We present four young patients with acute severe solar retinopathy after observation of the total eclipse on January 4, 2011 without appropriate eye protection. Funduscopic findings were accompanied by optical coherence tomography (OCT) investigation of the macula. All our patients were young (range 14–29 years). In three of the four patients we have been able to repeat OCT evaluation revealing that the retinal changes were reversible, but delineating mild pathology in the retinal pigment epithelium and photoreceptors. Best-corrected visual acuity in the fourth case was 6/24. In addition, macular edema, which has been previously described in literature, could not be demonstrated by OCT. In the two cases we performed an early fluorescein angiogram, no pathology was seen.
Presentamos cuatro pacientes jóvenes con retinopatía solar severa y aguda, tras la observación de un eclipse total el 4 de Enero de 2011, sin protección ocular adecuada. Los hallazgos funduscópicos se acompañaron de una prueba de tomografía de coherencia óptica (TCO) de la mácula. Todos nuestros pacientes eran jóvenes (rango 14–29 años). En tres de los cuatro pacientes pudimos repetir la prueba de TCO, que reveló que los cambios en la retina eran reversibles, pero subrayaron una patología leve en el epitelio pigmentario retiniano y los foto-receptores. La agudeza visual mejor corregida último caso fue de 6/24. Además, no se pudo demostrar el edema macular mediante la TCO, que ha sido previamente descrito en la literatura. En los dos casos en que realizamos un angiograma fluoresceínico no se observó patología alguna.
Visual deterioration caused by watching a solar eclipse has been recognized from the time of Plato. Solar retinopathy is a well-recognized clinical entity of retinal damage caused by viewing the sun, induced by a photochemical process that may be enhanced by elevated tissue temperature. Although most cases are commonly attributed to solar eclipse viewing, damage from sun gazing has also been described in religious ritual participants, military personnel, people with mental disturbances, sunbathers and forced sun gazing.1–7 As demonstrated in histopathological studies of solar retinal lesions, sun gazing causes fine structural anomalies in the outer segments of the photoreceptors and the retinal pigment epithelium (RPE) cells of the macula.8 Symptoms usually develop within 1–4h after exposure and include decreased vision, metamorphopsia, micropsia, and central or paracentral scotomas. Fundus examination typically shows a small yellow spot with a surrounding gray zone in the foveolar or parafoveolar area. Spontaneous evolution leads to the improvement of visual acuity.9–11
We present four young patients with acute severe solar retinopathy after observation of the total eclipse on January 4, 2011 without appropriate eye protection. Funduscopic findings were accompanied by optical coherence tomography (OCT) investigation of the macula.
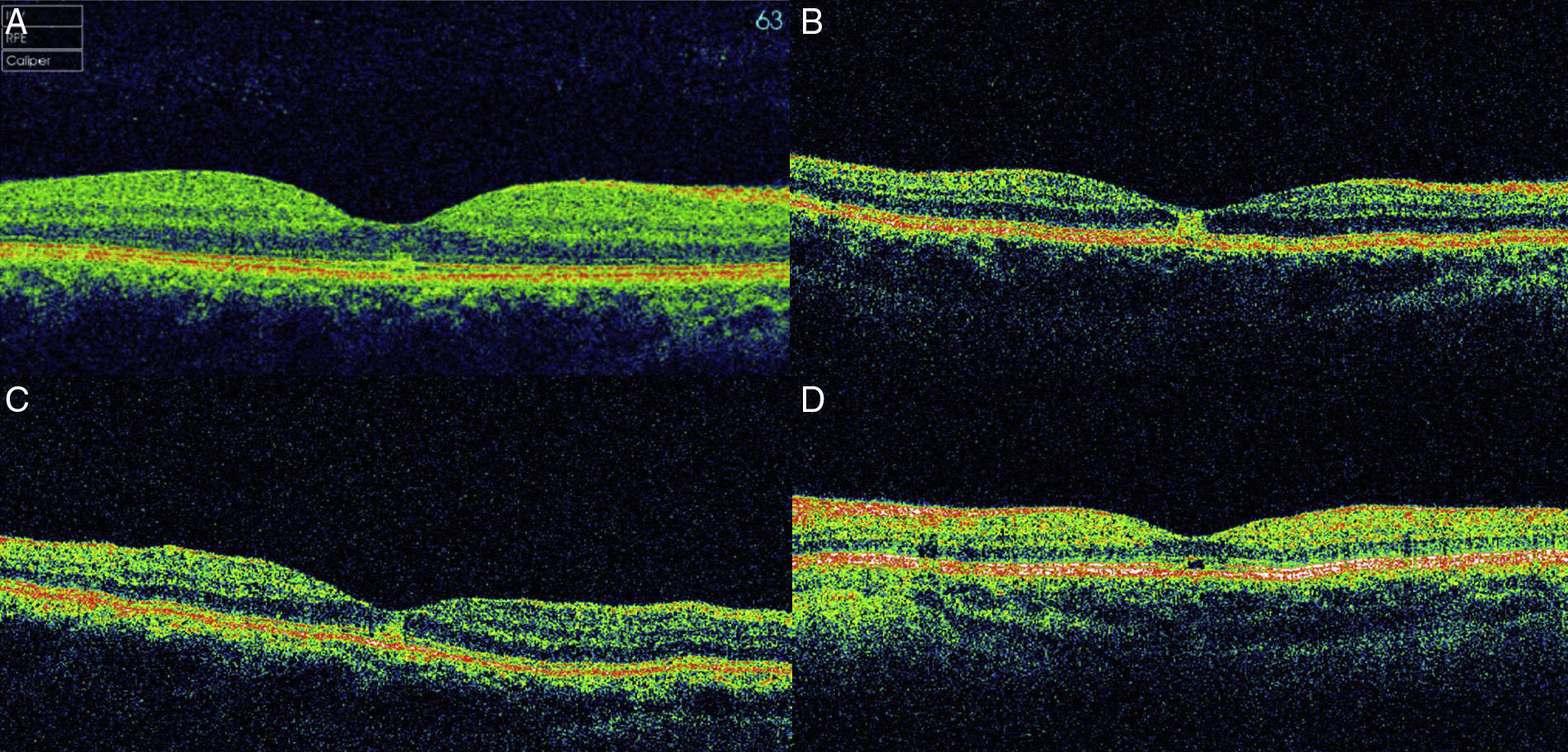
Patient descriptionsCase 1A 29-year-old man presented with complaints of blurred vision affecting the right eye. The onset of symptoms was one day prior to presentation, when he had gazed at the eclipse without eye protection for a few minutes. On initial examination the best corrected visual acuity (BCVA) was 6/12 OD and 6/6 OS. Slit lamp fundus examination showed a small foveal defect in the right eye. Fluorescein angiography (FA) appeared normal with no hyperfluorescence. Spectral domain OCT (3D OCT-2000 Topcon, Tokyo, Japan) showed a small disruption in the inner segment-outer segment (IS/OS) band in the right fovea (Fig. 1A) and no abnormalities in the left eye. One week later BCVA was 6/9. Three months later BCVA returned to 6/6. No pigment abnormalities were observed in the right macula.
Optical coherence tomography (OCT) images of cases at presentation. In case 1 (A, spectral domain 3D OCT-2000, Topcon, Tokyo, Japan), there is a small disruption in the inner segment-outer segment (IS/OS) band in the fovea. In case 2 (B, time-domain Stratus OCT, Carl Zeiss Meditec, USA), a hyper-reflective area in the fovea affecting all retinal layers without increase in retinal thickness is detected. In case 3 (C, time-domain Stratus OCT, Carl Zeiss Meditec, USA), a small hyper-reflective area at the fovea can be appreciated. In case 4 (D, time-domain Stratus OCT, Carl Zeiss Meditec, USA), there is a defect in the inner hyper-reflective layer of the fovea.
A 29-year-old woman presented with complaints of central scotoma and blurred vision of the right eye after watching the eclipse without eye protection two days before seeking examination. According to the patient, the exposure time was just a few seconds. On presentation BCVA was 6/12 OD and 6/6 OS. Fundus examination showed a small yellow round lesion in the fovea of right eye. Time-domain OCT (Stratus OCT, Carl Zeiss Meditec, Dublin, CA, USA) examination of the right eye showed a hyper-reflective area in the fovea affecting all retinal layers without increase in retinal thickness (Fig. 1B). FA was normal bilaterally. One month after the exposure BCVA was 6/6. Six months after the exposure BCVA remained 6/6. A small reddish demarcated spot was detected at the fovea. The revised OCT showed a very small hypo-reflective area at the inner hyper-reflective layer in the center of fovea.
Case 3A 13-year-old female presented 48h after direct viewing of the eclipse for a few seconds with both eyes opened. BCVA was 6/6 in both eyes. Fundus examination of both eyes did not show any pathology. Time-domain OCT (Stratus OCT, Carl Zeiss Meditec, Dublin, CA, USA) showed a small hyper-reflective area at the right fovea (Fig. 1C) that returned to normal three weeks later. BCVA remained 6/6 without subjective complaints.
Case 4A 14-year-old girl came to our Emergency Department four days after watching the solar eclipse, reporting blurred vision in the right eye. BCVA was 6/24 OD and 6/6 OS. A right central foveal defect was seen on examination. Time-domain OCT (Stratus OCT, Carl Zeiss Meditec, Dublin, CA, USA) showed a defect in the inner hyper-reflective layer of the right fovea (Fig. 1D). One year after the exposure, BCVA remains 6/24 and pigmentary foveal changes are seen clinically.
DiscussionSolar retinopathy is characterized by involvement of the outermost layers of retina. The RPE absorbs an important percentage of solar radiations with an ensuing increase of tissue temperature in surrounding areas, thus producing thermal damage. On the other hand high energy waves and low levels of ultraviolet A (UVA) or radiations close to UVA (320–400nm) are responsible for photochemical damage. It is generally believed that retinal involvement could be the result of the combination of thermal and photochemical damage. Solar radiation produces pointed damage in apical melanosomes of the RPE followed by alterations in the outermost segment of foveal photoreceptors.12–14
Solar retinopathy presents soon after initial exposure, with symptoms including reduced visual acuity, central scotomas, chromatopsia, photophobia, and metamorphosia. It is acutely characterized by a yellow foveolar lesion upon fundus examination. The main reported OCT finding was a hyper-reflective area involving all foveolar retinal layers without showing any sign of retinal edema. It correlates in size and location with the characteristic funduscopically visible yellow dot. At present, the origin of this well delineated area of hyper-reflectivity is unclear.11
All our patients were young (range 14–29 years). In three of the four patients we have been able to repeat OCT investigation revealing that the retinal changes were reversible, but delineating mild pathology in the retinal pigment epithelium and photoreceptors. BCVA in the fourth case remained 6/24. In addition, macular edema, which has been previously described in literature, could not be demonstrated by OCT. In the two cases we performed an early FA and no pathology was seen.
Recently fundus autofluorescence (FAF) has emerged as complementary non-invasive diagnostic tool in the management of retinal disease. FAF is based on the autofluorescent properties of retinal fluorophores, such as lipofuscin, which is mainly located in the RPE.13 Reduced content of lipofuscin in the RPE has been described in cases of light-induced loss of photoreceptors. In cases with presumed idiopathic outer lamellar defects at the fovea, e.g. chronic solar retinopathy, there is a characteristic autofluorescence pattern consisting of small areas of decreased autofluorescence, corresponding in location to the outer lamellar defects, surrounded by a ring of faint increased autofluorescence in the context of the relatively hypoautofluorescent macular area.15–20
This case series show that direct eclipse viewing without adequate eye protection can result in acute solar retinopathy. Public awareness and educational campaigns are essential. Permanent visual loss is still an area of concern. In many cases the changes are reversible, but solar retinopathy can lead to lasting visual impairment (case 2). OCT is an excellent modality for demonstrating macular pathology caused by solar retinopathy, and is superior to FA in demonstrating these changes. OCT can detect subclinical retinal changes as seen in case 3.
Conflicts of interestThe authors have no conflicts of interest to declare.