouse (1993).11 Few case reports,12,13 have demonstrated the effectiveness of vision therapy in esotropia. Vision therapy improved the patient's range of fusion and thus significantly reduced the incidence of diplopia in both these patients. Saccadic peak velocities and latency are documented to be affected in sixth nerve palsies14 and hence saccadic training was thought to be constructive to improve saccades especially toward the paretic side. Though there is absence of quality data to suggest eye movement therapy may be helpful, from a physiological perspective we considered that this could be beneficial in preventing secondary contracture of the extraocular muscles. Also it has been well documented in literature that a high percentage of patients with a 6th nerve palsy show spontaneous remission that may take months. Thus, aggressive optometric treatment with prism, lenses, and vision therapy can help the patient be more comfortable during the time it takes for remission to occur, and also speed up the improvement in function. Though it could be argued that the natural history would allow for spontaneous resolving of symptoms even without active intervention, our case emphasizes the short course of vision therapy that could be of potential benefit and immediate relief to visually bothering symptoms of diplopia and asthenopia.
ConclusionVision therapy plays a significant role in improving fusional ranges, reduce asthenopic symptoms, and improve eye movements, thereby meeting the visual demands of the patient in idiopathic abducens nerve paresis. Thorough neurological investigations are required to rule out life threatening illness before commencing the therapy. Regular follow-ups and appropriate co-management are mandatory.
Conflicts of interestThe authors have no conflicts of interest to declare.