To present a new iris pigmentation classification system based on comparison of iris pigmentation to a set of 24 standard eye photographs, with the aim of gaining on accuracy and on applicability for retinal straylight studies.
MethodsA reference set of 24 eye photographs was established by ranking the photographs from least (number 1) to most (number 24) iris pigmentation. Reproducibility was tested by grading a sample of 67 eye photographs with this reference set.
ResultsThe overall variation between observers was 1.46 on a scale of 0 to 25.
ConclusionThe new method is promising to be more accurate than existing iris color classification systems in clinical situations where objective colorimetry-based systems are not available. The method may be useful to assess iris translucency and fundus reflectance as sources of variation in retinal straylight.
Presentar un nuevo sistema de clasificación de la coloración del iris basado en la comparación de la pigmentación del iris con un conjunto de referencia formado por 24 fotografías de ojos, con el objetivo de lograr una mayor precisión y una mayor aplicabilidad del mismo en los estudios sobre la luz dispersa (parásita) que llega a la retina.
MétodosSe ha establecido un conjunto de 24 fotografías de ojos, ordenadas de menor (fotografía número 1) a mayor (fotografía número 24) según la cantidad de pigmentación del iris. Para evaluar la reproducibilidad de este sistema, se utilizó una muestra compuesta por 67 fotografías de ojos. Varios observadores asignaron a cada una de las fotografías un valor de la escala de coloración, utilizando para ello el mencionado conjunto de referencia.
ResultadosLa variación global entre observadores fue igual a 1,46, en una escala de 0 a 25.
ConclusionesEl nuevo método parece que puede llegar ser más preciso que los actuales sistemas de clasificación de la coloración del iris en aquellas situaciones de la práctica clínica donde no se dispone de sistemas objetivos basados en colorimetría. El método puede resultar útil para evaluar la translucidez del iris y la reflectancia del fondo de ojo como posibles orígenes de la variabilidad que existe entre sujetos de la cantidad de luz dispersa (parásita) que alcanza la retina.
It is known from studies in the past that the amount of pigmentation in the eye wall and fundus influences the quality of the image on the retina of the normal human eye. Two main reasons were identified: part of the light projected on to the retina is not absorbed but is reflected back into the eye by the layers of the fundus,1 and the fact taht the eye wall, including the iris, is not optically opaque.2 Both effects depend on the amount of pigmentation in the fundus and the eye wall respectively. The light originating from fundus reflectance and eye wall translucency does not partake in proper image formation on the retina, but is scattered in the eye to create a veil of light over the retinal image. Together with scattered light originating from optical imperfections in the cornea and the crystalline lens, this light is referred to as retinal straylight. The scatter-induced light veil reduces the contrast of the retinal image and may lead to impairment of the visual function. When this impairment is caused by bright lights at a distance, such as headlights of oncoming cars when driving at night, the term “disability glare” is used.
In previous studies the color of the eye (iris color) was used as an indicator for eye pigmentation. Blue-eyed caucasians were found to have higher retinal straylight values compared to pigmented brown-eyed non-caucasians, leading to the conclusion that pigmentation is a source of variation in straylight in normal eyes.2,3 Van den Berg et al.4 showed that this pigmentation dependence is partly caused by variations in transmission of light through the ocular wall. For dark-brown eyes of pigmented individuals transmission was found to be two orders of magnitude lower than for blue-eyed individuals. Furthermore, the authors speculated that variations in fundus reflectance are also partly responsible for pigmentation dependence of straylight, which was later investigated more thoroughly by Vos and van den Berg.1 The study of van den Berg et al.4 also showed that variation in pigmentation on the blue side of the eye color spectrum has much more influence on the straylight value than variation on the brown side. This can be understood by realizing that the contribution of straylight originating from fundus reflectance and eye wall translucency to the total amount of straylight is larger for less pigmented blue eyes than for well pigmented brown eyes.
To better understand the variation in optical quality of the eye in the normal population, and to be able to more accurately identify sources of increased retinal straylight in pathological eyes, the amount of fundus reflectance and eye wall translucency would need to be estimated, ideally by measuring these two factors directly. However, the techniques to do this are not readily available for most clinicians. Therefore, it would be desirable to have a relatively simple and straightforward way to assess these factors in a clinical environment. Grading of iris color seems to be an obvious candidate.
For iris color to be used as reliable measure of eye pigmentation, its classification should be standardized. In most studies, iris color was subdivided in either 2 (light/dark,5-9 blue/brown,10,11 or light-very light/black-brown12), 3 (blue/grey-green/brown,13,14 blue/mixture of brown, grey, green and/or yellow/brown,15 blue/grey-green-mottled/brown,16 blue/brown/other,17 blue-grey/green-hazel/brown-black,18 or blue/green/brown19), 4 (grey/blue/hazel/brown,20 blue/grey-green/hazel/brown,21 blue/hazel/brown/indeterminate,22 or blue/brown/green/hazel23), 5 (blue/grey/green/hazel/brown24,25 or blue/hazel/green/brown/black26), or 6 (blue/green/hazel/brown/black/not clear27) categories, to be assessed by the investigator and/or the subject. An extensive line of research has been devoted to the effects of prostaglandin analogs and prostamides on iris pigmentation.28,29 These are drugs used as ocular hypotensive agents in glaucoma patients. Most of these studies used 8, 9 or 10 iris color categories, based on a method introduced by Alm and Stjernschantz.30
These classification systems, which can be characterized by the term “color naming”, are very subjective, since they do not involve comparison of the eye color to some kind of standardized reference. To improve on this situation, iris color classification systems based on a comparison with some kind of color standard, such as a color chart with 331 or 1127 colors, 15 painted glass anterior eye segments,32 3 pictures of artificial eyes,33 or the 5-grade Boys-Smith pigment gradation lens,34 have been used. Also, sets of standardized photographs of real eyes have been used as a reference. Moss et al.35 used a reference set of 6 red reflex photographs, obtained with dilated pupils. In the Beaver Dam Eye Study, a set of 3 reference photographs was defined,36 to be practically used to classify eye color in 337 or 438 categories. A modified version was used to define 5 categories.39 Seddon et al.40 developed a system with 4 reference photographs (5 categories), that was also used in later studies.41-43
Most of these grading systems use 2 to 5 categories for eye color, which is too coarse (discretisation error too high) to discern the subtle differences on the blue side which are expected to induce relatively strong variations in retinal straylight, as explained above. In the last decade some objective classification systems have been proposed, based on automated image analysis by a computer using a calibrated software package (Bee WH, et al. IOVS 1997;38:ARVO Abstract 3797).44-48 Delori et al. (Delori FC, et al. IOVS 1991;32:ARVO Abstract 2333) explored the use of iris reflectometry as a potential tool for the evaluation of iris pigmentation. These methods offer objective and accurate ways to measure iris color. However, they are not readily available for most clinicians.
In this article, we present a new system for the classification of iris pigmentation, based on the comparison of iris pigmentation to a set of 24 standard photographs. It is intended to be a quick and easy-to-use system that is more accurate than the existing systems. A similar system for the evaluation of diffuse atrophy of the retinal nerve fiber layer was proposed earlier.49 To be precise, color is a bit of a misnomer for iris classification, because color is essentially a two-dimensional system, while the iris is rarely homogeneous in color. Therefore, we chose to develop a classification system based on (subjective) estimation of iris pigmentation, intended to give a one-dimensional quantity.
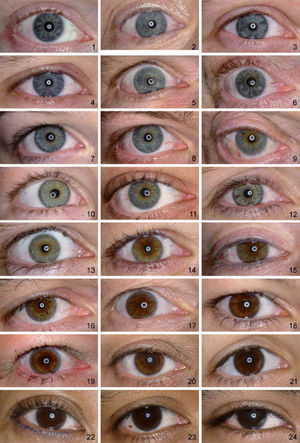
MethodsThe eyes of 32 volunteers were photographed with a Sony DSC-S75 digital camera under standardized illumination conditions and camera settings (eyes illuminated by a ring-shaped light derived by fiber optics from a halogen lamp, no flash, shutter speed 1/60 s, ISO value 200, fixed white balance). The volunteers were recruited from coworkers and students within the institute. Care was taken that the whole spectrum of possible iris colors would be included. For the reference set, 24 out of 32 photographs were selected by one observer based on image quality and variation in iris color. Three of these 24 eyes were non-Caucasian. Institutional Review Board (IRB)/Ethics Committee decided that approval was not required for this study.
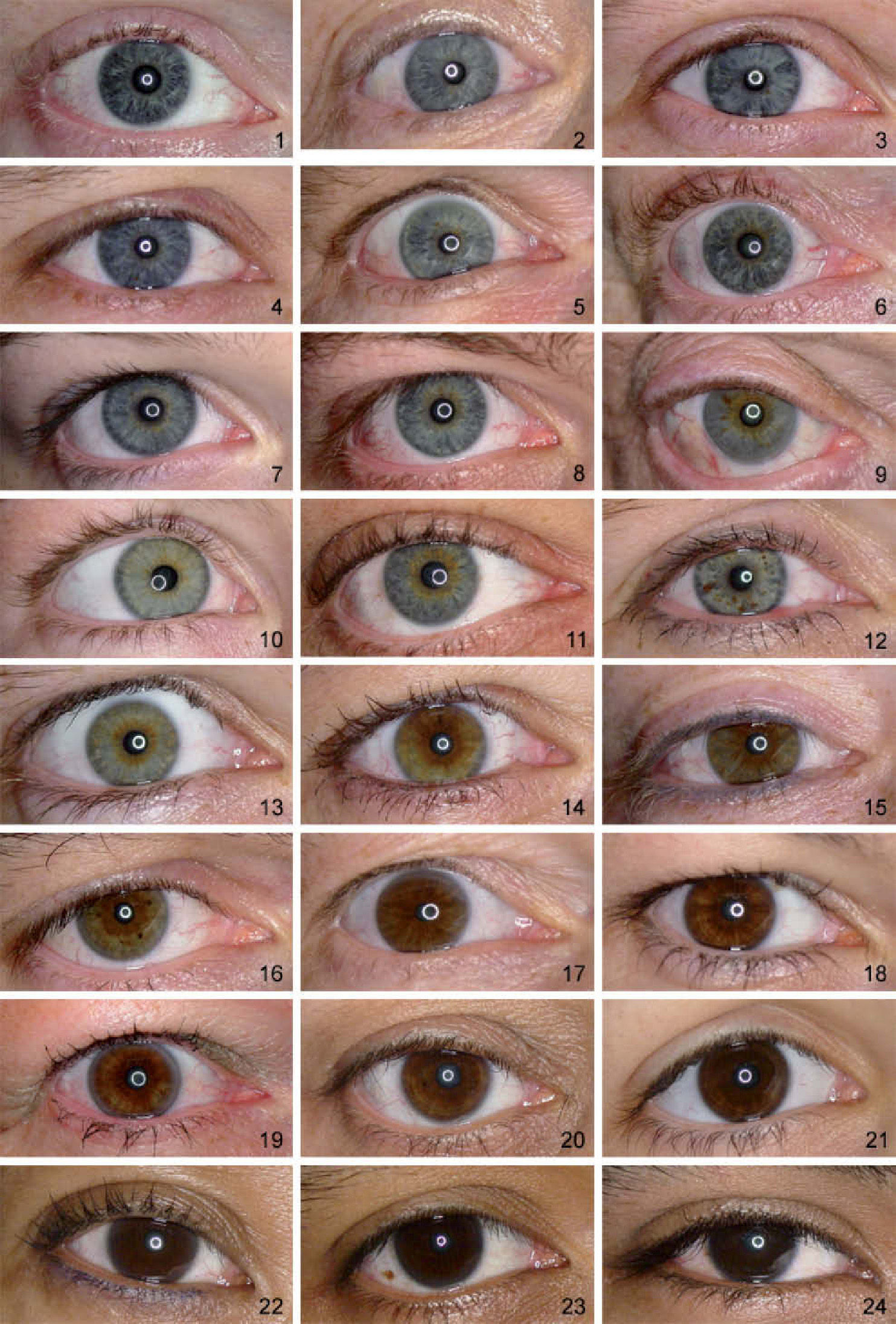
The 24 photographs were independently ranked from least (number 1) to most (number 24) average iris pigmentation by 4 observers with no color deficiencies. The final order for the reference set was determined by the mean scores of these 4 observers.
To investigate the reproducibility of this classification system, a test sample of 67 eye photographs (different from the ones used for the reference set) was graded according to the reference set by 4 observers with no color deficiencies, using a scale from 0 (zero discernable pigmentation) to 25 (darker than picture 24). The observers, of which two had also ranked the reference set, were asked to grade each test photograph on the scale created by the reference set in a global manner, as opposed to comparing each test photograph to each picture of the reference set in detail. The photographs in the test sample had a lower image quality and were taken under different illumination conditions than those in the reference set (compact digital camera with flash).
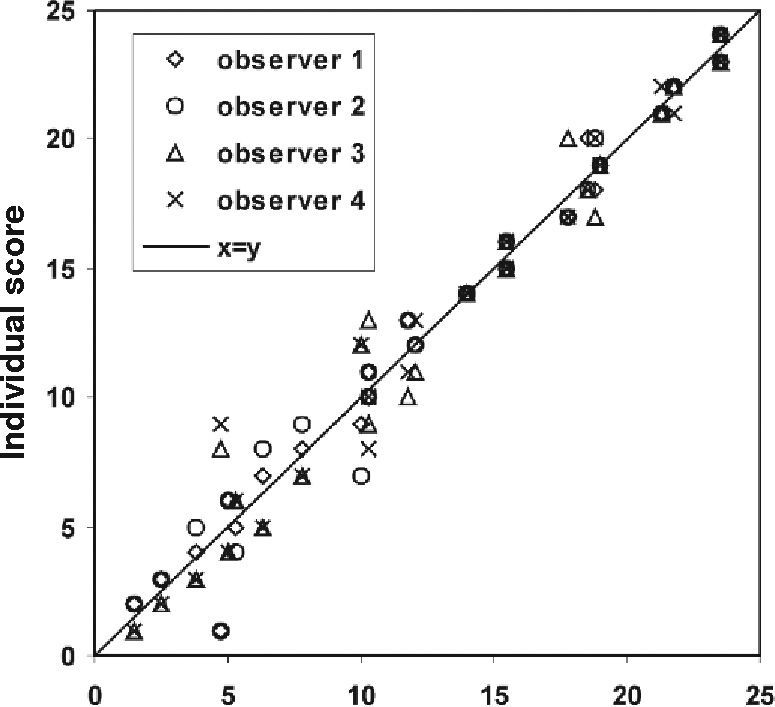
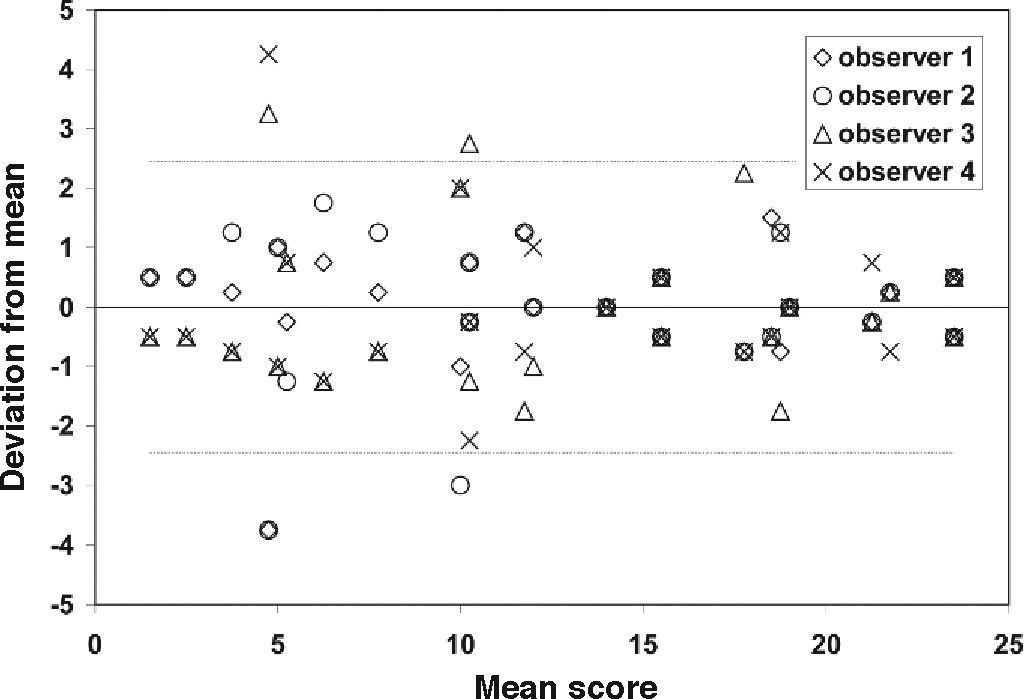
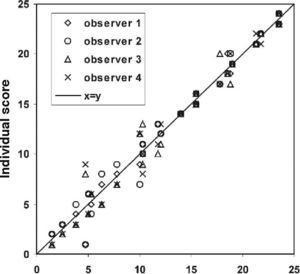
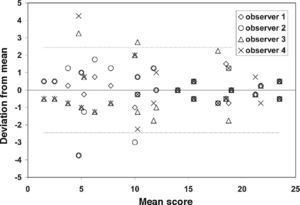
ResultsFigure 1 shows the individual ranking scores of the 24 reference photographs as a function of the mean score for each photograph. The deviations from the mean are given in figure 2. The overall standard deviation is 1.22. The figures show a higher spread of data points on the low side (bluish iris colors). The reference set of 24 photographs is presented in figure 3, ordered according to the average ranking of the 4 observers.
Similar to figure 1, only now the deviation from the mean is plotted against the mean score. The dashed lines represent the overall 95% confidence interval, based on an overall standard deviation of 1.22.
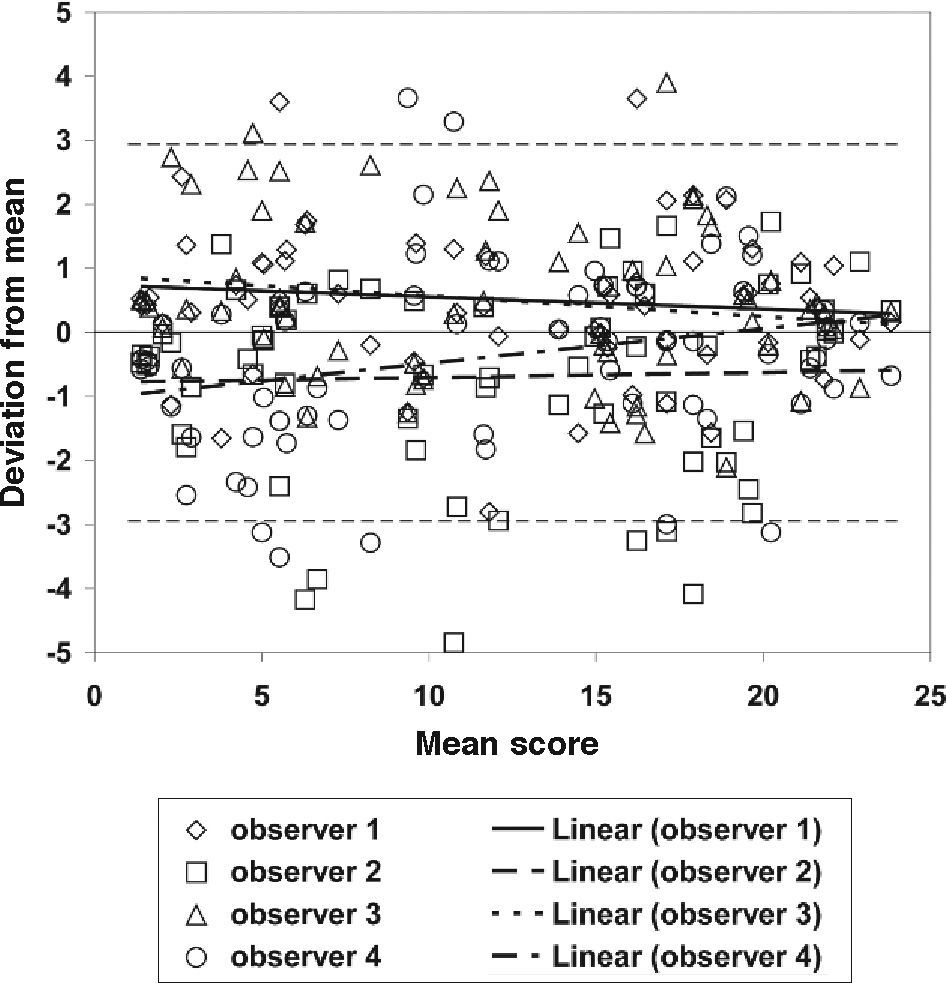
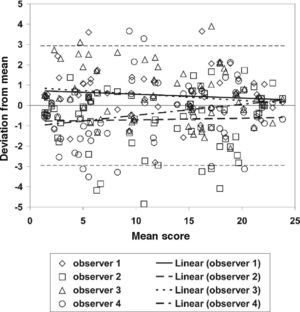
The deviations from the mean scores for the test sample of 67 photographs are plotted as a function of the mean score in figure 4. The overall standard deviation is 1.46. Part of this standard deviation is caused by small but statistically significant systematic differences between the 4 observers (average deviations 0.49, -0.68, 0.49, -0.31, respectively, corresponding to a standard deviation of these average deviations of 0.59). Linear trend lines are plotted for each observer.
Reproducibility of the iris classification procedure. The iris pigmentation in 67 eye photographs was evaluated by 4 observers using the reference photographs presented in figure 3. The deviation from the mean score is plotted against the mean score. The dashed lines represent the overall 95% confidence interval, based on an overall standard deviation of 1.46. To investigate systematic differences between observers, trend lines for the individual data sets are also plotted.
In this article, we presented a new classification system for iris pigmentation, using a set of 24 standard photographs as a reference. This system assesses iris pigmentation in a more quantitative way than the systems that have been used in the literature. Therefore, the new system might prove to be useful to gain more detailed knowledge about iris pigmentation, which is a source of variation for retinal straylight.
To establish the reference set of 24 photographs, some arbitrary choices had to be made. Since the photographs were chosen from a rather limited population sample, it is unclear to what extent the sample represents the whole population. Some areas in the range of iris pigmentations may be underor overrepresented in the chosen reference set. Furthermore, one might wonder whether the order would depend on the observers participating in the study. However, we are confident that these would be marginal effects.
We are strengthened in this assumption because a remarkable agreement between observers was found, in both the establishment of the order in the reference set (Figure 1and2), and the reproducibility test (Figure 4). The larger variation in data points on the low side (bluish iris colors) in figure 1 and 2 might suggest that it is more difficult to grade bluish than brownish iris colors. However, another explanation might be that in this reference set the differentiation of blue colors is more detailed than the differentiation on the brown side, giving rise to more noise on the blue side. In fact, this noise could be used to define a new reference set that has an equal accuracy over the whole scale, which would be desirable for general use of the system. For straylight applications, a more detailed reference set on the blue side might be useful, as explained in the introduction.
The overall standard deviation of 1.46 justifies the use of the relatively high amount of (24) categories for iris pigmentation. The (small) systematic difference in behavior between observers 1 and 3 on the one side and observer 2 on the other side might be caused by a different way of appreciation of the differences in image quality and general color appearance between the test sample and the reference set. The positive slope of observer 4 in figure 4 might indicate that this observer is more likely to use the extreme ends of the scale than the other observers.
The incentive for this study was the need for a relatively simple method to assess iris translucency and fundus reflectance as sources of variation in retinal straylight. Such a method was established by defining a reference set of eye photographs with different grades of iris pigmentation, containing more detail for the bluish colors than existing iris color grading systems. The scoring error of about 1.5 on a scale from 0 to 25 suggests a higher discriminative power than that of the existing systems, which have a higher discretisation error than this scoring error. However, we did not actually compare our method to the existing systems. We believe that our method can be an improvement over existing iris color classification systems in clinical situations where objective colorimetry-based systems are not available.