To compare the contributions of single vision (SVCL) and multifocal contact lenses (MFCL) to the relative peripheral refraction (RPR) profiles obtained via an autorefractor and an aberrometer in a pilot study.
MethodsTwo instruments, Shin-Nippon NVision K5001 (SN) and COAS-HD, were modified to permit open field PR measurements. Two myopic adults (CF, RB) were refracted (cycloplegia) under eight conditions: baseline (no CL); three SVCLs: Focus Dailies® (Alcon, USA), PureVision® (Bausch & Lomb, USA) and AirOptix® (Alcon, USA); and four MFCLs: AirOptix® (Alcon, USA), Proclear® Distant and Near (Cooper Vision, USA), and PureVision® (Bausch & Lomb, USA). CLs had a distance prescription of −2.00D and for MFCLs, a +2.50D Add was selected. Five independent measurements were performed at field angles from −40° to +40° in 10° increments with both instruments. The COAS-HD measures were analyzed at 3mm pupil diameter. Results are reported as a change in the relative PR profile, as refractive power vector components: M, J180, and J45.
ResultsOverall, at baseline, M, J180 and J45 measures obtained with SN and COAS-HD were considerably different only for field angles ≥±30°, which agreed well with previous studies. With respect to M, this observation held true for most SVCLs with a few exceptions. The J180 measures obtained with COAS-HD were considerably greater in magnitude than those acquired with SN. For SVCLs, the greatest difference was found at −40° for AirOptix SV (ΔCF=3.20D, ΔRB=1.56D) and for MFCLs it was for Proclear Distance at −40° (ΔCF=2.58D, ΔRB=1.39D). The J45 measures obtained with SN were noticeably different to the respective measures with COAS-HD, both in magnitude and sign. The greatest difference was found with AirOptix Multifocal in subject RB at −40°, where the COAS-HD measurement was 1.50D more positive. In some cases, the difference in the RPR profiles observed between subjects appeared to be associated with CL decentration.
ConclusionFor most test conditions, distinct differences were observed between the RPR measures obtained with the two modified instruments. The differences varied with CL design and centration. Although the pilot study supports the interchangeable use of the two instruments for on- and off-axis refraction in unaided eyes or eyes corrected with low/no spherical aberration; we advocate the use of the COAS-HD over the SN for special purposes like refracting through multifocal CLs.
Comparar la contribución de las lentes de contacto monofocales y de las lentes de contacto multifocales (LMF) a los perfiles de la refracción periférica relativa (RPR) obtenidos mediante un autorrefractómetro y un aberrómetro en un estudio piloto.
MétodosSe modificaron dos instrumentos, Shin-Nippon NVision K5001 (SN) y COAS-HD, para permitir las mediciones de la RP de campo abierto. Se refraccionó (bajo cicloplejía) a dos adultos miopes (CF, RB) bajo ocho situaciones: línea basal (sin LC); tres lentes monofocales: Focus Dailies® (Alcon, USA), PureVision® (Bausch & Lomb, USA) y AirOptix® (Alcon, USA); y cuatro LMF: AirOptix® (Alcon, USA), Proclear® dominnate (D) y no dominante (N) (Cooper Vision, USA), y PureVision® (Bausch & Lomb, USA). Las LC tenían una prescripción de distancia de -2,00D, y para las LMF se seleccionó una adición de +2,50D. Se realizaron cinco mediciones independientes a ángulos de campo comprendidos entre -40° y +40° en incrementos de 10° con ambos instrumentos. Las mediciones de COAS-HD se analizaron con un diámetro de pupila de 3mm. Los resultados se reportaron como cambios en el perfil de la RPR, como componentes del vector de potencia refractiva: M, J180, y J45.
ResultadosEn general, en la línea basal, las mediciones M, J180 y J45 obtenidas con SN y COAS-HD fueron considerablemente diferentes sólo para los ángulos de campo ≥±30°, lo que es plenamente coincidente con los estudios previos. Con respecto a M, esta observación fue cierta para la mayoría de las lentes monofocales con pocas excepciones. Las mediciones de J180 obtenidas con COAS-HD fueron considerablemente superiores en magnitud que aquellas adquiridas con SN. En las lentes monofocales, la mayor diferencia se halló a -40° para AirOptix SV (ΔCF=3,20D, ΔRB=1,56D), y en las LMF para Proclear D a -40° (ΔCF=2,58D, ΔRB=1,39D). Las mediciones de J45 obtenidas con SN fueron considerablemente diferentes a las mediciones respectivas con COAS-HD, tanto en magnitud como en signo. La mayor diferencia se halló en AirOptix Multifocal en el sujeto RB a -40°, donde la medición de COAS-HD reflejó un valor más positivo de 1,50D. En algunos casos, la diferencia en los perfiles de RPR observados entre los sujetos parece estar asociada a la descentralización de la LC.
ConclusiónPara la mayoría de las condiciones de la prueba, se observaron distintas diferencias entre las mediciones de la RPR obtenidas con los dos instrumentos modificados. Dichas diferencias variaron según el diseño y el centrado de la LC. Aunque el estudio piloto apoya el uso intercambiable de los dos instrumentos para la refracción dentro y fuera del eje en ojos sin ayuda, u ojos corregidos con aberración esférica baja/nula, abogamos por el uso de COAS-HD en lugar de SN para fines especiales tales como la refracción a través de LC multifocales.
Myopia progression has been associated with peripheral retinal image contour, in addition to several other factors of its multi-factorial etiology.1–4 Quantitative data on peripheral refraction could provide valuable insights into possible correlations between peripheral refraction and the emmetropization process or refractive error progression. Therefore, techniques that facilitate rapid and reliable peripheral refraction measurements have attracted great attention over the last decade.5–7 Two commercial instruments commonly used for such applications are the Shin-Nippon NVision K5001 (SN, Grand-Seiko, Japan) autorefractor and the Complete Ophthalmic Analysis System (COAS-HD) aberrometer (Wavefront Sciences, USA). The SN autorefractor has a near infrared ring-like target that illuminates the test eye and the reflected irradiation from the retina is imaged onto a sensor.8 A lens in the relay system of the reflection path automatically adjusts to always have the captured image in an approximate focus. The size and shape of the ring image is then analyzed to provide second order refraction. The working principle of the COAS-HD utilizes a Hartmann–Shack wavefront sensor and is well described elsewhere.9 Clearly, the operational principles of these instruments are different; the later considers multiple data points in the given working radius to yield refraction from Zernike polynomials, as opposed to the former which uses only ∼2.3mm ring for computation of the refractive state of the eye.8 However, both have been validated for their use in on- and off-axis applications; and it has been previously reported that good agreement exists between their measures for both applications, at least in unaided eyes.10
The different working principles of the SN autorefractor and COAS-HD aberrometer suggest that they may generate different refractive results for eyes fitted with multifocal contact lenses. A simple pilot study was conducted, using a reduced model eye. Five refraction readings were recorded using both the SN and the COAS-HD when the emmetropic model eye was fitted with a well-centered single vision spectacle lens (−1.00D). As expected, the magnitudes of the readings, produced by both the instruments were close to the power of the spectacle lens. The same measurements were then repeated after a 1.25mm diameter hole had been drilled in the center of the single vision spectacle lens. Unexpectedly, the measurements obtained by the autorefractor were identical to those obtained in the previous test case. However, this observation did not hold true for the COAS-HD results. Considering a single vision spectacle lens with a central hole could effectively represent a concentric bifocal contact lens, these results suggested that if the SN was to be used for obtaining refraction through bi-/multifocal lenses then the data from the center of the optic zone is likely to be ignored. This intriguing effect prompted a more thorough investigation into the reliability of both instruments under conditions of non-uniform power distribution across the pupil.
Further, in recent years, more research has been dedicated toward novel lens designs for myopia that alter peripheral refraction with the intention to control myopia progression.11,12 This has led to the use of the mentioned instruments for evaluating the peripheral refractive state of the eye through such specialty lenses.11,13,14 Recalling that most of these lenses have some sort of multifocality incorporated; this study was designed to compare the contributions of single vision (SVCL) and multifocal contact lenses (MFCL) to the relative peripheral refraction (RPR) profiles as measured with the SN autorefractor and the COAS-HD aberrometer.
MethodsThe protocol followed the tenants of the declaration of Helsinki and the research was approved by the local institutional human ethics committee with ratification from the University of New South Wales, Sydney (Approval 10/12). Both instruments, the SN and COAS-HD were modified to permit open-field PR measurements using the head turn approach.15 For the modification of the SN, an instrument head with several small red laser diodes was mounted on top of the instrument, which allowed fixation targets to be presented onto a distant wall in visual field angles ranging from −40° to +40° in 10° steps. To facilitate peripheral measurements, the working distance of COAS-HD was extended by using a unit-magnification relay pair (125mm EFL achromatic doublets, Thorlabs, Newark, NJ). Four supplementary infrared LEDs (840nm, RS Australia) facilitated the required additional illumination of the test eye. The tolerance to pupil misalignment decreases with increasing field angle16; therefore appropriate care was taken by the operators to keep the alignment within 0.50mm of the visible pupil to avoid any clinically significant errors in the refraction measurements. A wide-angle, physical model eye (shown in Fig. 1) configured at two different refractive states (−3D myopia and 0D emmetropia) was measured at various visual field angles, spanning 0° to +50° in 10° steps. A human participant cyclopleged with Tropicamide 1% (w/v) (Chauvin Pharmaceuticals, UK) was measured at visual field angles, spanning −30° to +30° in 10° steps. Each of these conditions when considered as independent test cases constituted 19 candidates for determining accuracy, repeatability and reproducibility of the modified systems.
Ten independent repeats were made on the test cases to validate the modified instruments and also assess the agreement between two operators, A and B. Assessment of the agreement between operators was performed using inter-class coefficients (ICC). After validation, two other-wise healthy myopic adults, the authors CF (Rx: −0.75DS) and RB (Rx: −5.75DS–0.75DC×170°), were characterized as the experienced participant and observer for each other, respectively.
Participants were refracted under the following eight conditions: baseline (no CL), three SVCLs: Focus Dailies® (Alcon, USA, TX), AirOptix® (Alcon, USA, TX) and PureVision (Bausch & Lomb, USA, NJ); and four MFCLs; AirOptix® (Alcon, USA, TX), Proclear® D and N designs (Cooper Vision, USA, CA), and PureVision® (Bausch & Lomb, USA, NJ). All CLs had a distance prescription of −2.00° D. MFCLs had an add power of +2.50° D. Both, the SN and COAS-HD instruments had been fitted with a series of red laser diodes. These light pointers sequentially generated fixation targets at the wall of the clinic room at 0°, 10°, 20°, 30° and 40° viewing angles on both left- and right-hand sides. The participants-to-fixation-target distances were ∼2.50m. Five independent repeats of the PR measurements were performed only on the right-eyes of the participants, at nine different field angles from −40° to +40° in 10° increments, using both SN and COAS-HD. All measurements were made under cycloplegia (Tropicamide 1.0% (w/v), Chauvin Pharmaceuticals, UK). Completion of the experiment required three 8-h sittings for each participant. It is known that the t1/2 of Tropicamide 1.0% (w/v) is only a few hours. Drops were therefore administered three times in 2.5h intervals for every sitting to ensure stable cycloplegia throughout the measurements. Custom-written Matlab® routines were used to reverse the 180° rotation of the wavefront caused by the lens relay pair added to the COAS-HD. For the PR measures obtained with COAS-HD only the central 3mm of the wavefront was considered for calculation. As the eyes were dilated, no extrapolation of the wavefront was required for any field eccentricity. For both instruments, results are reported as a change in the relative PR profile (RPR) in terms of refractive power vectors M, J180, and J45.17 Due to the small sample size, no statistical analyses were performed to compare the differences in the measures obtained with SN and COAS-HD, only trends were reported.
The centration of the contact lens (CL) was recorded in primary gaze using a Nikon SLR Camera (Nikon, Japan) mounted on the slit-lamp (Zeiss, Germany). Attempts to automatically detect the CL edge failed due to inherent low contrast of the CL edge against the white sclera background. Therefore, a manual method had to be implemented for determining the position of the correcting CL with respect to the horizontal visible iris diameter (HVID). A known size rectangular grid (15mm×15mm) with 1mm grid intervals was printed on cardboard to constitute the calibration card. This card was photographed with the current set-up to determine the ‘pixel to mm’ scale factor of the system. Once determined, this factor was applied to all post-processed images to derive real world co-ordinates. A dedicated custom-written Matlab® routine facilitated the post processing of these images. It involved the following two steps: (a) identifying the HVID manually and (b) identifying the CL edge manually. Once the image is loaded onto the user interface, the user is prompted to select at least eight points on the HVID and later eight additional points on the visible CL edge. Best circles are fitted through those selected points via least-squares method providing the information on the centers of the respective circles. The difference between the center of the correcting CL and HVID (i.e. CL decentration) was denoted in a right-handed co-ordinate system (X, Y); where X is the horizontal decentration (in mm) of the correcting CL and Y is the vertical decentration (in mm) of the correcting CL with respect to the HVID.
ResultsThe accuracy for on-axis refraction measured with SN and conventional COAS-HD setup were within 0.20D, 0.10D, and 0.10D for components M, J180 and J45, respectively. Measurements (M) obtained with extended COAS-HD demonstrated excellent correlation with those obtained from conventional setup (y=1.042x−0.155, R2=0.993, p<0.05). Good agreement was observed between the two experienced investigators (CF and RB) as noted in Table 1 by the inter-class coefficients for each refractive component for both, COAS-HD and SN.
The inter-class coefficients for each refractive component while performing the measurements on the model eye and human subjects with (a) the COAS-HD aberrometer and (b) Shin-Nippon autorefractor.
| ICC for each refraction component | COAS-HD extnModel eye (95% CI) | COAS-HD extnHuman participant (95% CI) | Shin-NipponModel eye (95% CI) | Shin-NipponHuman participant (95% CI) |
|---|---|---|---|---|
| M | 0.989 (0.983–0.992) | 0.917 (0.856–0.953) | 0.996 (0.994–0.998) | 0.780 (0.635–0.872) |
| J180 | 0.998 (0.997–0.999) | 0.903 (0.830–0.945) | 0.996 (0.993–0.997) | 0.869 (0.775–0.926) |
| J45 | 0.780 (0.690–0.848) | 0.897 (0.821–0.942) | 0.806 (0.696–0.879) | 0.768 (0.616–0.865) |
The coefficients of repeatability (intra-observer variability) of observers A and B for the validation measures were 0.88, 0.54 and 0.60 and 0.96, 0.62 and 0.48, for the refraction components M, J180 and J45, respectively. The coefficients of reproducibility (inter-observer variability) for the same measures were 1.68, 0.92 and 0.80. These coefficients were derived by using the equation (coefficient of repeatability=1.96×SD, where SD is the maximum within-subject standard deviation). Contact lens centration was determined from the slit-lamp images. Centration was generally better on participant CF than on RB. The mean±SD of CL centration for all seven lenses, determined with respect to the HVID, was (0.05±0.13mm, −0.05±0.21mm) and (0.38±0.15mm, −0.29±0.31mm), for participants CF and RB, respectively. Figs. 2–7 show the refraction components: M, J180, and J45 of the two participants CF (in column 1) and RB (in column 2) as a function of visual field eccentricity using both the modified systems SN and COAS-HD, for various test conditions. In all the plots, (+) sign indicates nasal visual field, while (−) sign indicates temporal visual field. The standard deviations of the average within-subject variability are indicated by the error bars and they are generally lower for the modified COAS-HD measurements. The results are presented in three sub-sections as guided by the measures of three refractive power vectors.
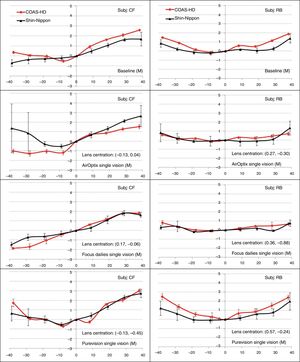
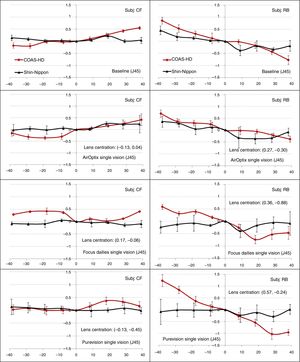
Mean spherical equivalent (M)At baseline, the M measures obtained with COAS-HD were more positive than those obtained with SN for both subjects; however were considerably different only at field angles ≥30°. With subject CF, there was considerable asymmetry in the M vector between the temporal and nasal visual fields, while participant B had an almost symmetric profile. With the single vision CLs, there were only two cases with noticeable differences across the entire profile: for participant CF corrected with the AirOptix single vision CL, the M measures from the COAS-HD were more negative than those obtained from the SN, and for participant RB corrected with the PureVision single vision CL where the SN measured more negative than the COAS-HD (Fig. 2).
Line plots of the mean spherical equivalent (M) measures of two subjects CF (column 1) and RB (column 2), as function of horizontal visual field eccentricity, for baseline condition (unaided eye) and when the test eye was corrected with different single vision contact lenses. Lens centration is given in (x, y)mm. In the plot, (+) sign indicates nasal visual field, while (−) sign indicates temporal visual field. Error bars represent the standard deviations of the average within-subject variability.
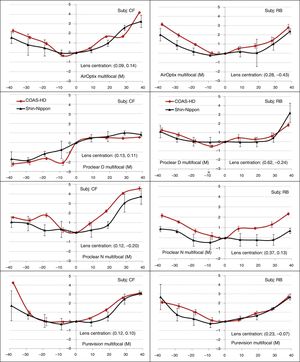
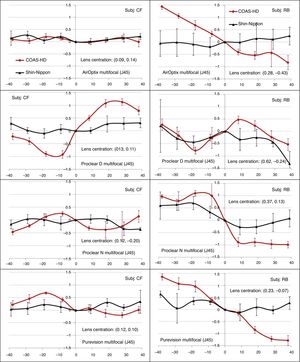
As can be seen in Fig. 3, the differences between the M measures obtained with both the instruments became more appreciable with the use of MFCLs. Overall, the COAS-HD measures were more positive for center-near designs (i.e. Proclear N, AirOptix MF and Purevision MF); while SN produced more positive results with center-distance multifocal design (Proclear D). These differences were however significant only in some peripheral locations for AirOptix multifocal and Proclear N design. The intra-subject variability was much greater in the measurements obtained from SN than those obtained with COAS-HD, especially true with SVCLs and MFCLs. The maximum within-subject variability for the SN instrument was about 2.54D while that for the COAS-HD was only 0.46D.
Line plots of the mean spherical equivalent (M) measures of two subjects CF (column 1) and RB (column 2), as function of horizontal visual field eccentricity when the test eye was corrected with different multifocal contact lenses. In the plot, (+) sign indicates nasal visual field, while (−) sign indicates temporal visual field. Error bars represent the standard deviations of the average within-subject variability.
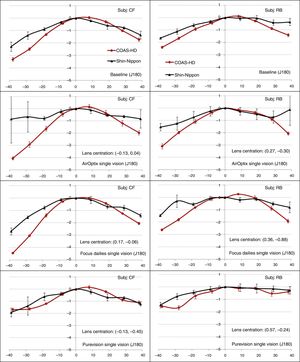
At baseline, the J180 measures obtained with the COAS-HD were more negative than those obtained with the SN for both subjects. This difference became more apparent as field angles increased. No obvious differences between instruments were noticed, in terms of asymmetry in the J180 measure between the temporal and nasal visual fields. As can be clearly seen in Fig. 4, for the test cases corrected with SVCLs there were considerable differences found between the J180 measures obtained with SN and COAS-HD across most field eccentricities, with the COAS-HD measures being more negative, except for the PureVision SVCL test case. The greatest difference in J180 was found at −40° for the AirOptix SV lens (ΔCF=3.20D, ΔRB=1.56D).
Line plots of the horizontal/vertical astigmatic component (J180) measures of two subjects CF (column 1) and RB (column 2), as function of horizontal visual field eccentricity, for baseline condition (unaided eye) and when the test eye was corrected with different single vision contact lenses. In the plot, (+) sign indicates nasal visual field, while (−) sign indicates temporal visual field. Error bars represent the standard deviations of the average within-subject variability.
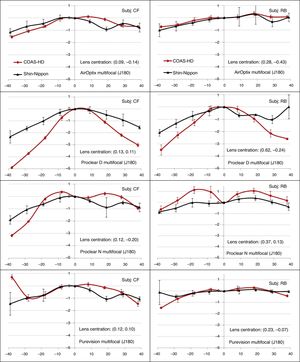
As can be seen in Fig. 5, the differences between the J180 measures obtained with both the instruments became more distinct with the use of MFCLs. Overall, the COAS-HD measures were more positive for center-near designs (i.e. Proclear N, AirOptix MF and Purevision MF), while SN produced more positive results with center-distance MFCL design (Proclear D). These differences were however significant only for Proclear D and N designs. The greatest difference of 2.58D and 1.39D, for subjects CF and RB, respectively, were measured with Proclear Distance at −40°. When compared with the baseline condition, all the center-near designs produced more positive results while the center-distant design produced more negative J180 measures with both the SN and the COAS-HD. The within-subject variability was much greater in the measurements obtained from SN than those obtained with COAS-HD, especially true with SVCLs and MFCLs. The maximum within-subject variability for the SN instrument results was about 1.95D while that for COAS-HD was only 0.53D.
Line plots of the horizontal/vertical astigmatic component (J180) measures of two subjects CF (column 1) and RB (column 2), as function of horizontal visual field eccentricity when the test eye was corrected with different multifocal contact lenses. In the plot, (+) sign indicates nasal visual field, while (−) sign indicates temporal visual field. Error bars represent the standard deviations of the average within-subject variability.
At baseline, the J45 measures obtained with SN were noticeably different to the respective measures obtained with COAS-HD, for both subjects. However, they were only significant for extreme visual field angles ≥30°. The asymmetry in the J45 measures between the temporal and nasal visual fields was more evident for subject RB.
As can be clearly seen in Fig. 6, there were only small differences found between the J45 measures obtained with SN and COAS HD across most field eccentricities, for the test cases corrected with all SVCLs, except when subject RB was corrected with Focus Dailies and PureVision SVCLs.
Line plots of the oblique astigmatic component (J45) measures of two subjects CF (column 1) and RB (column 2), as function of horizontal visual field eccentricity, for baseline condition (unaided eye) and when the test eye was corrected with different single vision contact lenses. In the plot, (+) sign indicates nasal visual field, while (−) sign indicates temporal visual field. Error bars represent the standard deviations of the average within-subject variability.
As shown in Fig. 7, the differences between the J45 measures obtained with both the instruments became more evident with the use of MFCLs, especially true for subject RB. The mean differences within both the instruments ranged between 0.10D and 1.50D. The greatest difference of 1.50D was found with AirOptix Multifocal in subject RB at −40°, where the COAS-HD measurement was more positive. Again, the within-subject variability was much greater in the measurements obtained from SN than those obtained with COAS-HD, especially true with SVCLs and MFCLs. The maximum within-subject variability for the SN instrument results was about 1.07D while that for COAS-HD was only 0.57D.
Line plots of the oblique astigmatic component (J45) measures of two subjects CF (column 1) and RB (column 2), as function of horizontal visual field eccentricity, when the test eye was corrected with different multifocal contact lenses. In the plot, (+) sign indicates nasal visual field, while (−) sign indicates temporal visual field. Error bars represent the standard deviations of the average within-subject variability.
The purpose of this pilot study was to compare the contributions of SVCL and MFCL to the PR profiles obtained with the SN and the COAS-HD instruments. Overall, the refractive components M, J180 and J45 obtained with SN and COAS-HD for baseline condition were considerably different only for field angles ≥30°, both in temporal and nasal directions. This is in agreement with previous studies confirming their interchangeable use for on-axis and peripheral refraction.9,10,18 However, when measuring through SVCLs or MFCLs, the two instruments can behave quite differently. Nevertheless, some patterns were noticed. In general, the J180 measures with the SN were considerably lower in magnitude than those acquired with COAS-HD. Further, the J45 measures obtained with the SN were noticeably different to the respective measures with the COAS-HD, both in magnitude and sign, with the differences ranging between 0.10D and 1.00D. These observations for J180 and J45 held true with both SVCLs and MFCLs. In addition, for some correcting CLs, a difference in the PR profiles was observed between the two subjects, which appeared to be associated with the CL centration with respect to HVID. The maximum within-subject variability (repeatability for the RPR measurements for test lenses at various field angles) for the SN instrument was 2.54D, 1.95D and 1.07D, for M, J180 and J45 components, respectively. However, the same measures for the COAS-HD were 0.46D, 0.53D, 0.57D (much lower), supporting the use of a Hartmann–Shack system over autorefractors, when performing peripheral refraction measurements through MFCLs.
The current study has only considered high-add multifocal CLs, however the authors believe that the results could be extrapolated to even low-add multifocal CLs, although the magnitude of differences are expected to be smaller. The designs considered in this study were limited to center-distance and center-near multifocal CLs and we believe that there could be more variability induced for concentric or zonal bifocal contact lenses.
In the interest of manuscript length and appropriate comparison with SN measures, the COAS-HD results were presented for the 3mm pupil analysis diameter. When the analysis was extended to 4mm diameter, there were small (0.50–0.75D) changes in almost all M, J180 and J45 components, Proclear® D and N lenses demonstrating the greatest dependency on the pupil analysis diameter. This greater dependency can be explained by the fact that the power profiles of the Proclear® D and N lenses exhibited the most distinctive steps from distance to near zones, when compared to the other MFCLs used in this study.19
Atchison10 found good agreement between his custom-built ‘visible’ Hartmann–Shack instrument and the Shin-Nippon SRW5000, with mean power differences in the range of 0.30–0.70D. He attributed the differences partly to the differences in the source wavelengths. Although, the commercial COAS-HD measures in the near-infrared – the software actually converts the measurements back into visible (555nm) wavelength, accounting for chromatic dispersion.20 Therefore, some of the differences observed in our case also could be partly explained by the wavelength differences. We note that the SN used in our study is newer than the SRW 5000 version; however we are not aware of any changes in its working principle. Nevertheless, this would only hold true to explain the differences observed in the unaided state. When the differences with SVCLs and MFCLs are considered, it would appear that they are more likely the effects of the instrument in combination with lens type and centration induced interactions.
Interestingly, SVCLs have produced significant alterations to the baseline peripheral refraction profiles. This can be explained by the fact that none of the SVCLs used have a linear power profile across the optic zone, i.e. are spherical aberration (SA) free. The three SVCLs used in this experiment were reported to have negative SA across the optic zone (i.e. increase in the negative power with increase in the semi-cord diameter). Amongst these, data for a −3.00D Rx suggests that the PureVision design has the greatest negative SA followed by the Focus Dailes.21,22 The AirOptix design however is claimed to have a ‘quasi-linear’ power profile with least negative SA.23 Although the lenses used here were −2.00D, the authors deem that the profiles should be comparable. In some occasions, the trends discussed above have been reflected in the results of single vision CLs, for example: the M measures through PureVision CL with respect to the baseline were always seen to be relatively more hyperopic.
It is worth noting that amongst the center-near MFCLs used, Proclear N design had the most pronounced effect on the peripheral refraction profile, gauged in terms of M. Also, in general, all center-near MFCLs produced relative more positive J180 measures from baseline and in some instances absolute positive J180 measures, particularly with the Proclear N design. Absolute positive J180 values, an indication that the axis of astigmatism is either less than 45° or greater than 135°, are quite uncommon for horizontal peripheral refractions. These surprising results could plausibly be explained by its inherent optical design, which has a 1.70mm diameter central near zone followed by a blending zone into the 8.50mm diameter peripheral distant optic zone (Source: Manufacturer's fitting guide). When compared to the other MFCLs used in this study, the Proclear N design has a distinctively smaller near zone and a more pronounced step from central near to peripheral distance zones.19
For non-astigmatic eyes, the J45 power vector is expected to be close to zero, indicating that the axis of astigmatism is along the principle meridians. However, most reported PR measurements have values as large as 0.75D. This is likely due to some degree of oblique/eccentric viewing or inaccurate instrument alignment. In this study, J45 measures are up to 1.5× greater, in particular when measuring through SVCLs or MFCLs. This appears to be caused by vertical or oblique CL decentration; as such values were only seen in the participant RB, where on average the correcting CLs decentered more than on subject CF.
The literature on peripheral refraction measurements using autorefractors and aberrometers suggests that both these techniques can be interchangeably employed with confidence to measure peripheral refraction in human participants.9,10,18 The current work suggests that this may only be valid when considering unaided eyes or eyes corrected with lenses with minimal spherical aberration. For eyes fitted with MFCLs or other lenses with considerable amounts of SA, the use of autorefractors like the SN may generate unreliable results.
With the small subject size (n=2) and no gold standard being available to calibrate peripheral refraction results from either instrument for absolute accuracy, no definitive conclusions can be drawn with regards to instrument preferences. Nevertheless, all the indications from this pilot study are, that the SN generates more variable results for eyes fitted with MFCLs, or for that matter any lens with significant levels of SA, and PR data from that instrument should be treated with some degree of caution.
ConclusionFor most test conditions with the exception of baseline measures, distinct differences were observed between the PR measures obtained with the two modified instruments, SN and COAS-HD. The differences varied as a function of CL design, correcting CL centration and pupil analysis diameter. Although the pilot study supports the interchangeable use of the two instruments for on- and off-axis refraction in unaided eyes or eyes corrected with low or no spherical aberration contact lenses; it advocates the use of the COAS-HD over the SN when refracting through MFCLs.
Conflicts of interestThe authors have no conflicts of interest to declare.
The authors thank Ms. Rebecca Weng for her participation in the study and Dr. Thomas John for statistical advice. This work was presented in part at the American Academy of Optometry (2011) at Boston, USA.