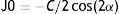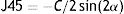To determine the agreement and validity of keratometric measurements in children with the Nidek ARK-510A auto-refractokeratometer compared to rotating Scheimpflug imaging with Pentacam and biograph with Lenstar LS 900.
MethodsThis study was conducted on 5620 schoolchildren aged 6–12 years in Shahroud, Iran. Minimum and maximum keratometry values and corneal astigmatism magnitude were compared by calculation of Paired difference, interclass correlation coefficient, and 95% limits of agreement (LoA) between devices.
ResultsAfter applying the exclusion criteria, 4215 right eyes were enrolled into the study. Mean minimum keratometry with Nidek ARK-510A, Pentacam, and Lenstar was 43.13±1.51, 43.14±1.48, and 42.87±1.46 diopters (D), respectively, and mean maximum keratometry was 43.97±1.59, 44.00±1.56, and 43.75±1.54D, respectively. Nidek ARK-510A overestimated minimum and maximum keratometry by 0.25±0.37 and 0.22±0.41, respectively, compared to Penatcam. The LoA between Nidek ARK-510A and Pentacam for minimum and maximum keratometry measurements were −0.98 to 0.47D and −1.02 to 0.57D, respectively. The LoA between Nidek ARK-510A and Lenstar for minimum and maximum keratometry measurements were −0.70 to 0.72D and −0.79 to 0.85D, respectively. The agreement between devices was best in emmetropes, worst in hyperopes. For astigmatic vector components, the agreements between devices were poor but best agreement was between Nidek ARK-510A and Pentacam.
ConclusionsKeratometry measurement with Nidek ARK-510A was not significantly different from Pentacam and Lenstar, and this device can be used in screening programs in emmetropes.
Determinar la concordancia y validez de las mediciones queratométricas en niños con el autorefractoqueratómetro Nidek ARK-510A, comparadas con las imágenes de Scheimpflug con Pentacam y el biómetro Lenstar LS 900.
MétodosEste estudio se realizó en 5.620 niños, de edades comprendidas entre 6 y 12 años, en Shahroud, Irán. Se compararon los valores queratométricos mínimo y máximo y la magnitud del astigmatismo corneal mediante cálculo de diferencia pareada, coeficiente de correlación inter-clase, y límites de comcordancia del 95% (LoA) entre dispositivos.
ResultadosTras aplicar los criterios de exclusión, se incluyeron 4.215 ojos derechos en el estudio. Los valores de queratometría mínima media con Nidek ARK-510A, Pentacam y Lenstar fueron de 43,13±1,51, 43,14±1,48, y 42,87±1,46 dioptrías (D), respectivamente, siendo los valores de queratometría máxima media de 43,97±1,59, 44±1,56, y 43,75±1,54D, respectivamente. Nidek ARK-510A sobre-estimó la queratometría mínima y máxima en 0,25±0,37 y 0,22±0,41, respectivamente, en comparación con Penatcam. El LoA entre Nidek ARK-510A y Pentacam para las mediciones de queratometría mínima y máxima fue de −0,98 a 0,47D y −1,02 a 0,57D, respectivamente. El LoA entre Nidek ARK-510A y Lenstar para las mediciones de queratometría mínima y máxima fue de −0,7 a 0,72D y −0,79 a 0,85D, respectivamente. El acuerdo entre dispositivos fue mejor en emétropes, y peor en hipermétropes. Para los componentes del vector astigmático, los acuerdos entre dispositivos fueron débiles, aunque existió una mejor concordancia entre Nidek ARK-510A y Pentacam.
ConclusionesLa medición de la queratometría realizada con Nidek ARK-510A no fue significativamente diferente a la realizada con Pentacam y Lenstar, pudiendo utilizarse este dispositivo en los programas de chequeo en emétropes.
Measuring the corneal curvature and refractive power with high accuracy and repeatability is one of the most important challenges in the examination of children. Correct measurement of corneal curvature in children is essential for fitting contact lenses, calculation of IOL power in aphakic children, or examining changes in the corneal shape during accommodation or with aging.1–4 Moreover, corneal astigmatism is known as an amblyogenic factor, therefore its screening would be helpful for identifying children at higher risk of amblyopia.5 In recent years, a variety of measurement devices have been introduced, and studies on variations of corneal curvature and shape with accommodation or age have reported contradictory results.2–4,6–9 The interpretation and comparison of findings of these studies is only possible after the repeatability and agreement of different keratometry methods have been examined. Multiple studies have been conducted to verify the accuracy, repeatability, and agreement of a variety of keratometry methods, and they provide very useful information to the examiner. Nevertheless, a very limited number of these studied investigated repeatability and agreement of different keratometry methods in children.10–12 Huynh et al. studied the repeatability and comparability of keratometry results between the RK-F1 auto-kerato-refractometer and the IOLMaster in 6-year-old children. Their findings indicated high repeatability in keratometric measurements in children, but the results of the two devices were not in agreement.11 Liang et al. compared non-cycloplegic keratometry readings with the handheld Nikon Retinomax K-Plus2 (Rmax) and the on-table Topcon KR8100 autokeratometers in two groups of children aged 2–12 years; they reported a high level of agreement between the two devices, albeit the agreement was lower after the cycloplegia was induced.12
Since keratometry is difficult in children due to their lack of cooperation,11 in this study we used Nidek ARK-510A autorefracto-keratometer, Pentacam HR, and Lenstar LS 900, which performs highly accurate measurements of the corneal curvature in less time compared to the manual method. Also, according to our review of available literature, there have been no studies on the agreement of keratotomy readings with these three devices in this age group. Should their results be comparable, the Nidek ARK-510A can be used when advanced devices such as Pentacam and Lenstar are not available for keratometry and follow up examinations. For this reason, the purpose of this report is to determine the agreement and interchangeability of Nidek ARK-510A with Pentacam and Lenstar in keratometry readings.
MethodsThe present report is part of the first phase of the Shahroud Children Cohort Study. The first phase of this study was conducted through a cross-sectional approach in 2015. In this phase, the target population was 6- to 12-year-old urban and rural children in Shahroud, northeast Iran.13
Given the small number of rural schoolchildren, the total population of rural elementary schoolchildren was selected, while in urban areas, schoolchildren were selected using random cluster sampling. In the urban area, schoolchildren were enrolled in 473 classrooms, and to achieve a sufficient sample size, 200 classes were randomly selected from among these 473 classes. Selected schoolchildren were invited to participate in the study on a scheduled date. Those who were willing to participate in the study were transferred to the examination site free of charge on their scheduled appointment day. First, parent consent was obtained, and after the interview, vision tests and anthropometric measurements were conducted for participating schoolchildren. Optometric examinations were performed by two trained optometrists under standard conditions.
For vision testing, first uncorrected visual acuity was first measured using the Nidek CP-770 projector chart at a distance of 3 meters. Then non-cycloplegic refraction was performed using the Nidek ARK-510A autorefracto-keratometer (Nidek Co. Ltd, Gammagori, Aichi, Japan). After refining the results through retinoscopy with the Heine Beta 200 (HEINE Optotechnic, Hersching, Germany), corrected visual acuity was measured, and subjective refraction was performed.
In the next step, biometric measurements were measured using the Allegro Lenstar LS 900 (WaveLight AG, Erlangen, Germany), and then Scheimpflug-based topography was done using the Pentacam HR (Oculus, Inc., Lynnwood, WA). To avoid the effect of diurnal variations, examinations were done at least 2h after waking time. All Keratometry measurements were performed under non-cycloplegic condition. Finally, cycloplegic autorefraction with Nidek ARK-510A, and retinoscopy were performed at least 30min after instilling 2 drops of cyclopentolate 1% at an interval of 5min.
Exclusion criteriaExclusion criteria were history of eye surgery or trauma, tropia, amblyopia, error in Pentacam measurements, pterygium, ptosis, congenital cataract, and those presenting as outliers in the data.
DefinitionsIn this study, refractive errors were based on cycloplegic autorefraction. Myopia was defined as a spherical equivalent (SE) of −0.5 diopter (D) or worse, and cases with an SE of +2.0D or more were marked as hyperopic. Corneal astigmatism was defined as the difference between steep minus the flat meridians. Vector analysis in polar coordinates was measured by using a Fourier transformation as below.
where C is the cylindrical power and α is the cylindrical axis in radians. The J0 (Cartesian astigmatism) refer to a cross-cylinder set orthogonally at 90° and 180° and the J45 (oblique astigmatism) refer to a cross-cylinder with axes at 45° and 135°.14Statistical analysisIn this study, the minimum and maximum keratometry readings with the three devices – Nidek ARK-510A, Pentacam and Lenstar – were analyzed. Minimum and maximum keratometry data with these three devices were summarized as mean and standard deviation. We also analyzed corneal astigmatism magnitude and mean and standard deviation of J0 and J45 components. The intraclass correlation coefficient (ICC) between every two pairs of these devices was determined. To determine the agreement between pair devices, the 95% limits of agreement (LoA) were calculated as the mean difference±1.96×standard error of the differences, and illustrated using the Bland–Altman plot.
Ethical considerationsThe protocol of this study was approved by the Ethics Committee of Shahroud University of Medical Sciences which adheres to the principles of the Declaration of Helsinki. All parents signed informed consents for the participation of their children in the study, and all schoolchildren were willing to participate.
ResultsOf the 6624 selected schoolchildren, 5620 participated in the study. After applying the exclusion criteria, data from 4222 schoolchildren were used in the analysis. In this sample, the mean age of the schoolchildren was 9.24±1.72 years (from 6 to 12 years), and 53.8% (n=2266) were boys.
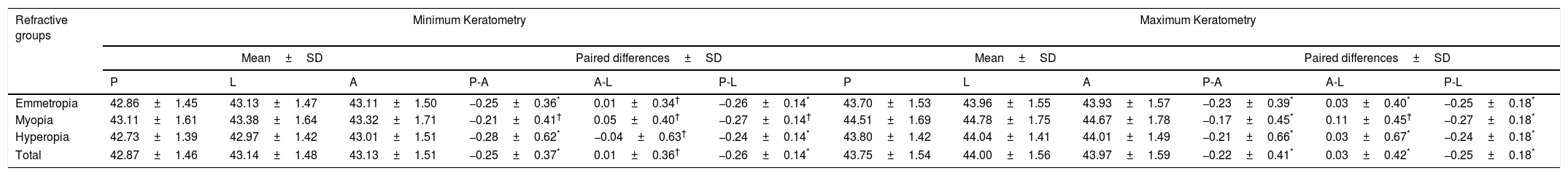
Pentacam and Nidek ARK-510ATables 1 and 2 show the minimum and maximum keratometry readings obtained from Nidek ARK-510A and Pentacam. As presented in Table 1, comparison between minimum keratometry measurements with these two devices indicated that Nidek ARK-510A generates higher minimum keratometry readings in the total sample than Pentacam. When tested in refractive error groups, myopics showed the smallest difference between these two devices, and hyperopics had the largest difference (p<0.001).
Mean, standard deviation (SD), and paired differences (PD) of minimum and maximum keratometry measured with Nidek Auto-refractokeratometer 510A (A), Pentacam HR (P), and Lenstar LS 900 (L).
| Refractive groups | Minimum Keratometry | Maximum Keratometry | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean±SD | Paired differences±SD | Mean±SD | Paired differences±SD | |||||||||
| P | L | A | P-A | A-L | P-L | P | L | A | P-A | A-L | P-L | |
| Emmetropia | 42.86±1.45 | 43.13±1.47 | 43.11±1.50 | −0.25±0.36* | 0.01±0.34† | −0.26±0.14* | 43.70±1.53 | 43.96±1.55 | 43.93±1.57 | −0.23±0.39* | 0.03±0.40* | −0.25±0.18* |
| Myopia | 43.11±1.61 | 43.38±1.64 | 43.32±1.71 | −0.21±0.41† | 0.05±0.40† | −0.27±0.14† | 44.51±1.69 | 44.78±1.75 | 44.67±1.78 | −0.17±0.45* | 0.11±0.45† | −0.27±0.18* |
| Hyperopia | 42.73±1.39 | 42.97±1.42 | 43.01±1.51 | −0.28±0.62* | −0.04±0.63† | −0.24±0.14* | 43.80±1.42 | 44.04±1.41 | 44.01±1.49 | −0.21±0.66* | 0.03±0.67* | −0.24±0.18* |
| Total | 42.87±1.46 | 43.14±1.48 | 43.13±1.51 | −0.25±0.37* | 0.01±0.36† | −0.26±0.14* | 43.75±1.54 | 44.00±1.56 | 43.97±1.59 | −0.22±0.41* | 0.03±0.42* | −0.25±0.18* |
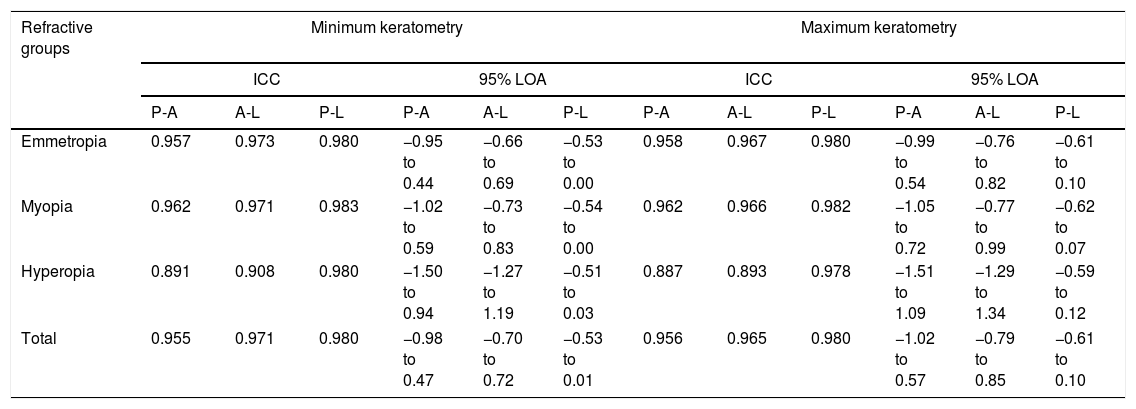
Interclass correlation coefficient (ICC) and 95% limit of agreement (LOA) for minimum and maximum keratometry in measurements by Nidek Auto-refractokeratometer 510A (A), Pentacam HR (P), and Lenstar LS 900 (L).
| Refractive groups | Minimum keratometry | Maximum keratometry | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ICC | 95% LOA | ICC | 95% LOA | |||||||||
| P-A | A-L | P-L | P-A | A-L | P-L | P-A | A-L | P-L | P-A | A-L | P-L | |
| Emmetropia | 0.957 | 0.973 | 0.980 | −0.95 to 0.44 | −0.66 to 0.69 | −0.53 to 0.00 | 0.958 | 0.967 | 0.980 | −0.99 to 0.54 | −0.76 to 0.82 | −0.61 to 0.10 |
| Myopia | 0.962 | 0.971 | 0.983 | −1.02 to 0.59 | −0.73 to 0.83 | −0.54 to 0.00 | 0.962 | 0.966 | 0.982 | −1.05 to 0.72 | −0.77 to 0.99 | −0.62 to 0.07 |
| Hyperopia | 0.891 | 0.908 | 0.980 | −1.50 to 0.94 | −1.27 to 1.19 | −0.51 to 0.03 | 0.887 | 0.893 | 0.978 | −1.51 to 1.09 | −1.29 to 1.34 | −0.59 to 0.12 |
| Total | 0.955 | 0.971 | 0.980 | −0.98 to 0.47 | −0.70 to 0.72 | −0.53 to 0.01 | 0.956 | 0.965 | 0.980 | −1.02 to 0.57 | −0.79 to 0.85 | −0.61 to 0.10 |
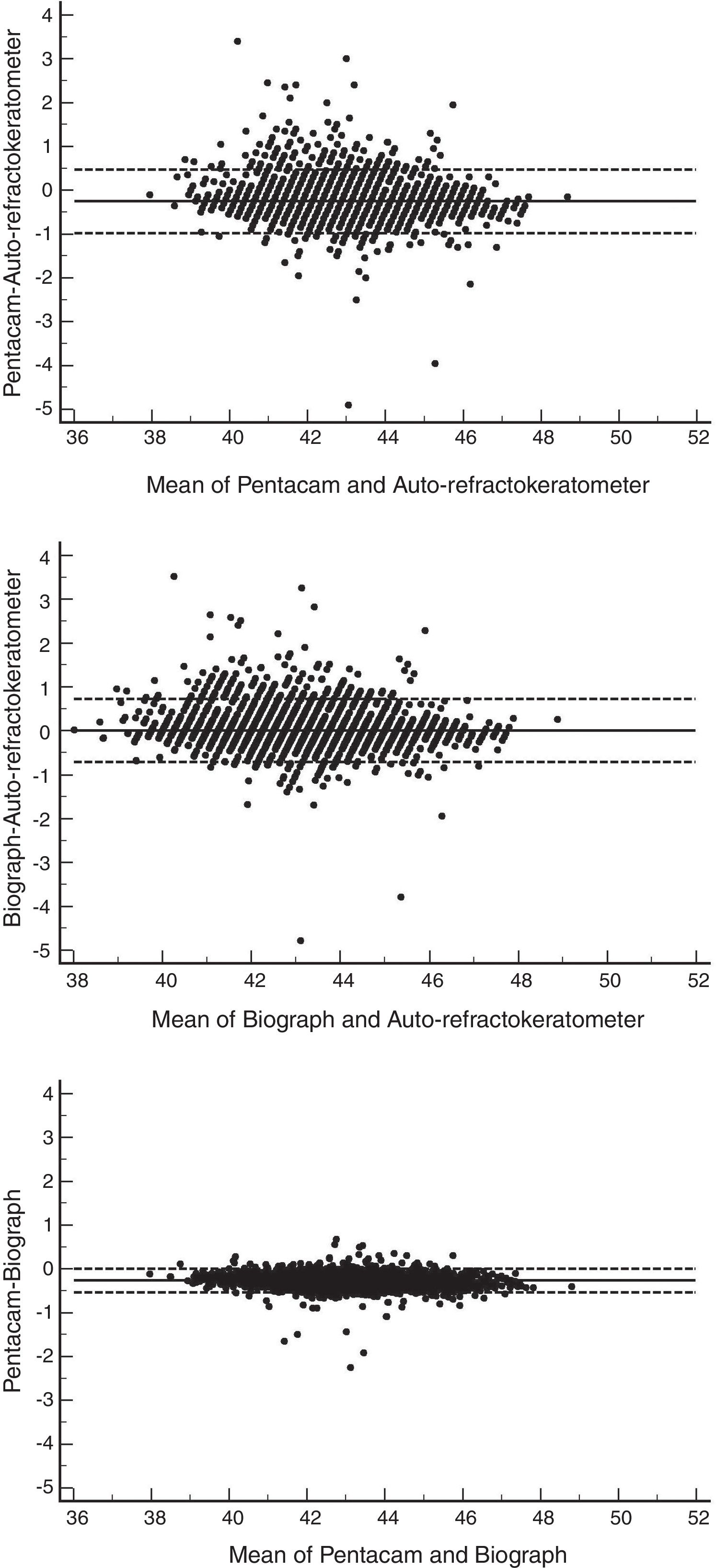
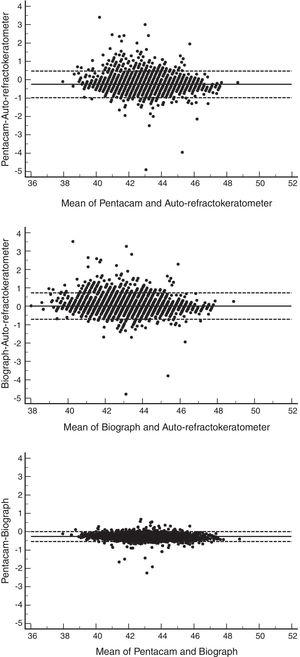
The ICC between the two devices for minimum keratometry readings was 0.955; the highest ICC was 0.962 as observed in myopics, and the lowest ICC was 0.891 which was observed in the hyperopic group. As illustrated in Fig. 1, the 95% LoA between these two devices in minimum keratometry measurement was −0.98 to 0.47D; the best and worst agreement was among the emmetropic and hyperopic groups, respectively.
Comparison of these two devices with respect to maximum keratometry readings showed that Nidek ARK-510A generates higher maximum keratometry values compared to Pentacam. In different refractive error groups, the smallest difference was observed among myopics.
The ICC between the Nidek ARK-510A and Pentacam was 0.956 for maximum keratometry measurements; as presented in Table 1, it was highest in myopics (0.962) and lowest in hyperopics (0.887). The LoA between these two devices in maximum keratometery readings was −1.02 to 0.57D; the narrowest and widest LoA was observed in the emmetropic group and the hyperopic group, respectively.
Lenstar LS 900 and Nidek ARK-510AAs presented in Table 1, ARK and Lenstar differences in minimum keratometry measurements (0.01±0.36) (p=0.125) were very small. These results did not differ significantly after breaking them down by type of refractive error.
The ICC between the two devices in measuring the minimum keratometry was 0.971, and as the results in Table 2 indicate, the highest ICC was 0.973 in the emmetropic and the lowest ICC was 0.908 in the hyperopic group. The 95% LoA for these two devices was −0.70 to 0.72; this was narrowest in the emmetropic and widest in the hyperopic groups. Fig. 1 illustrates the Bland–Altman plot of the agreement between these two devices for minimum keratometry readings.
In terms of maximum keratometry, Nidek ARK-510A generated higher readings than Lenstar, and the inter-device difference was statistically significant (p<0.001). A similar difference was also observed in refractive error groups, especially myopes. The ICC between the two devices in reading the maximum keratometry was 0.982. The highest ICC was 0.967 in emmetropes and myopes and the lowest was 0.893 in hyperopes.
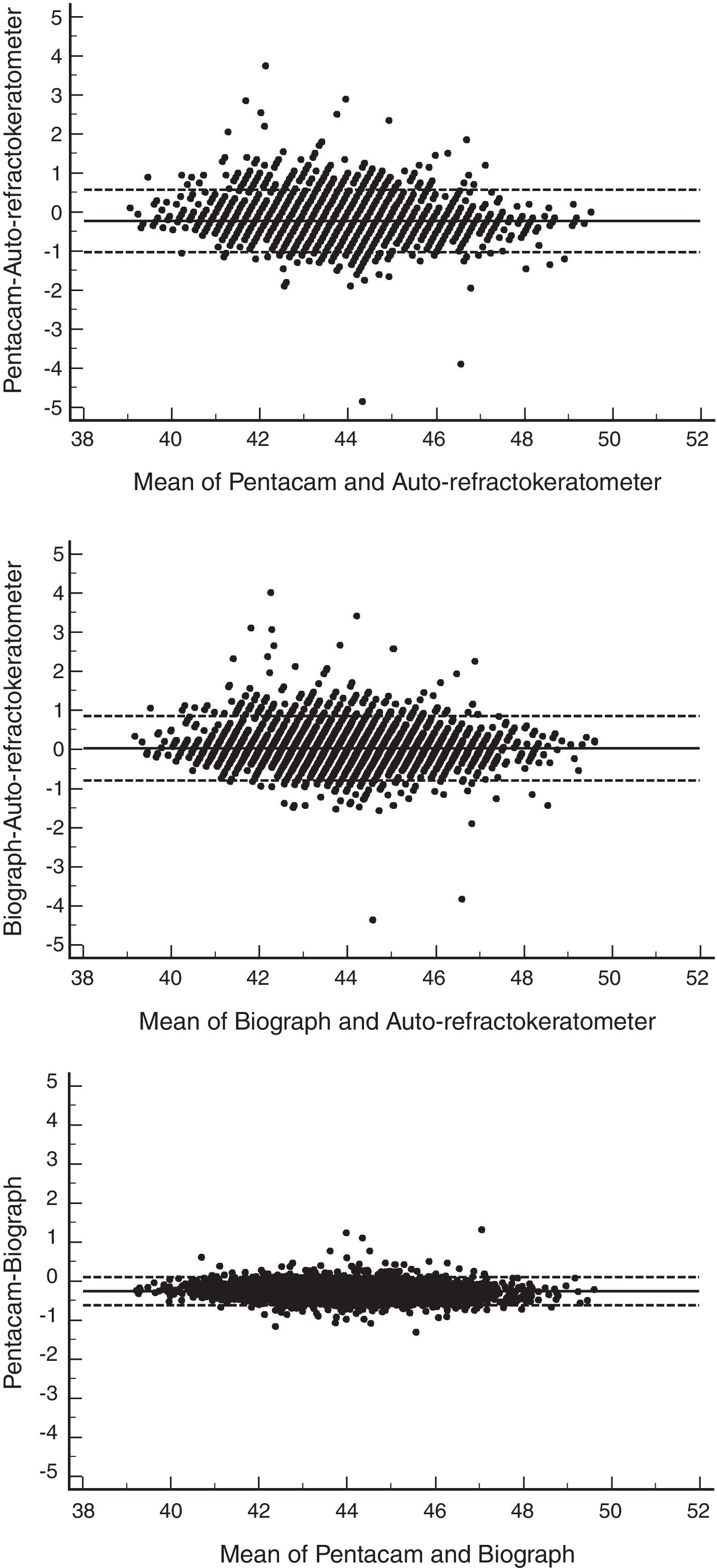
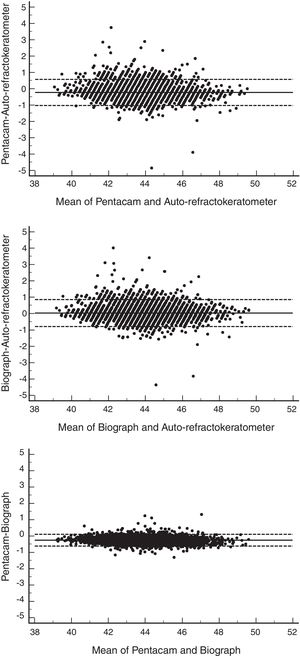
The limits of agreement in the total sample were from −0.79 to 0.85; in groups of refractive error, the LoA was narrowest in the emmetropes and widest in the hyperopes group. Fig. 2 illustrates the agreement between ARK and Lenstar in the measurement of maximum keratometry.
Pentacam and Lenstar LS 900Table 1 presents the minimum and maximum keratometry readings with Pentacam and Lenstar. The minimum keratometry readings measured with Pentacam were lower than those generated by Lenstar (p<0.001). The ICC between these two devices for minimum keratometry reading was 0.980; this was 0.980 in emmetropes and hyperopes, and 0.983 in myopes (Table 2). The 95% limits of agreement between the two devices in reading minimum keratometry were −0.53 to 0.01. Fig. 1 illustrates the Bland–Altman plot for the agreement between these two devices in measuring the minimum keratometry. The widths of the agreement limits between the two devices for minimum keratometry readings were quite similar in groups of myopes, emmetropes, and hyperopes.
Comparison of the two devices in the measurement of maximum keratometry readings indicated that Lenstar measurements of maximum keratometry were higher than Pentacam (p<0.001). The ICC between the two devices in the measurement of maximum keratometry was 0.980 in the total sample, 0.982 in myopes, 0.980 in emmetropes, and 0.978 in hyperopes.
The 95% LoA between the two devices in the measurement of maximum keratometry was from −0.61 to 0.10 for the total sample; results were not very different when calculated for different types of refractive errors. Fig. 2 shows the Bland–Altman plot for the agreement between the two devices in maximum keratometry readings.
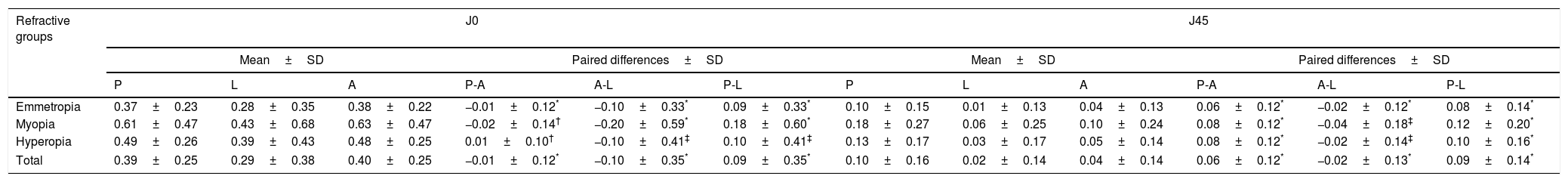
Corneal astigmatismTable 3 represents Mean, standard deviation, and paired differences of J0 and J45 of corneal astigmatism measured with Nidek ARK-510A, Pentacam, and Lenstar. According to the table, for J0 component, the smaller difference was between Pentacam and Nidek ARK-510A, and the greatest difference was between Nidek ARK-510A and Lenstar. As shown in Table 4, the highest ICC was between Pentacam and Nidek ARK-510A and the lowest was between Nidek ARK-510A and Lenstar. Also, the 95% LoA between the Nidek ARK-510A and the Pentacam was better than the other comparisons. The paired differences and 95% LoA were higher in myopes compared to other refractive groups.
Mean, standard deviation (SD), and paired differences of J0 and J45 of corneal astigmatism, measured with Nidek Auto-refractokeratometer 510A (A), Pentacam HR (P), and Lenstar LS 900 (L).
| Refractive groups | J0 | J45 | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean±SD | Paired differences±SD | Mean±SD | Paired differences±SD | |||||||||
| P | L | A | P-A | A-L | P-L | P | L | A | P-A | A-L | P-L | |
| Emmetropia | 0.37±0.23 | 0.28±0.35 | 0.38±0.22 | −0.01±0.12* | −0.10±0.33* | 0.09±0.33* | 0.10±0.15 | 0.01±0.13 | 0.04±0.13 | 0.06±0.12* | −0.02±0.12* | 0.08±0.14* |
| Myopia | 0.61±0.47 | 0.43±0.68 | 0.63±0.47 | −0.02±0.14† | −0.20±0.59* | 0.18±0.60* | 0.18±0.27 | 0.06±0.25 | 0.10±0.24 | 0.08±0.12* | −0.04±0.18‡ | 0.12±0.20* |
| Hyperopia | 0.49±0.26 | 0.39±0.43 | 0.48±0.25 | 0.01±0.10† | −0.10±0.41‡ | 0.10±0.41‡ | 0.13±0.17 | 0.03±0.17 | 0.05±0.14 | 0.08±0.12* | −0.02±0.14‡ | 0.10±0.16* |
| Total | 0.39±0.25 | 0.29±0.38 | 0.40±0.25 | −0.01±0.12* | −0.10±0.35* | 0.09±0.35* | 0.10±0.16 | 0.02±0.14 | 0.04±0.14 | 0.06±0.12* | −0.02±0.13* | 0.09±0.14* |
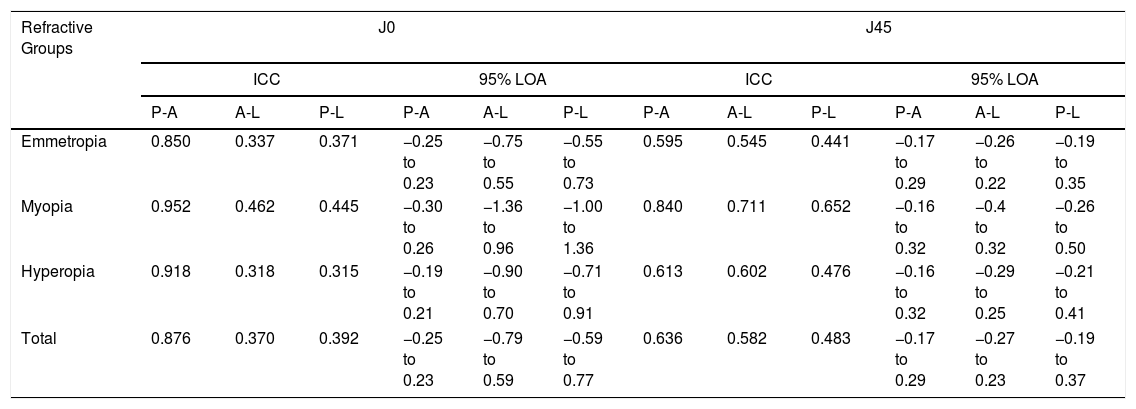
Interclass correlation coefficient (ICC) and 95% limit of agreement (LOA) for J0 and J45 of corneal astigmatism in measurements by Nidek Auto-refractokeratometer 510A(A), Pentacam HR (P), and Lenstar LS 900(L).
| Refractive Groups | J0 | J45 | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ICC | 95% LOA | ICC | 95% LOA | |||||||||
| P-A | A-L | P-L | P-A | A-L | P-L | P-A | A-L | P-L | P-A | A-L | P-L | |
| Emmetropia | 0.850 | 0.337 | 0.371 | −0.25 to 0.23 | −0.75 to 0.55 | −0.55 to 0.73 | 0.595 | 0.545 | 0.441 | −0.17 to 0.29 | −0.26 to 0.22 | −0.19 to 0.35 |
| Myopia | 0.952 | 0.462 | 0.445 | −0.30 to 0.26 | −1.36 to 0.96 | −1.00 to 1.36 | 0.840 | 0.711 | 0.652 | −0.16 to 0.32 | −0.4 to 0.32 | −0.26 to 0.50 |
| Hyperopia | 0.918 | 0.318 | 0.315 | −0.19 to 0.21 | −0.90 to 0.70 | −0.71 to 0.91 | 0.613 | 0.602 | 0.476 | −0.16 to 0.32 | −0.29 to 0.25 | −0.21 to 0.41 |
| Total | 0.876 | 0.370 | 0.392 | −0.25 to 0.23 | −0.79 to 0.59 | −0.59 to 0.77 | 0.636 | 0.582 | 0.483 | −0.17 to 0.29 | −0.27 to 0.23 | −0.19 to 0.37 |
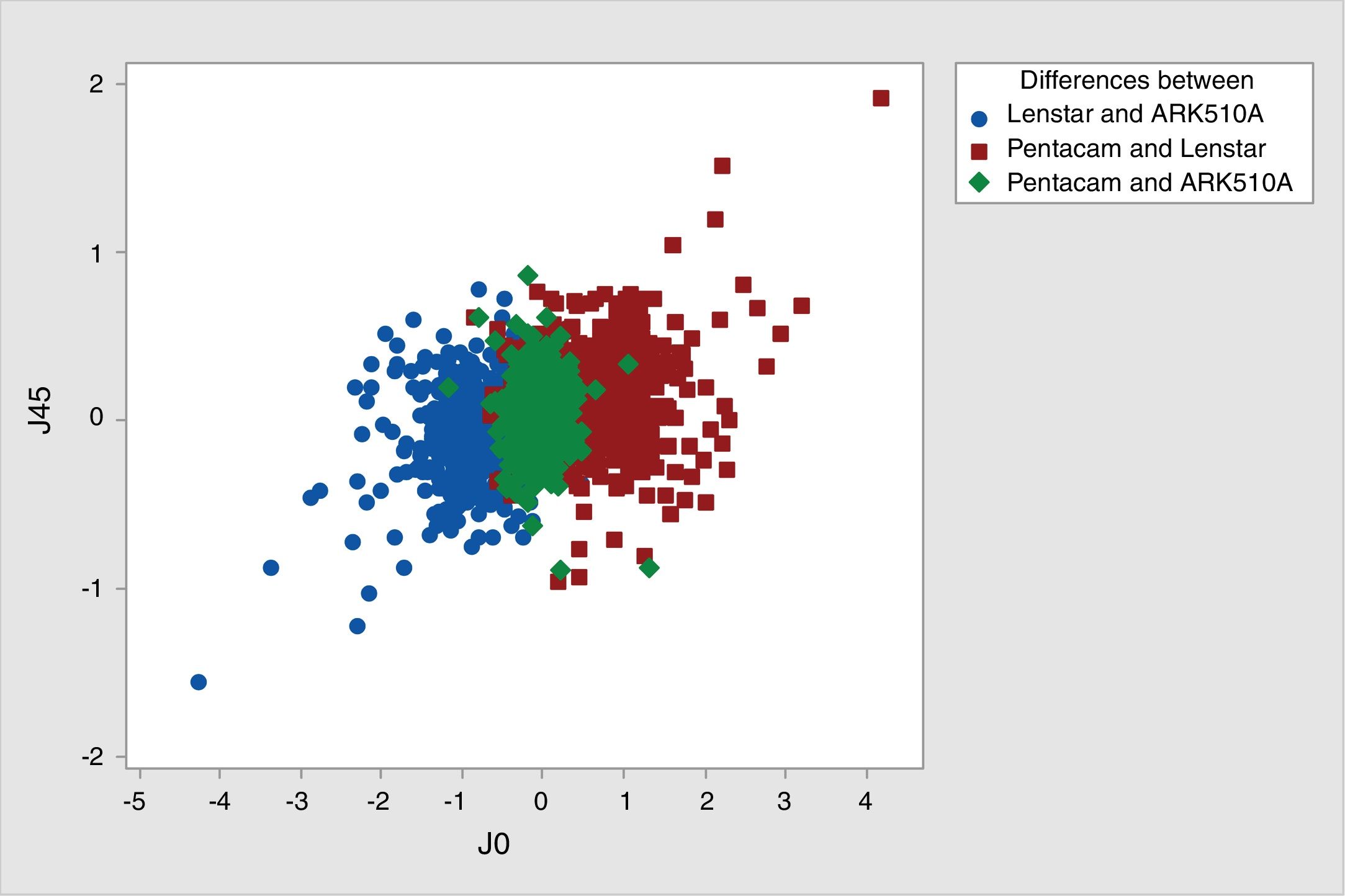
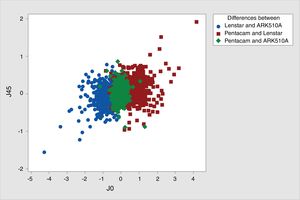
In the case of J45, the smaller difference was between Nidek ARK-510A and Lenstar, and the greatest difference was between Pentacam and Lenstar (Table 3). Moreover, the highest ICC was between Pentacam and Nidek ARK-510A, and the lowest ICC was between Pentacam and Lenstar (Table 4, Fig. 3).
DiscussionThe present study is one of the few studies to compare keratometry readings with 3 devices: Nidek ARK-510A, Pentacam, and Lenstar in children. Regarding the comparison of Pentacam and Lenstar, previous studies reviewed the correlation and interchangeability of these two devices in adults. Contrary to previous studies conducted in adults, the results of our study in 6–12-year old children showed that although readings with Lenstar were slightly higher than Pentacam, the agreement between them in minimum and maximum keratometry readings was very high, and their limits of agreement interval and the level of bias were almost the same in the total sample and in groups of different types of refractive error. This is while the limits of agreement were relatively wider for comparisons between Nidek ARK-510A and Pentacam and between Nidek ARK-510A and Lenstar.
In evaluating the agreement of the three devices for corneal astigmatism using vector analysis, the results of the present study showed that it was only high for J0 between Nidek ARK-510A and Pentacam.
The results of this study showed that keratometry values in both the steep and flat meridians were higher with the Lenstar than with Pentacam and Nidek ARK-510A. However, the inter-device difference for both meridians was smaller between Lenstar and Nidek ARK-510A, and there was no significant difference between the keratometry results with Lenstar and Nidek ARK-510A in the flat meridian. Also, mean keratometry in both flat and steep meridians were higher with Nidek ARK-510A compared to Pentacam. Various studies have compared keratometry results with devices such as Lenstar, Pentacam, and Auto-keratometer.15–23 However, none of these studies have focused on the 6- to 12-year-old age group. Moreover, few studies have assessed the comparability of astigmatic vector components24–26 and to the best of our knowledge; this is the first study to compare these astigmatic parameters between Nidek ARK-510A, Pentacam and Lenstar. Hashemi et al., studied the agreement of three devices (Lenstar, Pentacam and Nidek ARK-510A Auto-keratometer) in the 40- to 64-year old age group; results indicated that readings with Lenstar were about 0.5D steeper than Pentacam, those with the Auto-keratometer were 0.54D steeper than Pentacam, and the mean difference was smallest between Lenstar and Auto-keratometer (0.03 D).18 In other studies where Lenstar and Pentacam were compared, similar to the present study, Lenstar measurements of the steep and flat meridians were significantly higher than the results with Pentacam.20,22,23 The same trend was observed in studies comparing Auto-keratometer and Pentacam, and similar to the present study, Auto-keratometer measurements of the steep and flat meridians were higher than the results with Pentacam.17,18,21 Jasvinder et al. compared Lenstar and Auto-keratometer in 76 individuals with mean age of 54 years; similar to the present study, the inter-device difference was small, and Lenstar measured the cornea slightly steeper than the Auto-keratometer.27 The observed differences among devices can be due to differences in optic zone, the refractive index, the number of measured points, and the algorithm used in each device.
Auto-keratometers usually determine the corneal power based on measurements of 4–6 points in the central cornea. This central area varies from 2.25mm to 4mm depending on the type of keratometer. The Nidek ARK-510A examines only 4 points, each at a distance of 1.5mm from the Corneal Light Reflex in the center of the cornea, and thus, the measurement is not based on the entire corneal surface.28 Lenstar performs keratometry on two concentric rings of 1.65 and 2.3 millimeters using a 32-point pattern.29 Pentacam examines two major perpendicular meridians in the 3mm central cornea to measure the corneal radius of curvature.30 Given that the corneal center is steeper than its periphery31 and Lenstar makes more central measurements compared to Nidek ARK-510A and Pentacam, a steeper corneal curvature can be expected with this method. Also, inter-device differences can be due to the use of different refractive indexes in their calculations. Lenstar applies different refractive indexes in different populations including 1.3315, 1.3320, 1.3360 and 1.3375.32 In this study, we used the refractive index of 1.3375. Buckhurst et al. suggest that using different refractive indexes with Lenstar and IOL Master can result in significant differences in the calculated corneal power from the measured curvature radius.33
In the present study, the calculated ICC for minimum and maximum keratometry indicated strong correlations among keratometry readings with the three devices, and the highest correlation was found between Lenstar and Pentacam. The high correlation among the three devices shows that all three devices have comparable accuracy in measuring the corneal curvature. Regarding astigmatic vector components, the comparability was only high for J0 between Nidek ARK-510A and Pentacam (ICC=0.876), with all other comparisons showing ICC<0.400. Also, the comparability of J45 between all three devices was notably low. While a correlation analysis compares the measurements performed by different devices, Bland–Altman's Analysis is used to demonstrate the interchangeability of devices.33 Accordingly, studying agreement intervals between devices in this study showed that for Keratometry measurements, Pentacam and Lenstar had the best agreement, and the weakest agreement was between Nidek ARK-510A and the other two devices. On the other hand, for astigmatic vector components, the best agreement was between Nidek ARK-510A and Pentacam (Fig. 3).
In general, according to the reported results, the agreement of the devices was better when we regard dioptric power of the cornea in comparison to astigmatic vector components. Since, corneal astigmatism magnitude was determined as the difference between the dioptric power of steepest and flattest meridians, the lower agreement of devices regarding astigmatic vector components could be due to the effect of corneal cylinder orientation. An inevitable disagreement reported in measuring axis location, despite a very good agreement of the evaluated devices (ARK and corneal topography) in measuring corneal power and the amount of astigmatism, confirms this issue.26
In the study by Hashemi et al. the 40–64-year age group, unlike the present study, the correlations between Lenstar and Pentacam and between Nidek ARK-510A and Pentacam were weak and agreements were poor. In their study, the best correlation and agreement was between Nidek ARK-510A and Lenstar. Although the levels of correlation and agreement between the Nidek ARK-510A and Lenstar in their study were similar to the present study, as mentioned, the highest ICC and agreement in the present study was observed between Lenstar and Pentacam.18 The main reason for the difference between these findings appears to be the age of the subjects in the two studies.
In a study by Elbaz et al. on 11 subjects with a mean age of 56 years, the correlation between keratometry readings with Nidek ARK-510A and Pentacam was high (r=0.889), but the wide LOA between the two devices (2.54) suggested that they should not be used interchangeably.17 Modis et al. also found similar results in examining the agreement between the two devices.21 Although the agreement between these two devices was lower in the mentioned studies than in the present study, the results of present study also indicated that Nidek ARK-510A and Pentacam are not interchangeable for keratometry measurements.
Huang et al. studied Lenstar and Pentacam keratometry in 108 individuals in the age range between 18 and 32 years. Similar to the results of the present study, there was a high correlation between the two devices and the reported agreement interval was closer to the present study compared to other studies.20 Nonetheless, they concluded that the two devices should not be used interchangeably in this age group. The results of other studies on the agreement between Lenstar and Pentacam confirmed that the two devices cannot be used interchangeably,22,23 while the findings of the present study in the 6–12-year age group indicated that there was a fairly high agreement between the two devices. The reason for these differences is probably the difference in the mean age of the studied populations. Hashemi et al. have suggested that, when using Lenstar, it might be necessary to use different refractive indexes for calculating the keratometry in different age groups.18 Of course, the weak agreement may be due to a small sample size that widens the limits through its influence on the standard deviation, and the large sample size of the present study should be considered as an important strength of the study.
The present study is the first to compare device correlation and agreement in different groups of refractive errors. In this regard, Pentacam and Lenstar, which had the best correlation and agreement, showed similar results in different types of refractive errors. Comparisons of Nidek ARK-510A with Lenstar and Pentacam showed lower agreement and correlation in cases with hyperopia than those with myopia and emmetropia. Similarly, the ICC and agreement of all devices for astigmatic vector components was higher among myopic than hyperopic groups. These results confirm our assumption that accommodation affects corneal curvature during auto-keratometry in this age group, especially in hyperopic children. Given the different targets used in these three devices, it may be argued that, in this age group, accommodation is stimulated to a greater degree during measurements with the Nidek ARK-510A compared to the other two devices which use optical targets. On the other hand, each device used in this study examines a different optic zone and different regions of the cornea. Given the different effects of accommodation on different regions of the cornea,4,7,34 changes in Nidek ARK-510A results, especially in the hyperopic group, may be due to the active accommodation in this age group, the relative stimulation of accommodation during measurements with this device, or the greater effect of accommodation in the corneal areas examined by this device. Therefore, Nidek ARK-510A is not a suitable substitute for Pentacam and Lenstar in this age group, especially in children with hyperopia which is one of the most common refractive errors in this age group. The change in the agreement between handheld Nikon Retinomax K-Plus2 (Rmax) and on-table Topcon KR8100 Auto-keratometers before and after cycloplegia observed in the study by Liang et al. on the 2–12-year age group also confirms the role of accommodation in corneal curvature variations in children.12
The strength of the present study was the large sample size in children's age group. Given the importance of achieving accurate measurements of corneal curvature in children, especially for contact lenses fitting, IOL power calculations in aphakic children or examining structural and dimensional corneal changes in studies looking into myopia progression, repeatability studies of these devices in children are recommended. Considering the effect of accommodation on the corneal curvature and the wide range of accommodation in this age group, a study before and after cycloplegia is recommended to compare device agreement with and without cycloplegia. Moreover, evaluating the agreement of keratometry results between open-field auto-refractokeratometer and these devices (especially before and after cycloplegia) can help to clarify the role of accommodation on corneal curvature and is also recommended. Since open-field auto-refractokeratometer produces less instrument myopia or proximal accommodation than that of conventional auto-refractokeratometer in which the target is inside the instrument, it is expected to show better agreement than conventional auto-refractokeratometer.
Finally, the results of this study indicate that there is no clinical difference between keratometry measurements with Nidek ARK-510A and Pentacam or Lenstar, and this device can be used to determine keratometry in children screening programs. However, these three devices are not interchangeable in evaluation of corneal astigmatism. It should be also noted that the best measurements with Nidek ARK-510A are achieved in emmetropics, and results of three devices are not interchangeable in hyperopics.
Financial supportShahroud School Children Eye Cohort Study is funded by the Noor Ophthalmology Research Center, Tehran, Iran; and Shahroud University of Medical Sciences, Shahroud, Iran (Project number: 9329).
Conflicts of interestThe authors have no conflicts of interest to declare.